A 21-year-old man with a history of Kawasaki disease at the age of 5 years came to hospital with acute-onset chest pain. He denied any illicit drug use and reported that he had not taken ASA for about 2 years. His initial ECG documented lateral-lead ST-wave depression; blood tests showed an elevated level of creatine kinase. The diagnosis was non–ST-elevation myocardial infarction. With ASA, clopidogrel, and intravenous nitrates and low-molecular-weight heparin, his symptoms abated by 6 hours after onset.
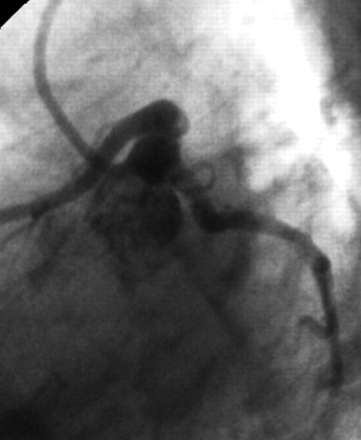
Fig. 1: Coronary angiogram showing the patient's thrombotic lesion (arrow) in the ostial circumflex artery.
Diagnostic coronary angiography revealed an aneurysmal left main coronary artery with a thrombotic lesion in the circumflex artery that blocked 75% of its cross-sectional area (Fig. 1). Thrombosuction reduced the stenosis. Intravascular ultrasound (IVUS) to better define the lesion showed focal, eccentric narrowing; the rest of the ostial circumflex artery appeared normal (Fig. 2). A 3.5 × 16 mm bare-metal stent was placed across the ostial stenosis and postdilated with a 4 × 9 mm balloon. Coronary angiography (Fig. 3) and repeat IVUS showed adequate stent apposition with a minimum luminal area of 15.5 mm2. The patient had an uneventful recovery and was discharged home 2 days later with prescriptions for ASA (100 mg), clopidogrel (75 mg) and warfarin (3 mg), intended to achieve a target international normalized ratio of 2–2.5.
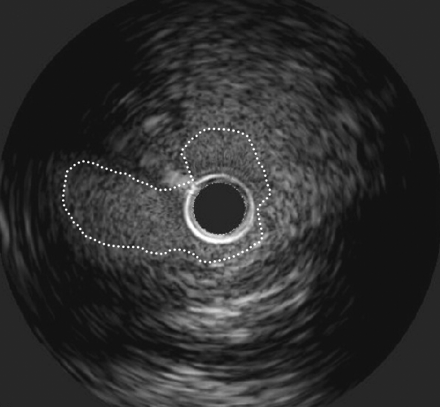
Fig. 2: Eccentric narrowing (outline) of the left circumflex artery, as shown with intravascular ultrasound.
Fig. 3: Final coronary angiogram documenting a resolution of the ostial circumflex stenosis.
Mucocutaneous lymph-node syndrome, also called Kawasaki disease, is a childhood illness with an onset typically between infancy and 10 years of age. Its cause is not well understood. The acute phase usually lasts 2 weeks, with clinical manifestations that generally include fever, polymorphous rash, bilateral conjunctival injection, changes in the mucous membranes and extremities, and lymphadenopathy.1 During the acute stage, coronary aneurysms have been known to rupture; intravenous gamma globulin, which in treatment plays an immunomodulatory role, has been shown to reduce the risk of a coronary aneurysm from 20% to 5%. Thrombus formation is another complication, particularly giant aneurysms (> 8 mm). High-dose ASA (75–100 mg/kg daily) is given concurrently for its anti-inflammatory properties, typically until the acute phase is over and test results for inflammatory markers have entered their normal ranges.
Unfortunately, Kawasaki disease can have longer-term cardiac effects. Aneurysms may regress in size over time, but about 20% will form clinically significant stenoses. About half of all patients with giant aneurysms develop arterial stenosis or complete obstruction, and about two-thirds of these experience a myocardial infarction.2,3 These events may occur years after the original manifestion of the disease.
Low-dose ASA (3–5 mg/kg per day) is maintained until the acutely affected child shows no echocardiographic evidence of arterial changes, usually within 2 months after disease onset. Those with demonstrated abnormalities of their coronary artery will take low-dose ASA indefinitely. For those with giant aneurysms, ASA is used in combination with warfarin. Owing to the rare association of Reye's syndrome (liver dysfunction with encephalopathy) with ASA among children infected with influenza or varicella, yearly flu vaccination is recommended for those taking ASA for long periods. Patients or the responsible adults are also advised, if exposure to influenza or varicella is suspected, to contact their physician promptly to give the clinician the opportunity to advise stopping the ASA temporarily.
Footnotes
-
Competing interests: None declared.