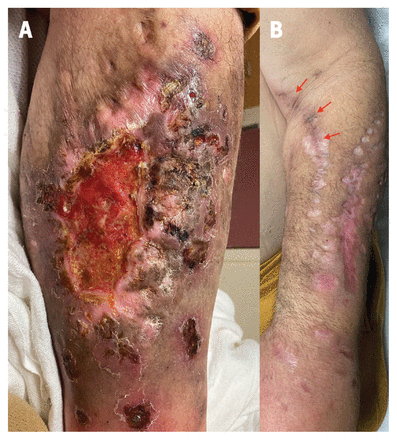
A 55-year-old man with a history of intravenous heroin use presented to the emergency department with a 14-month history of a large ulcer on his left lower leg that would not heal. The ulcer was lined with granulation tissue, with many surrounding confluent, nummular, depressed, hyperpigmented and hypopigmented sclerotic patches (Figure 1A). He also had numerous needle tracks, hyperpigmentation over veins and nummular scars consistent with “skin popping” whereby drugs are injected under the skin (Figure 1B). The patient reported previously using the ulcer as an injection site, with last use more than 1 year ago. We diagnosed a chronic skin ulcer associated with and used for injection of drugs, known colloquially as a “shooter’s patch.” Wound cultures grew methicillin-resistant Staphylococcus aureus and Streptococcus pyogenes. During hospital admission, the internal medicine team treated the patient with intravenous vancomycin, and nursing staff dressed the wound with petrolatum gauze and a sterile bandage. When he left the hospital, he transitioned to oral doxycycline and amoxicillin–clavulanic acid, after which he was lost to follow-up.
Photographs of a 55-year-old man with a history of intravenous drug use, showing (A) an ulcer on the left lower leg with granulation tissue, surrounded by depressed, sclerotic nummular patches; and (B) numerous depressed, nummular, sclerotic patches on his left arm, with hyperpigmentation overlying a vein (arrows).
Cutaneous signs of intravenous drug use are more often seen in long-term injectors than in short-term injectors.1 As easily accessible veins become exhausted, drug users may inject into intradermal or subcutaneous spaces, known as “skin popping,” resulting in abscesses or ulcerations, which may resolve with characteristic depressed, nummular scars.2 Subsequently, the rich vascular supply provided by these ulcers may be used for further injection. Such ulcers are often found in accessible sites that may be easily covered by clothing, including the forearm, thigh or anterior lower leg.2,3 We propose that these lesions be referred to as chronic cutaneous ulcers from drug use, which is a less stigmatizing term than “shooter’s patches.”
Vascular damage from the repetitive trauma of injection and secondary infection may contribute to the persistence of ulcers.1,2 Bacterial cultures from the wound should be obtained, using specimens from deep aspirate or biopsies, along with blood cultures if systemic infection is suspected, to guide antibiotic therapy. Imaging may be required to rule out osteomyelitis.1–3 Either secondary healing of the lesion or surgical management may be indicated depending on wound characteristics such as size and presence of infection, patient comorbidities (including diabetes, peripheral vascular disease and smoking) and the patient’s ability to access care and attend follow-up appointments. 2 Given the high rate of precarious housing and homelessness among people who use intravenous drugs, referral to social care and exploration of the patient’s motivation to engage in addiction treatment should be considered.4,5
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
The authors have obtained patient consent.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/