An 80-year-old man presented with a one-week history of constant epigastric pain and left-sided exertional chest pain. On the day of presentation, he had experienced four episodes of nonbilious vomiting, but had no other gastrointestinal symptoms. He did not report fever, chills or sweats. There was no history of recent travel or contact with an ill person. His medical history included hypertension, type 2 diabetes mellitus, dyslipidemia, prior myocardial infarction with left ventricular dysfunction, and a left hemicolectomy for adenocarcinoma of the colon, which was in remission.
He was afebrile, his heart rate was 112 beats/min and his blood pressure was 123/71 mm Hg. Except for mild tenderness in the upper abdominal quadrants, his physical examination was normal. The results of laboratory investigations are summarized in Table 1. Electrocardiography showed a first-degree atrioventricular block with sinus bradycardia.
Results of laboratory investigations in an 80-year-old man with epigastric pain
The patient was admitted with a diagnosis of non–ST-segment elevation myocardial infarction and received evidence-based therapies. His chest pain resolved; however, his epigastric pain persisted.
What is the next step in investigating his persistent epigastric pain?
-
Abdominal ultrasonography
-
Contrast-enhanced computed tomography (CT) of the abdomen
-
Plain radiography of the abdomen
-
Exploratory laparotomy or laparoscopy
-
Esophagogastroduodenoscopy
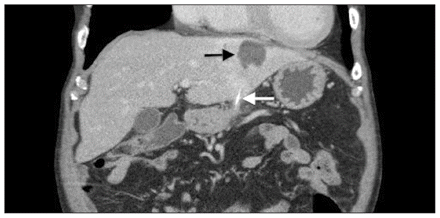
To further investigate his epigastric pain, in association with newly elevated liver enzymes, (a) abdominal ultrasonography was first performed followed by (b) contrast-enhanced CT of the abdomen. Ultrasonography showed two hypoechoic lesions in the liver, the largest measuring 3.0 × 3.1 × 3.3 cm; one of the lesions had a cystic component. The biliary tract was normal. The contrast-enhanced CT scan of the abdomen showed two rim-enhancing lesions, the largest measuring 5.9 × 3.7 cm. A curved, calcified foreign body was identified, spanning between the gastric antrum and one of the liver lesions (Figure 1). No other abnormalities were noted.
Coronal contrast-enhanced computed tomographic scan of the abdomen in an 80-year-old man with persistent abdominal pain, showing a curved, calcified object (white arrow) communicating between the gastric antrum and the left lobe of the liver. A hypodense lesion is seen in the left lobe of the liver (black arrow).
What is your diagnosis?
-
Liver metastases
-
Hemangiomas of the liver
-
Multifocal hepatocellular carcinoma
-
Liver abscesses secondary to foreign-body migration
The diagnosis is (d) liver abscesses secondary to migration of a foreign body. Based on the CT findings, the foreign body appeared to originate from the gastric antrum, penetrating through the wall of the stomach into the left lobe of the liver. The patient was started on intravenous piperacillin–tazobactam, empirically.
What is your next step in management?
-
Esophagogastroduodenoscopy for retrieval of the foreign body
-
Laparotomy or laparoscopy for retrieval of the foreign body and drainage of the abscesses
-
Continuation of antimicrobial therapy alone
-
Catheter drainage of the liver abscesses by an interventional radiologist
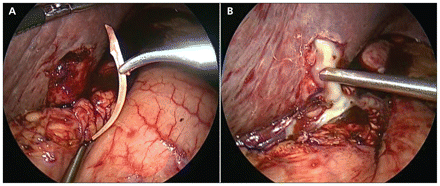
Laparoscopy (b) was performed to retrieve the foreign body. A 6-cm fishbone was removed (Figure 2A). A fistulous tract extending between the gastric antrum and the left lobe of the liver was identified. The liver abscesses were explored and drained (Figure 2B), and a specimen was sent for microbiologic analysis. The abscess culture grew an organism of the Streptococcus anginosus group. Blood cultures were negative. The antimicrobial therapy was subsequently changed to intravenous penicillin and metronidazole. When the patient was able to tolerate oral medications, he was prescribed oral amoxicillin–clavulanate. Following a four-week course of antibiotics, his epigastric pain had completely resolved, and follow-up CT of the abdomen showed complete resolution of the pyogenic liver abscesses.
