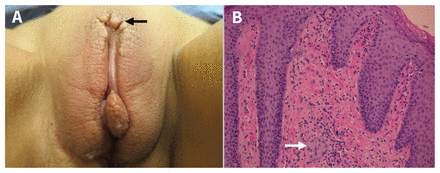
A 35-year-old woman with a 15-year history of gastrointestinal Crohn disease presented to a multidisciplinary vulvar clinic with an 18-month history of symptomatic vulvar bumps. She reported intermittent vulvar pain and swelling. A superficial skin biopsy performed 2 years earlier by her family physician had shown only mild keratosis. The lesions had been treated unsuccessfully with trichloroacetic acid for presumed condylomata. Findings on clinical examination included bilateral labial edema, thickening of the labia majora and minora and flesh-coloured papules (Figure 1A). These findings were suggestive of acquired lymphangectasia from vulvar Crohn disease, supported by the presence of noncaseating granulomas on biopsy (Figure 1B). The lesions responded well to CO2 laser vapourization. Since the patient had also been recently started on vedolizumab for her gastrointestinal Crohn disease, this may eventually improve the vulvar edema.
(A) Photograph of the vulva of a 35-year-old woman with bilateral labial swelling and edema, thickening of the labia majora and minora, and a well-defined plaque of flesh-coloured papules (2–3 mm) on the upper labia majora (black arrow) and on the edge of the lower right labia majus, suggestive of acquired lymphangectasia secondary to vulvar Crohn disease. (B) Photomicrograph from a vulvar biopsy illustrating a noncaseating granuloma (white arrow), suggestive of vulvar Crohn disease (hematoxylin and eosin stain, 200 × magnification).
Vulvar Crohn disease is uncommon, but it can adversely affect quality of life, and is often under-recognized and misdiagnosed. 1–3 The median time to diagnosis of vulvar Crohn disease is 3.5 years, as patients often see multiple specialists before a diagnosis is established.2 Although most patients (50%–80%) with this condition have underlying gastrointestinal Crohn disease, not all patients with vulvar Crohn disease will go on to develop bowel disease.1,2
Nonspecific associated gynecologic symptoms, such as itch, make the diagnosis challenging.2 Vulvar findings include edema, labial hypertrophy, lymphangiectasia, knife-like fissures, ulcerations, abscesses and fistulas.1–3 Histological findings, such as the presence of noncaseating granulomas, granulomatous vasculitis or lymphangitis in the dermis, support the diagnosis.1–3 Other diagnoses to consider in presentations similar to our patient’s include skin tags, condylomata, molluscum contagiosum, vulvar intraepithelial neoplasia and acquired lymphagiectasia.4
Vulvar Crohn disease is a chronic disease that involves long-term medical (e.g., antibiotics, systemic corticosteroids or anti–tumour necrosis factor-α therapies) or surgical (CO2 laser ablation, excision) management.2 It may be challenging to manage and it benefits from a multidisciplinary approach, involving gastroenterologists, gynecologists, pathologists and dermatologists.1,2 In patients with known Crohn disease and abnormal vulvar findings, the possibility of underlying vulvar Crohn disease should be considered.3
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
The authors have obtained patient consent.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/