Interval for bone mineral density testing
The baseline T score is the most important determinant of the interval for bone mineral density (BMD) testing, say the authors of a prospective cohort study. Almost 5000 women 67 years of age or older with a normal BMD score or osteopenia at baseline were followed for up to 15 years. The BMD testing interval was defined as the estimated time for osteoporosis to develop in 10% of women before a hip or vertebral fracture occurred and before treatment for osteoporosis was initiated. The estimated BMD testing interval (with adjustment for estrogen use and risk factors) was 16.8 years (95% confidence interval [CI] 11.5–24.6) for women with normal BMD, 4.7 years (95% CI 4.2–5.2) in women with moderate osteopenia and 1.1 years (95% CI 1.0–1.3) in those with advanced osteopenia. These results suggest that screening intervals could vary depending on the T score at baseline. See N Engl J Med 2012;366:225–33.
Antihypertensive drugs and gout
Calcium channel blockers and losartan are associated with a lower risk of gout in patients with hypertension, whereas diuretics, β blockers, angiotensin-converting enzyme inhibitors and other angiotensin II receptor blockers are associated with increased risk. In a population-based case–control study using a general practice database in the United Kingdom, 24 768 people who had a first diagnosis of gout (or were first started on an anti-gout treatment) were matched with 50 000 controls. After adjustment for risk factors, including alcohol intake and comorbidities, the relative risk of gout among those with hypertension was 0.87 (95% confidence interval [CI] 0.82–0.93) for calcium channel blockers and 0.81 (95% CI 0.70–0.94) for losartan. This is consistent with the agents’ uric–acid-lowering properties. In contrast, the relative risks for other agents ranged as high as 2.36 (95% CI 2.21–2.52) for diuretic use, which suggests that calcium channel blockers or losartan might be preferred for treating those who are at particular risk of gout. See BMJ 2012;344:d8190 doi: 10.1136.bmj.d8190.
Number of embryos transferred in assisted conception
Transfer of three or more embryos should be avoided at any age, but the decision about transferring one or two embryos should take the age of the mother into account. Using a database that collects data on all licensed fertility treatment cycles in the United Kingdom, researchers looked at whether perinatal live birth outcomes varied by the number of embryos transferred in relation to maternal age. Almost 125 000 cycles were assessed; these resulted in 33 514 live births. The overall live birth rate was 27.0 per 100 cycles, with older women less likely to have live births than younger women. All women studied were more likely to have a live birth if two embryos were transferred rather than one embryo (odds ratio in women aged 40 years or older 3.12, 95% confidence interval [CI] 2.56–3.77 v. 2.33 95% CI 2.20–2.46 in those aged less than 40 years). However, older women had a lower risk of adverse events, such as preterm birth, multiple birth and low birth weight, with transfer of two embryos than did younger women. The rates of live birth did not increase with the transfer of three embryos, but the risk of adverse perinatal outcomes did increase. See Lancet 2012; DOI:10.1016/S0140-6736 (11)61267-1.
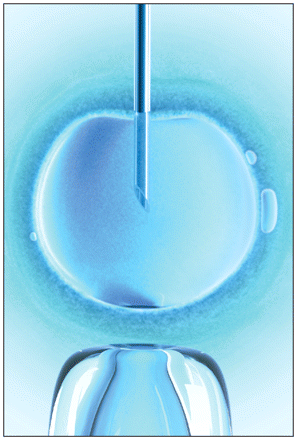
Image courtesy of © 2012 Thinkstock
Treating dementia in Down syndrome
Memantine is not an effective treatment for cognitive impairment and dementia in people older than 40 years with Down syndrome. Although dementia is common in those with Down syndrome, particularly in those over 40 years of age, there is little information on pharmacologic therapy in this group. A controlled randomized trial enrolled 88 adults with Down syndrome who had either dementia at any age or were over the age of 40 years. They were randomly assigned to receive either placebo or memantine for one year; groups were balanced for prognostic factors. At the end of the study, both groups had declined similarly in cognition and function. The authors caution that therapies that may be beneficial in people with Alzheimer disease are not necessarily effective for treating dementia or cognitive impairment in those with Down syndrome. See Lancet 2012; DOI:10.1016/S0140-6736(11)61676-0.