(A) Laparoscopic image of a fishbone that was removed from the left lobe of the liver. (B) Laparoscopic drainage of a pyogenic liver abscess.
Discussion
The annual incidence of pyogenic liver abscess has been estimated at 1.1–2.3 cases per 100 000 population.1,2 Incidence increases with age: people aged 65 years or older are 10 times more likely than younger people to develop pyogenic liver abscesses.1 This parallels the increased incidence of biliary tract disease in older populations.3,4 Risk factors for pyogenic liver abscess include male sex, advanced age, biliary tract disease, diabetes mellitus, liver transplantation, malignancy and percutaneous treatments for hepatocellular carcinoma, including radiofrequency ablation.1,5 The most common clinical features include fever (73%), chills (45%) and right upper quadrant pain (38%). The most frequent laboratory abnormalities include hypoalbuminemia (96%), elevated γ-glutamyl transferase (81%), elevated alkaline phosphatase (71%) and leukocytosis (69%).1
Microbial causes include Escherichia coli, Klebsiella pneumoniae, streptococci (including organisms of the S. anginosus group) and anaerobes (including Bacteroides fragilis).1 Many liver abscesses are polymicrobial. Abscesses secondary to biliary tract disease and other intra-abdominal infections are more likely to be polymicrobial in etiology, whereas primary or cryptogenic liver abscesses are more likely to be monomicrobial in etiology.6 In our patient, an organism of the S. anginosus group was isolated. This organism is commensal to the oral cavity and would be compatible with a swallowed foreign body with gastric penetration as the mechanism of infection. Blood cultures should be obtained in all instances of suspected pyogenic liver abscess; blood cultures are positive in about 50% of cases.1
Routes of infection
Pyogenic liver abscesses may be classified according to the presumed route of infection. As summarized in Box 1, infectious pathways include the biliary tract, portal vein, hepatic artery, contiguous spread from an adjacent intra-abdominal focus of infection and trauma, including foreign-body migration.1 Still, a likely route of infection often cannot be found, and as many as 50% of instances are therefore labelled “primary” or “cryptogenic.”1
Routes of infection in pyogenic liver abscess and predisposing conditions1,2,5,7
-
Biliary tract
-
- Ascending cholangitis
-
-
Portal vein
-
- Diverticulitis, ischemic colitis, appendicitis and inflammatory bowel diseases
-
- May be associated with suppurative thrombophlebitis of the portal vein
-
-
Hepatic artery
-
- Systemic bacteremia
-
-
Contiguous focus of infection
-
- Gallbladder diseases, including cholecystitis, gallbladder empyema and gallbladder perforation
-
- Subphrenic abscess
-
- Perinephric abscess
-
-
Trauma
-
- Liver lacerations secondary to penetrating trauma
-
- Posthepatic resection
-
- Radiofrequency ablation procedures for malignancy
-
-
Primary or cryptogenic
-
- Occur in the absence of the above conditions
-
- Hypermucoviscous variants of Klebsiella pneumoniae are increasingly being recognized as a cause
-
- Chronic granulomatous disease
-
One emerging cause of primary liver abscess is K. pneumoniae caused by a hypermucoviscous phenotype. Primary liver abscesses due to this organism occur in the absence of the traditional routes of infection listed in Box 1. Abscesses related to K. pneumoniae have been associated with diabetes mellitus and impaired glucose tolerance, and have had their greatest incidence in people of Southeast Asian origin. This bacterium has the propensity for metastatic spread beyond the liver, resulting in endophthalmitis and meningitis.7,8
Diagnostic imaging
Recommended imaging for suspected pyogenic liver abscess includes abdominal ultrasonography and contrast-enhanced CT of the abdomen.9 Abdominal ultrasonography allows for the best evaluation of the biliary tract.9 On the other hand, contrast-enhanced CT of the abdomen provides increased sensitivity compared with ultrasonography (95% v. 90%); better visualization of predisposing conditions including appendicitis, diverticulitis and inflammatory bowel disease; and contrast visualization of the portal vein to assess for the presence of suppurative thrombophlebitis.9,10
Liver abscess and foreign-body ingestion
There are little data outlining the incidence of foreign-body ingestion in the adult population. Risk factors for intentional foreign-body ingestion include psychiatric illness and incarceration.11 Liver abscesses secondary to foreign-body migration are rare but should be considered when there is a history of foreign-body ingestion, when imaging is suggestive and when treatment fails despite appropriate antimicrobial therapy and drainage. Only 5% of patients with foreign-body abscesses recall the ingestion.11 In our patient, abdominal CT showed the foreign body. Only in retrospect did he mention routinely consuming fish three times per week. He did not recall swallowing a fishbone.
