Left atrial–esophageal fistula is a deadly complication of atrial ablation
Percutaneous and surgical ablation of atrial fibrillation is common worldwide. Because the esophagus is adjacent to the posterior wall of the left atrium, it is susceptible to thermal injury during ablation procedures. This may result in the development of a left atrial–esophageal fistula. Although case series have suggested a low prevalence (< 0.001%–1.2%) of this complication,1,2 mortality rates, including rates among patients who receive treatment, are high (67%–100%).3,4 Procedural modifications have been introduced to reduce the likelihood of this complication, but this has not eliminated the risk. Periprocedural proton-pump inhibitors are advocated to minimize gastric acid exacerbation of thermal injury.5
A high index of suspicion is necessary after ablation
Case series report the onset of symptoms between 3–41 days after ablation.3 Symptoms are frequently nonspecific. Dysphagia, odynophagia and gastrointestinal bleeding have been reported.3 Fever, leukocytosis and bacteremia may be present and misdiagnosed as endocarditis.3 Neurologic symptoms, including subacute emboli (septic, thrombotic or air), cerebritis or meningitis, have been reported in about 70% of cases.3
Computed tomography is the preferred diagnostic test
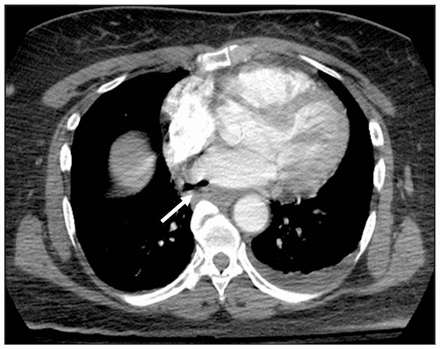
Computed tomography of the chest with intravenous contrast is the preferred diagnostic test.6 Loss of clear delineation between the esophagus and adjacent mediastinal structures may be noted. The presence of intravenous contrast in the esophagus confirms a fistulous connection; this is a specific, but infrequent sign. Air in the mediastinum or cardiac chambers may be seen (Figure 1).
Computed tomography of the chest showing pneumomediastinum (arrow).
If a fistula is suspected, esophageal manipulation should be avoided
If a fistula is suspected, esophageal manipulation with transesophageal echocardiography, esophagogastroduodenoscopy, nasogastric tube placement or oral contrast imaging should be avoided because catastrophic embolism or bleeding may occur under increased esophageal pressure.
Prompt surgical intervention is essential
The prognosis is dependent on prompt recognition and diagnosis. Once a fistula is identified, immediate surgical repair is required to improve survival and minimize morbidity.4,5 A multidisciplinary approach (preferably with a predefined plan) including cardiologists, cardiothoracic surgeons, gastroenterologists, radiologists, neurologists and infectious disease specialists is essential to optimize patient outcome.
Footnotes
-
Competing interests: Isabelle Nault has served as a consultant for Bayer and has received payment for lectures from Bayer and Sanofi. No competing interests declared by Sheldon Singh.
-
This article has been peer reviewed.