- © 2005 CMA Media Inc. or its licensors
New research is advancing our understanding of the genetic factors involved in the development of Crohn's disease. The disease strikes about 6 out of every 100 000 people in Western countries,1 and although a genetic component has long been appreciated the precise pathogenesis remains a mystery. Recent findings from 2 research groups have helped to uncover the pathways that lead to disease.
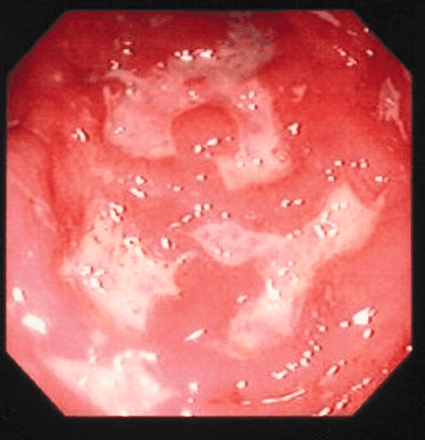
Figure. Photo by: Wolfson Endoscopy Unit, St. Mark's Hospital, London, UK
Genetics of Crohn's disease
Crohn's disease causes chronic inflammation of focused areas of the gastrointestinal tract, resulting in pain and diarrhea. Current research suggests that bacterial infection, or perhaps the entire gut flora, combine with defects in the intestinal immune response to play a causative role.1 How this occurs at the molecular level is not understood, although both environmental and genetic factors are thought to have an influence. Indeed, data on the clustering of Crohn's disease within families and ethnic groups as well as findings from studies involving twins provide strong and enticing evidence that the genetics behind this disease needs to be uncovered.
In 2001, 2 independent research groups did just that, zeroing in on the gene Nod2 (also called CARD15).2,3 Mutations in this gene were found to increase susceptibility to Crohn's disease 40-fold, and 3 common Nod2 were found in patients with Crohn's disease. These findings sparked an exciting drive to understand how Nod2 contributes to the pathology of this disease.
Today, it is known that Nod2 expresses a protein that recognizes a building block of bacterial cell walls, called muramyl dipeptide (MDP), effectively making it a bacterial sensor. Nod2 is expressed primarily by bone-marrow-derived macrophages. In addition, the protein NOD2 appears to play a role in the activation of NF-κB, a major regulator of the production of pro-inflammatory cytoκines such as tumour necrosis factor-α (TNFα) and interleukin IL-1β. The relation is relevant because patients with Crohn's disease overproduce NF-κB and cytokines, and anti-inflammatory drugs represent the mainstays of treatment. Nevertheless, how Nod2 contributes to the pathology of Crohn's disease has been an open question — one that the modelling of the disease in mice is beginning to answer.
Mutating Nod2
Two recent and complementary studies now point directly at a link between Nod2 mutations and increased susceptibility to intestinal bacterial infection. This research provides strong evidence that a primary role of NOD2 is to mediate the immune responses to intestinal bacterial infection.
To examine the effect of NOD2, Maeda and colleagues created a line of mice possessing the most common Nod2 mutation associated with Crohn's disease.4 Although normal in all other respects, these mice produced higher levels of NF-κB and IL-1β when exposed to bacterial MDP, which suggests that the mutation resulted in a heightened response of the Nod2 gene.
To understand the interplay between the Nod2 mutation and bacteria in the gut, Maeda and colleagues provoked bacterial infection in the mutant mice by exposing them to a chemical in their drinking water that destroyed their intestinal mucosal epithelial cells. After 6 days, 37.5% of mutant mice died, compared with none of the normal mice. Nod2 mutant mice also had more inflammatory lesions and produced more cytokines, particularly IL-1β. Interestingly, both oral antibiotics and injection of an antagonist of the IL-1 receptor protected Nod2 mutant mice.
In contrast, Kobayashi and colleagues generated mice lacking Nod2.5 These knockout mice had no obvious intestinal inflammation after 6 months of observation. However, these investigators found that bone-marrow-derived macrophages produced in the Nod2 knockout mice could not detect bacterial MDP. Furthermore, when immunized with MDP, the mice were found to be defective in antibody production. Both findings suggest that NOD2 plays an important role in recognizing the presence of bacteria and inciting an immune response.
To better understand this immune response, Kobayashi and colleagues challenged wild-type and Nod2 knockout mice with the intracellular bacterium Listeria monocytogenes by intravenous, intraperitoneal and intragastric injection. Only via the intragastric route did the knockout mice show increased susceptibility to infection as compared with wild-type mice. This finding implies that there is a specific role for NOD2 in protecting against intestinal infection. The researchers also discovered that antimicrobial peptides called cryptdins (α-defensins in humans) were reduced in Nod2 knockout mice.
The results of these studies help to explain the association between Nod2 mutations and Crohn's disease. In finding Nod2 to be an important immune mediator in the intestine, the studies also fuel the notion that bacterial infection is an important pathogenetic factor. Indeed, as Kobayashi and colleagues suggest, Nod2 mutations may not play a directly causative role but, rather, may create an environment in the gut that renders it susceptible to Crohn's disease. Further research is required to confirm this and to elucidate the link between Nod2 mutations and α-defensin, one that has already been established in humans.6 It is hoped that the results of this research will open future therapeutic avenues.