Liver abscesses resulting from foreign-body migration most commonly occur in the left lobe of the liver, often as a result of perforation through the gastric antrum or proximal small bowel. Common foreign bodies include fishbones (44%), toothpicks (29%), chicken bones (8%), metallic objects (14%) and unidentified bones (5%).11 Clinical and laboratory features of liver abscess secondary to foreign-body migration are similar to those related to other mechanisms of infection.11 A systematic review of the literature that identified 60 instances of pyogenic liver abscess related to foreign-body migration suggested improved sensitivity of CT over ultrasonography for visualization of foreign bodies; however, imaging may be nondiagnostic in more than 50% of instances.11 A thickened gastrointestinal wall in contact with a liver abscess may suggest a migrated foreign body as the mechanism of infection. For instances in which a foreign-body mechanism is suspected and the foreign body is not seen on imaging, esophagogastroduodenoscopy is recommended.11 Findings at endoscopy may include direct visualization of the foreign body, mucosal inflammation and the presence of a fistulous tract. Endoscopy may assist with foreign-body removal. In some instances, exploratory laparotomy or laparoscopy may be needed to arrive at the diagnosis.11
Management
The management of a visceral abscess, including a pyogenic liver abscess, should include a combination of drainage of the abscess and antimicrobial therapy.5 A typical empiric antimicrobial regimen may include ceftriaxone intravenously in combination with metronidazole for the coverage of intestinal gram-negative bacilli, S. anginosus group organisms and intestinal anaerobes. Definitive antimicrobial therapy should be based on the results of cultures. In most instances, a short course of intravenous antibiotics is followed by oral antibiotics, with common durations ranging from four to six weeks.12
Percutaneous drainage of liver abscesses should be performed for both therapeutic and diagnostic purposes, with a specimen sent for Gram stain and both aerobic and anaerobic culture.5 Indwelling catheter drainage of the abscess has become the standard of care, but recent studies have suggested needle drainage may offer comparable outcomes with greater ease.13
In instances of liver abscess related to foreign-body migration, rates of cure without foreign-body removal are low (9.5%).11 Removal of the foreign body is critical to permitting resolution of the abscess and closure of fistulous tracts. Surgical drainage of the abscess at the time of removal of the foreign body appears to be an adequate means of source control (i.e., eradicating the focus of infection).11 There are limited data addressing the need for ongoing catheter drainage following surgical drainage in this situation. Surgical drainage is in principle similar to needle drainage, which has shown comparable efficacy to catheter drainage in instances of pyogenic liver abscess due to all causes.13
Methods of foreign-body removal include laparotomy, laparoscopy, and endoscopy of the upper or lower gastrointestinal tract.11 Natural orifice transluminal endoscopic surgery may offer an additional method of minimally invasive foreign-body removal.14 In this patient, a laparoscopic approach was used for removal of the fishbone.
CMAJ invites submissions to “What is your call?” Clinical details (including images) are presented on the first page along with a multiple-choice question about the diagnosis. The answer and a brief discussion of the condition follow on the second page. We specifically invite submissions illustrating common or important radiographic and electrocardiographic diagnoses of appeal to a general audience. We require authors to obtain consent from the patient for publication of his or her story (form available at www.cmaj.ca/authors/checklist.shtml). Submit manuscripts online at http://mc.manuscriptcentral.com/cmaj.
Footnotes
-
Competing interests: None declared.
-
This article has been peer reviewed.