Critical care bypass
In January 2000, 18-year-old Joshua Fleuelling suffered an asthma attack and was transported by ambulance to hospital, but not the one nearest his home because it was on “critical care bypass.” Anne Walker examines policies of critical care bypass in a legal framework, reviewing the concept of duty to care as it relates to emergency physicians, who do not necessarily have a pre-existing relationship with their patients. She discusses the legal dilemmas that arise when the physician's duty to care confronts real-world problems of staff and equipment shortages and emergency department overcrowding. In a related commentary, Jane Upfold provides an emergency physician's perspective on the challenges of weighing the potential harms of having patients diverted to another hospital against those of accepting critically ill patients and possibly jeopardizing the care of patients already in the overcrowded emergency department.

Figure.
Fewer “general” practitioners
Comprehensiveness and continuity of care are key principles of family medicine. Benjamin Chan studied Ontario physician billing data for 1989/90 to 1999/2000 and extracted demographic variables as well as the numbers of physicians doing inpatient hospital visits, house calls, emergency work, nursing-home visits, obstetric deliveries, anesthesia or exclusively office work. Over the years studied, the proportion of physicians practising exclusively in their offices increased from 14% in 1989/90 to 24% in 1999/2000 (p < 0.001). In 1999/2000, recent graduates were more likely than older physicians to be involved in emergency medicine work (40% v. 5%), whereas older physicians were more likely than recent graduates to do house calls and nursing-home visits (57% and 20% v. 37% and 11%). Physicians with only an office practice were more likely to be female (odds ratio [OR] 2.65, 95% confidence interval [CI] 2.37–2.96), recent graduates (OR 1.35, 95% CI 1.15–1.60), aged 65 years and older (OR 1.45, 95% CI 1.20–1.75) or practising in a city with a medical school (OR 2.30, 95% CI 2.06–2.56) and less likely to be rural physicians (OR 0.31, 95% CI 0.24–0.41) or certified in family medicine (OR 0.58, 95% CI 0.52–0.66).
Figure.
See page 429
Ultrasound therapy for fractures
Animal models have shown that the use of low-intensity pulsed ultrasound may promote fracture healing, although the mechanism is unknown. Jason Busse and colleagues conducted a systematic review and meta-analysis to summarize the data from randomized controlled trials involving humans that studied the effect of ultrasound therapy on fracture healing. Of 138 potentially eligible studies, 3 were judged to be of good quality and sufficiently heterogenous that the data could be pooled. These trials involved 158 fractures at 3 different sites: the tibial shaft, the distal radius and the scaphoid. In all 3 studies, the mean time to healing was shorter in the treatment groups than in the control groups (weighted average effect size 6.41; 95% confidence interval [CI] 1.01–11.81). The authors acknowledge that, although more and better trials are needed, self-applied ultrasound treatment holds promise for shortening the healing time of nonoperative fractures.
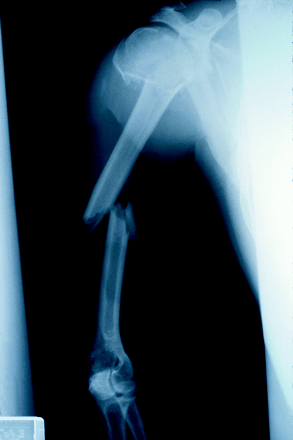
Figure.
See page 437
Drugs in renal failure
The kidneys are the route of elimination for many drugs and their metabolites. Some medications can easily reach toxic levels in patients with renal disease, and these people can be especially sensitive to the nephrotoxic effects of other drugs. Joanne Kappel and Piera Calissi review the relevant principles of pharmacology and discuss simple strategies for safe drug prescribing in renal failure. Commonly prescribed medications and herbal remedies that are affected by states of renal insufficiency are also discussed.
See page 473










