A previously healthy 34-year-old woman presented to her family physician with an asymptomatic erythematous rash on her hands that had been present for several weeks. She had elevated levels of alanine transaminase, alkaline phosphatase and γ-glutamyltransferase, compatible with a diagnosis of primary biliary cholangitis. Because the morphology of the lesions was atypical, the patient was referred to a dermatologist.
There were well-circumscribed, red-orange, waxy plaques on the patient’s palms and soles, compatible with a diagnosis of pityriasis rubra pilaris (Figures 1A and 1B). Because of the plaques, it was unlikely to be palmar erythema secondary to hepatic disease, although psoriasis was a possibility. Results for HIV testing were negative. A biopsy supported the clinical impression of pityriasis rubra pilaris (Appendix 1, available at www.cmaj.ca/lookup/suppl/doi:10.1503/cmaj.190961/-/DC1).
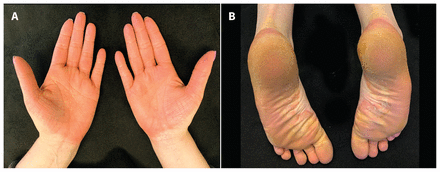
(A) Confluent, red-orange, waxy plaques on the palmar aspects of the hands of a 34-year-old woman with pityriasis rubra pilaris. (B) Similar red-orange plaques on the plantar aspects of the feet.
Pityriasis rubra pilaris is a cutaneous disease of unknown cause. It can be classified into 6 subtypes based on morphology, age of onset and HIV status,1 and although the prognosis of pityriasis rubra pilaris varies with subtype, it typically resolves within 3–5 years.1 Waxy keratoderma is a distinctive feature of all types of pityriasis rubra pilaris1 presenting with acral involvement, the texture being likened to carnauba wax. Waxiness is not a feature of non-acral pityriasis rubra pilaris.1 The association with primary biliary cholangitis is uncommon; therefore, the significance of the presence of primary biliary cholangitis in this patient is uncertain.2
Investigations should include a biopsy and testing for levels of liver enzymes and HIV serology. Acitretin is the first-line treatment, but alternative treatments include topical steroids, phototherapy, methotrexate and tumour necrosis factor-α inhibitors.3
The patient’s pityriasis rubra pilaris was treated with topical steroids, as systemic treatment was contraindicated, together with ursodiol for her primary biliary cholangitis. At a 4-week follow-up, her plaques had improved, thinning by about 50%.
Acknowledgement
We wish to thank Dr. Amy Thommasen for the histopathology image as well as her expert opinion.
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
The authors have obtained patient consent.