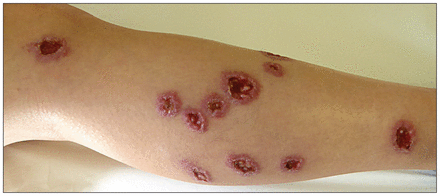
A 27-year-old healthy woman presented to the medical centre with a one-month history of widespread skin lesions with slow clinical progression. The lesions appeared on her thighs, shins, lower abdomen and left arm three weeks after she had travelled to an area endemic for Leishmania major in southern Israel. The lesions comprised violaceous tender nodules (0.5–1 cm in diameter) with central ulceration and crust (Figure 1). A skin smear showed Leishmania amastigotes (Appendix 1, available at www.cmaj.ca/lookup/suppl/doi/10.1503/cmaj.151115/-/DC1).
Multiple ulcers (0.5–1 cm in diameter), each surrounded by a violaceous hue, on the right shin of a 27-year-old woman who recently returned from travelling in southern Israel.
Leishmaniasis is a protozoan disease that is spread by the bite of infected female sand flies. Two million cases occur annually worldwide, mostly as cutaneous and mucocutaneous infections.1 The disease is present in all continents and is endemic in 88 countries.2 This parasitic disease is divided into Old World leishmaniasis, which is endemic in Asia, Africa, the Middle East and southern Europe, and New World leishmaniasis, which is endemic in Central and South America.1 With increased travel to endemic areas, the disease is encountered more often in tourists and is regarded as one of the 10 leading diseases among tourists returning from tropical countries.3
Erythematous nodules that gradually ulcerate and develop a central keratotic plaque are characteristic of leishmaniasis. These lesions spontaneously resolve over a period of months and often leave atrophic scars.1 Leishmaniasis is usually localized to one area of the body, with a few lesions.1 However, multiple bites can result in widespread multilesional disease requiring systemic treatment (e.g., sodium stibogluconate, miltefosine, liposomal amphotericin B), and familiarity with such cases can facilitate diagnosis. Treatment is often unsatisfactory, and varies in different centres owing to a lack of well-controlled studies.1
We started the patient on treatment with intravenous sodium stibogluconate. Although her lesions were improving, we stopped intravenous treatment because test results showed she had elevated liver enzymes. With intralesional injections of the medication, the lesions healed completely, leaving residual scarring.
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
The authors have obtained patient consent.