A 77-year-old man with vascular dementia presented to the emergency department with dyspnea. His medical history included rheumatic mitral stenosis with mechanical mitral valve replacement in 2001. On examination, he was afebrile, jaundiced and euvolemic. On auscultation we heard a new holosystolic murmur, loudest at the apex. Laboratory investigations revealed low hemoglobin of 89 (normal 125–170) g/L, mean corpuscular volume 98.9 (normal 80–100) fL, a normal platelet count, undetectable haptoglobin level, and elevated lactate dehydrogenase (1603 [normal 99–167] U/L), bilirubin (total 45 [normal < 15] μmol/L; direct 19 [normal < 5] μmol/L) and reticulocyte counts (42.9%, normal 1.5%–15%). A direct antiglobulin test (DAT [Coombs test]) was negative. We saw numerous schistocytes on peripheral blood smear (Figure 1). A transthoracic echocardiogram showed dehiscence of the prosthetic mitral valve posteriorly, with substantial paravalvular mitral regurgitation not present on echocardiogram 5 months earlier (Appendix 1, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.202620/tab-related-content). The patient’s left ventricular ejection fraction was 50%–55%. Negative blood cultures, coupled with the absence of fever or other infectious findings, made endocarditis unlikely. The patient was given a diagnosis of macroangiopathic hemolytic anemia secondary to prosthetic valve dehiscence. He was managed conservatively, owing to his poor baseline functional status.
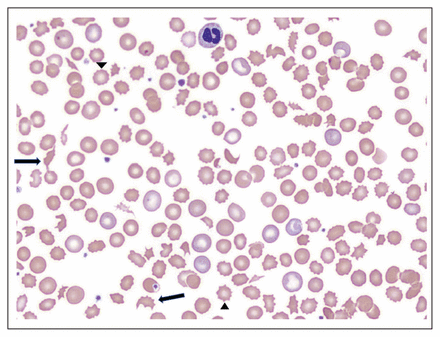
Peripheral blood smear of a 77-year-old patient with a mechanical mitral valve who presented with hemolytic anemia. The smear shows numerous schistocytes (arrows), acanthocytes (arrow-heads), and a normal platelet count.
Valve-associated hemolytic anemia has been reported in as many as 1% of patients with prosthetic valves.1 The pathophysiology involves paravalvular regurgitation causing mechanical trauma to red blood cells. Clinical features include jaundice and a new murmur. The blood smear typically indicates numerous schistocytes and a normal platelet count. Other laboratory findings include an elevated lactate dehydrogenase, bilirubin and reticulocyte count with low haptoglobin. In patients with a prosthetic valve who present with anemia, it is important to consider valve-associated hemolysis in the differential diagnosis. Initial workup should include a blood smear, DAT and transthoracic echocardiography to assess prosthetic valve function. If evidence of paravalvular regurgitation exists, definitive management is either percutaneous paravalvular leak closure or surgical repair. Medical and supportive measures (transfusions, folic acid supplementation) may be helpful in the short term.2
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
The authors have obtained consent from the patient’s family.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/