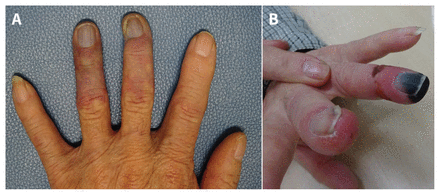
An 80-year-old man presented to our clinic with a 7-month history of purple discoloration, numbness and pain of the left third and fourth digits (Figure 1A). His other hand and his feet were unaffected. The discoloration was exacerbated by cold exposure but did not return to normal colour or show paroxysmal pallor, ruling out Raynaud phenomenon. He had a history of well-controlled diabetes, was not hypertensive and did not smoke. His body mass index was 19.7.
Left hand of an 80-year-old man with cold agglutinin disease. (A) On presentation, showing peripheral acrocyanosis distal to the proximal interphalangeal joints of the third and fourth fingers. (B) One week later, showing necrosis at the tip of the fourth finger.
Laboratory investigations were as follows: hemoglobin 10.6 (normal 13.5–17.6) g/dL, reticulocyte count 6.4% (normal 0.6%–2.0%), indirect bilirubin 1.2 (normal 0.2–0.9) mg/dL, lactate dehydrogenase 514 (normal 106–211) IU/L, reduced haptoglobin, elevated immunoglobulin M (IgM) 526 (normal 33–190) mg/dL, hemagglutination on blood smear (Appendix 1, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.211570/tab-related-content) and normal leukocyte count. A direct Coombs test was anti-C3 positive and cold agglutinin titre was 1:8192 (normal < 64) at 4°C. Screening for infectious mononucleosis, Mycoplasma pneumoniae, syphilis, antinuclear antibodies, autoantibodies and cryoglobulin was negative. Whole-body computed tomography was normal. We diagnosed cold agglutinin disease and referred the patient to hematology. Seven days later, his left fourth fingertip appeared necrotic (Figure 1B). Because neither revascularization nor surgery was indicated, the patient was instructed to avoid exposure to cold and keep warm, and the finger healed. At 12-months’ follow-up, having avoided cold exposures only, he had no new lesions or progression of anemia.
Cold agglutinin disease is an autoimmune hemolytic anemia in which the autoantibody is a cold agglutinin, usually IgM, which reacts with red blood cell antigens at 3–4°C. It affects 1.9/1 000 000 people.1 Primary cold agglutinin disease occurs as a result of cold-reacting autoantibodies, whereas secondary cold agglutinin disease occurs as a result of infection, autoimmunity or malignant disease.1,2
Hemagglutination leads to localized circulatory failure, resulting in acrocyanosis, Raynaud phenomenon, livedo reticularis and, rarely, necrosis. Differential diagnoses include vascular occlusive disease, cryoglobulinemia, frostbite and chilblain lupus erythematosus.2 To diagnose cold agglutinin disease, the cold agglutinin titre is at > 64, but usually higher.1,2 Management is usually conservative, with advice to keep warm and avoid cold exposures, including cold foods and drinks. Management may also include warmed transfusions or fluids, if required. If the patient is severely anemic, rituximab, sutimlimab or plasmapheresis may be used.1,3
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
The authors have obtained patient consent.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/