- © 2007 Canadian Medical Association
Consider this: in the 20th century, there were more maternal mortalities than deaths from tuberculosis, suicide, traffic accidents and AIDS combined.
Even today, 2 decades after the global health community signed on to the Safe Motherhood Initiative and vowed to halve the number of women who die in childbirth by the year 2000, almost as many women still die from maternal causes as did in 1987.
During that interval, 10.5 million women have died in pregnancy and 160 million babies were stillborn or died in their first 4 weeks. Another 420 million women had unsafe abortions and 315 million have lived with complications such as fistula. Every day 1600 women die during pregnancy, 90% of whom live in developing countries (Table 1). Over her lifetime, an African woman has a 1 in 16 chance of dying from pregnancy-related complications. In the industrialized world, the risk is 1 in 4000.
Table 1.
“It is a humbling experience that on the 20th anniversary of these goals, we still have a half-million women dying every year,” said Dr. Dorothy Shaw, the first woman to be president of the Fédération internationale de gynécologie et d'obstétrique. “We haven't accomplished enough, if anything,” she told attendees at the Society of Obstetricians and Gynaecologists of Canada, International Women's Health Symposium, Safe motherhood and newborn health: looking back, looking forward, which was held June 21 in Ottawa.
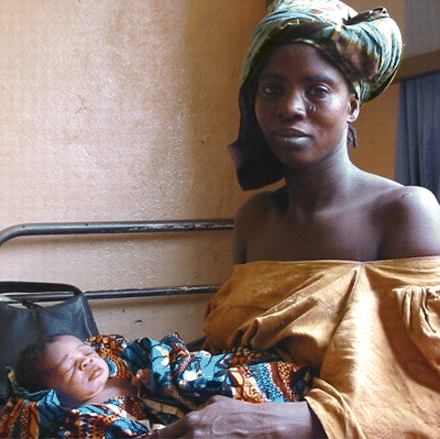
After labouring all night, this Mali mother is tired but proud to present her newborn child. This photo by Dr. Françoise Couturier, entitled “Matin Calme,” placed first in a contest run by the Society of Obstetricians and Gynaecologists of Canada's International Women's Health Program. Photo by: Françoise Couturier
There have been notable steps forward in Uganda (see page 244) and 34 other African countries that have drawn up national plans to reduce maternal and newborn deaths. And there are scattered successes worldwide. A pilot project in India, for example, trained 100 physicians at 3 centres to perform cesarean sections and administer anesthesia; that program is now expanding to 20 centres. The Canadian International Development Agency has spent $45 million on myriad programs, including $350 000 toward creating an obstetrical centre at Mirwais Hospital in Khandahar.
The recent progress may be partially due to revitalization of political will, with the world having committed in the year 2000 to 8 Millennium Development Goals, including 1 to “reduce by three-quarters, between 1990 and 2015, the maternal mortality ratio.”
Prime Minister of Norway Jens Stoltenberg has vowed to accelerate progress towards that goal by launching a Global Business Plan at the United Nations General Assembly in New York City this September. It aims to reduce duplication of efforts by allowing low-resource countries to present 1 plan to a consolidated group of funders.
“It will make better use of resources and increase funding for national health systems,” said Shaw, senior associate dean, faculty affairs at the University of British Columbia.
Further progress is also expected at the Women Deliver conference in London, UK, Oct. 18–20 (http://womendeliver.org), where more than 2000 major political and public figures, health professionals, social scientists and women's advocates will convene.
But while people meet and talk, women continue to die. Many of the 529 000 annual deaths are preventable, since up to 80% of them result from 1 of 5 well-understood and relatively common obstetric complications (see Box 1) that can be readily treated with existing, inexpensive medical or surgical interventions.
The principle underlying medical cause of high maternal mortality is that about one-half of all women in developing countries don't have a skilled birth attendant at delivery; in fact, many women deliver alone. In addition, 201 million women who would like to use contraceptives, can't access them. Not surprisingly, many women die from complications after undergoing unsafe abortions.

Mali nurse, Djeneba, poses with one of her 4 children, for photographer and long-time colleague, Dr. Françoise Couturier, a physician in St. Lambert, Que. The photo was first runner-up in a contest run by the Society of Obstetricians and Gynaecologists of Canada's International Women's Health Program. Photo by: Françoise Couturier
Insufficient numbers of trained health professionals is a widespread problem. The Lancet's frequently cited series on maternal survival (September 2006) concluded that the health centre model could achieve 73% coverage by 2015 for 75 priority countries if 334 000 more health care professionals could be recruited and 24 000 birthing units plus 11 000 maternity units established.
The Lancet estimated that achieving Millennium Goal 5 would cost between US$5.5 billion and US$6.1 billion in additional funds. Yet, in 2004, donors invested just US$530 million in newborn and maternal health.
“Yes, we need a lot. But does that mean we can't do it? I don't think so,” said Shaw, adding that “decreasing maternal mortality is the key to improving the health of the population.”
Depending upon the country, the Fédération identifies as priority activities the need to track maternal mortality; establish partnerships with ministries of health, midwives and others; establish effective family planning; avoid unsafe abortions; institute competency-based training for emergency obstetrical services; and effectively share more information.
“We know what to do,” said Shaw. “We know how to do it. We can't do it alone. We can't do it all at once.” The first goal, though, is access to emergency obstetric care.












