A healthy 68-year-old woman presented to the emergency department with a 6-month history of neck pain, weakness of the arms, hand incoordination, difficulty walking and tingling sensations in the arms and legs. She had been in a motor vehicle collision 25 years earlier in which the base of the odontoid process had been fractured.
Examination showed increased muscle tone, diffuse hyperreflexia, unsteady broad-based and hesitant gait, and Hoffman and Babinski signs. Computed tomography (CT) (Figure 1A) imaging showed a chronic odontoid pseudoarthrosis complicated by anterior subluxation, a substantial posterior osteophyte narrowing the spinal canal and striking segmental kyphosis. Magnetic resonance imaging (MRI) (Figure 1B) showed that the spinal cord was compressed ventrally and under tension because of the osteophyte and the remainder of the axial body. Axial CT imaging of the most compressed site (Figure 1C) showed severe narrowing of the spinal canal; at this level, MRI also showed focal segmental T2-weighted signal abnormality.
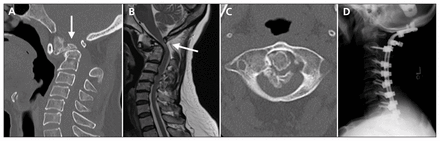
A 68-year-old woman presented with acutely progressive myelopathy 25 years after a motor vehicle collision. Computed tomography (A, C) showed a chronic odontoid pseudoarthrosis, anterior subluxation, a substantial posterior osteophyte (A, arrow) and segmental kyphosis. Magnetic resonance imaging showed ventral compression of the spinal cord (B, arrow) by the posterior osteophyte and the remainder of the axial body, in addition to subaxial spinal spondylotic disease. Transoral decompression of the odontoid fragment, posterior osteophyte and body was followed by posterior occipitothoracic decompression and fusion (D).
We used preoperative halo traction to reduce kyphosis, after which we performed transoral decompression of the odontoid fragment, posterior osteophyte and vertebral body, followed by posterior laminectomy of the first cervical vertebra and subaxial decompression (Figure 1D). Our patient has now improved to functional independence, with no evidence of pseudoarthrosis or implant failure.
This patient’s case highlights the hazards of nonunited odontoid fractures in adults. Rarely, such pseudoarthrosis may predispose the patient to mechanical neck pain1 and progressive craniocervical deformity.2 The association with progressive cervical myelopathy and the appropriate surgical remedy for when it occurs remains undefined. Close follow-up after either conservative or surgical management remains important to protect these patients from delayed complications.
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
The authors have obtained patient consent.