Consulting pharmacists
Figure. Photo by: Smithsonian Institution Libraries
Many elderly people take multiple medications, which increases the potential for inappropriate dosing, drug interactions and adverse drug reactions. Community pharmacists may be able to help family physicians manage their patients' drug therapy. John Sellors and colleagues report the results of a randomized controlled trial in which patients in family physicians' practices assigned to the intervention group had a structured medical assessment carried out by a pharmacist; the pharmacist then advised the patient's physician about drug-related problems and recommended corrective steps. Patients in control practices received usual care from their physicians. The intervention did not have a significant effect on patient outcomes, but physicians were receptive to the pharmacists' recommendations to resolve drug-related problems. In a related commentary, Sumit Majumdar and Stephen Soumerai suggest reasons for the lack of effect and say that further research is warranted to test other community-based pharmaceutical care interventions, because improvements in the quality of prescribing are urgently needed.
Predicting dropout from and readmission to a detoxification unit

Figure. Photo by: Health Canada
Substance abuse threatens the health and quality of life of many Aboriginal people. Russell Callaghan reviewed the medical charts of First Nations people admitted to an inpatient detoxification unit in British Columbia in order to develop a model to predict treatment dropout and readmission. Self- referral and a preferred drug of choice other than alcohol were weakly associated with dropout from the program. A previous history of admission to the unit was the strongest predictor of readmission.
See page 23
Percutaneous coronary intervention: Expand access at any cost?
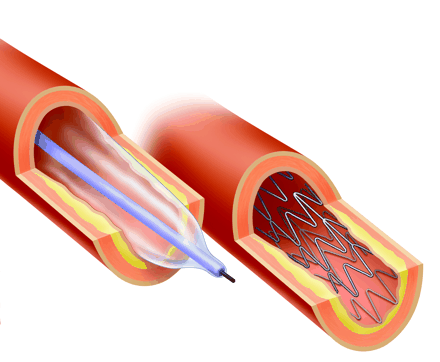
Figure. Photo by: Christine Kenney
The treatment of ST-segment elevation myocardial infarction evolved from bedrest in the 1960s to the use of thrombolytic agents as the standard of care by the late 1980s. Percutaneous coronary intervention (PCI), a mechanical intervention to re-establish patency in infarct- related vessels, is at the front of a new wave of innovations. However, to be effective, PCI must be done as soon as possible after myocardial infarction. But are the costs of expanding this high-technology treatment beyond large urban centres warranted? In this issue, 2 groups of authors offer different perspectives. Madhu Natarajan and Salim Yusuf raise practical questions about expanding access to PCI and comment that cost-effectiveness must be a consideration. William Ghali and colleagues argue that the data in support of PCI are so impressive that cardiac care providers and health care system decision-makers should work to provide round-the-clock access to PCI to increasing numbers of patients.











