A 75-year-old man had a 3-year history of increasing weakness and fatiguability. He had also noticed bilateral foot and leg swelling over the last year, followed by 1 month of abdominal distension and shortness of breath on exertion. He had no history of heart disease, hypertension, diabetes, smoking, tuberculosis or alcohol abuse and no other cardiac, respiratory, gastrointestinal or constitutional symptoms.
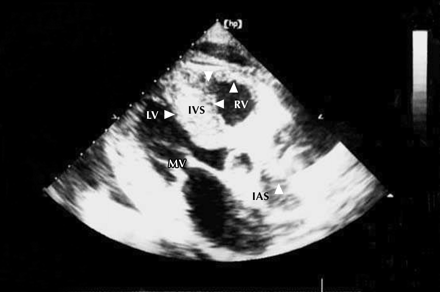
The man's vital signs were normal, but his jugular venous pulse was 6 cm above the sternal angle. The results of his chest and precordial examination were normal, except for a mild left parasternal systolic ejection murmur. He had mild hepatomegaly and moderate ascites. Aspirated peritoneal fluid was transudative, and cytology and cultures were negative. His blood values were unremarkable, and a chest radiograph demonstrated only mild cardiomegaly. An ECG showed low-voltage QRS complexes with nonspecific intraventricular conduction defects. A 2-D echocardiogram (Fig. 1) revealed symmetrical thickening of the left ventricular (LV) and right ventricular (RV) walls, interventricular septum (IVS) and interatrial septum (IAS). The myocardium had a diffuse, hyperreflectile “granular sparkling” appearance (arrows). Ventricular cavity constriction, atrial dilatation, and diffuse thickening of the tricuspid valve (not shown) and mitral valve (MV) were noted. Systolic function was normal, and there was no pericardial effusion. Cardiac amyloidosis was suspected, however, Congo-red-stained biopsies of the patient's abdominal fat pad, rectum and gingiva were negative. Urine and serum electrophoresis and a bone marrow biopsy looking for plasma cell dyscrasias were also negative. The patient was diagnosed with isolated primary cardiac amyloidosis and was started on oral prednisolone, with melphalan added 4 weeks later. Unfortunately, the patient developed increasing congestive heart failure and died 10 months later.
Figure 1. Photo: Image courtesy of Dr. Amitabh Monga
Cardiac amyloidosis, or “stiff heart syndrome,” occurs when amyloid protein slowly replaces normal myocardial tissue. Some degree of cardiac amyloidosis is common in elderly people (detected incidentally in 20%–40% of routine post mortems), but it is rarely clinically significant.1,2
Primary (or amyloid light-chain [“AL type”]) cardiac amyloidosis is caused by “amyloidogenic” immunoglobulin from the bone marrow (plasma cell dyscrasias). It rarely involves only the heart and can occur without clear evidence of a plasma cell dyscrasia.3,4 Long-standing infections, chronic inflammatory diseases and, sometimes, cancer can cause “secondary amyloidosis,” also known as “AA type” because serum amyloid protein A is involved. AA type amyloidosis primarily affects the kidneys, liver, spleen and, sometimes, the heart.5 A subtype of secondary amyloidosis, “senile amyloidosis,” commonly affects the heart and blood vessels.6
Cardiac amyloidosis causes a restrictive cardiomyopathy with slow ventricular filling and abnormal relaxation, leading to significant diastolic dysfunction but preserved systolic function. Although some patients are asymptomatic, progressive fatigue, reduced activity tolerance and breathlessness on exertion are common. Signs of right heart failure often develop. Excessive nocturnal urination and orthopnea, angina or cardiac rhythm disturbances can sometimes occur. The differential diagnosis of cardiac amyloidosis includes constrictive pericarditis. However, low-voltage QRS complexes on ECG, a restrictive pattern on transmitral Doppler blood flow and a “sparkling” myocardium on 2-D echocardiography (Fig. 1) are characteristic of cardiac amyloidosis.7 Endomyocardial biopsies are sometimes falsely negative.8 The sensitivities of biopsies to detect systemic amyloidosis range from 50% for bone marrow aspirates to 70% for those of the skin and subcutaneous fat, and 80% for those of the rectum and gums. The need for biopsies can be avoided by localizing affected organs with an 123I-labelled serum amyloid P scintigraphic scan.9
Digitalis, calcium channel blockers and β-blockers are contraindicated in amyloid-associated cardiomyopathy, because they bind easily to amyloid fibrils, causing toxicity at apparently therapeutic levels.10 Pacemakers are sometimes needed for patients with symptomatic bradycardia. Cytotoxic and immunosuppressive drugs directed at plasma cell dyscrasias have been used to treat primary cardiac amyloidosis, but are often ineffective.11 The prognosis for patients with primary cardiac amyloidosis is poor, with death often occurring within 6 months of onset from congestive heart failure. In secondary amyloidosis, aggressive treatment of the underlying infection or inflammatory or neoplastic disease can improve symptoms and slow progression of the disease.12
Sandeep Arora Anju Arora Ravinder P.S. Makkar Amitabh Monga Department of Medicine Sitaram Bhartia Institute of Science and Research New Delhi, India