- © 2007 Canadian Medical Association or its licensors
Suicide has often been called the North's quiet epidemic. It's become a leading cause of death, particularly among Aboriginal youths, in the Northwest Territories as rates skyrocketed over the past decade to the point where they're now twice the national average.
Reversing that disturbing trend is only possible through increased support for community-driven prevention strategies, according to a gathering of experts who convened for the 2007 Canadian Association of Suicide Prevention Conference in Yellowknife, Northwest Territories from Oct. 5 to 8.
Although the staggering rate of growth in the suicide rate appears to have levelled off or even decreased in recent years, it remains a major problem in the North, said Sandy Little, former mental health consultant with the Department of Health and Social Services for the Northwest Territories government.
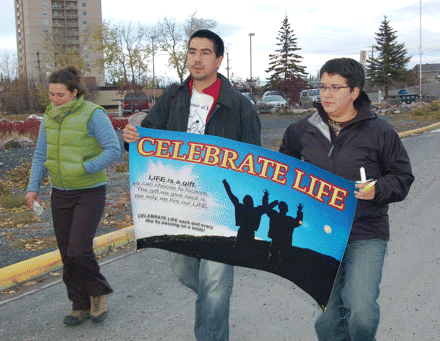
Qajaaq Ellsworth, centre, of the National Inuit Youth Council, took part in a memorial march during the Canadian Association of Suicide Prevention Conference in Yellowknife, Northwest Territories, Oct. 5–8. Ellsworth is part of the Embrace Life Committee, a suicide prevention group that promotes its message to youth in communities throughout Nunavut. Image by: Natalie Dunleavy
A 2003 study conducted by Little indicated that from 1998 to 2002, the rate of suicide in the Territories was 4 times the national average among youth ages 12–19, sitting at 28.8 per 100 000, compared with a national rate of 6.96. There was an even greater disparity in the comparative rates of young adults aged 20–29. In the Northwest Territories, with a population number just over 40 000, that rate was 40 per 100 000, compared with a national rate of 14.78.
Delegates were told a multitude of factors contribute to the higher likelihood of self-harm, particularly within the Aboriginal population, including colonization, residential schools and cultural disruption.
“Suicide is not simply a biological and/or psychological event,” Antoon Leenaars, who has conducted research for the World Health Organization, told the conference. “Suicide is equally an event with socio-cultural factors.”
Delegates also appeared divided on the efficacy of initiatives that have been put in place by various levels of government to reduce suicide rates.
A survey by Ekos Research Associates, in which one-on-one interviews were conducted with aboriginal suicide prevention workers, indicated that Health Canada's efforts to curb the high suicide rate in Canada's Aboriginal youth are not working. In the Ekos report, interviewees “generally dismissed the resources because they were thought to be culturally irrelevant, inappropriately worded, and lacking in actionable solutions.”
But Little took issue with those findings and argued that the most effective suicide prevention strategies are community-oriented. “The money that came from the feds went directly to community based programs,” she said.
Such community-based programs, like one funded by the Northwest Territories government, focus on community counselling, training community wellness workers, and hiring mental health/addictions counsellors and clinical supervisors. To help transcend cultural barriers, community wellness workers underwent government training to adapt material to community norms.
A similar approach was adopted in a recently-established Health Canada program called the National Aboriginal Youth Suicide Prevention Strategy, funded by the First Nations and Inuit Health branch and introduced in 2005–2006.
“It's meant to give communities an opportunity to create a (prevention) strategy of their own,” said Sara Riddell, prevention services wellness planner for the Territories' Department of Social Services.
Some 9 such programs are now running within the 6 regions of the Territories. Under the national strategy, roughly $400 000 will be divided among those communities in 2007–2008. “It gives [communities] the opportunity to put into place things that don't already exist,” said Riddell.
Hiring and training local workers rather than bringing in someone new can help solve the retention problem most isolated communities face, Riddell added. “This is a way they can build the capacity in their own community.”











