- © 2008 Canadian Medical Association
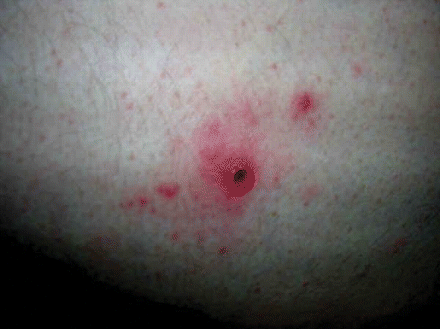
A 47-year-old man presented to the emergency department with fever, chills, drenching sweats and erythema over his left buttock and groin. He was taking cephalexin, which had been prescribed 3 days earlier for presumed cellulitis, with no clinical response. The patient informed us that he had been on a bush safari in South Africa 10 days earlier. Careful physical examination revealed a black crusted lesion 10 mm in diameter with a surrounding red halo on his left buttock (Figure 1). Initial bloodwork indicated mild leukopenia (leukocyte count 1.7 × 109/L) and transaminitis (aspartate aminotransferase level 67 U/L, alanine aminotransferase level 97 U/L). Malaria films were negative. We made a clinical diagnosis of African tick-bite fever and prescribed a 1-week course of doxycycline. The patient's symptoms resolved within 48 hours. Serologic testing of samples taken in the acute phase were negative for rickettsial antibodies, but we detected Rocky Mountain spotted fever antibody titres (IgM ≥ 1/64, IgG ≥ 1/256) in convalescent serum samples.
Figure 1: Black crusted lesion, or tache noire, 10 mm in diameter, on the left buttock of a 47-year-old man.
African tick-bite fever is caused by Rickettsia africae, one of the spotted fever group of the Rickettsia species, and is transmitted in sub-Saharan Africa by Amblyomma ticks.1 About 1 week after a tick bite, an influenza-like syndrome with fever, fatigue, headache and myalgia develops. A black eschar, or tache noire, occurs at the site of the tick bite. Multiple bites may result in several eschars. Lymphadenitis in the nodes draining the eschar site can occur, and rashes, both adjacent to the eschar and generalized, are relatively common.
Diagnosis of African tick-bite fever is usually established on clinical grounds. Nonspecific laboratory abnormalities include lymphopenia and, less commonly, transaminitis (40% of cases) and thrombocytopenia (20% of cases). Serologic tests for R. africae are not commercially available; however, since there is cross-reactivity between R. africae and Rocky Mountain spotted fever antibodies, positive results for those antibodies can support the clinical diagnosis. The clinical presentation of African tick-bite fever may be distinguished from Rocky Mountain spotted fever (caused by Rickettsia rickettsii) by the presence of an eschar, and from Mediterranean spotted fever (caused by Rickettsia conorrii) if multiple eschars are present. Although performing a biopsy of the eschar is not common, biopsy results can also distinguish African tick-bite fever from Mediterranean spotted fever.2 In addition, thick and thin films and blood cultures are required to rule out competing diagnoses, including malaria and typhoid fever.
Tourism in South Africa, the most common source of African tick-bite fever cases, has increased dramatically since the end of apartheid; in 2005, 67 400 Canadians travelled to that country.3 The only prospective study to date found that African tick-bite fever occurred in 4% of travellers to sub-Saharan Africa. Of note, the classic eschar seen in the case of our patient was found in the cases of only half of those infected.4 Risk factors for infection include game hunting and travel to southern Africa from November to April.
Travellers can protect themselves from African tick-bite fever by wearing long-sleeved clothing; however, in hot climates adherence may be difficult. The role of topical insect repellents in preventing tick bites is unclear. A recent study found that products containing more than 20% diethyltoluamide (DEET) provided substantial but short-term protection.5
This case emphasizes the need to obtain a travel history for all febrile patients, including a detailed timeline and exposure profile. African tick-bite fever should be considered in patients with fever, headache and myalgia who have travelled to disease-endemic countries. When present, an eschar is a helpful clue and so should be sought carefully. Therapy with doxycycline (100 mg twice a day for 7 days) typically leads to rapid improvement; however, a subset of patients may experience a prolonged convalescence characterized by arthralgia and malaise.
Footnotes
-
This article has been peer reviewed.
Acknowledgements: We thank Jennifer Morson for the photograph of the tache noire.
Competing interests: None declared.