Abstract
Background: Access to primary care protects the reproductive and non-reproductive health of females. We aimed to quantify health care disparities among “off-reserve” First Nations, Métis and Inuit females, compared with non-Indigenous females of reproductive age.
Methods: We used population-based data from cross-sectional cycles of the Canadian Community Health Survey (2015–2020), including 4 months during the COVID-19 pandemic. We included all females aged 15–55 years. We measured health care access, use and unmet needs, and quantified disparities through weighted and age-standardized absolute prevalence differences compared with non-Indigenous females.
Results: We included 2902 First Nations, 2345 Métis, 742 Inuit and 74 760 non-Indigenous females of reproductive age, weighted to represent 9.7 million people. Compared with non-Indigenous females, Indigenous females reported poorer health and higher morbidity, yet 4.2% (95% confidence interval [CI] 1.8% to 6.6%) fewer First Nations females and 40.7% (95% CI 34.3% to 47.1%) fewer Inuit females had access to a regular health care provider. Indigenous females waited longer for primary care, more used hospital services for nonurgent care, and fewer had consultations with dental professionals. Accordingly, 3.2% (95% CI 0.3% to 6.1%) more First Nations females and 4.0% (95% CI 0.7% to 7.3%) more Métis females reported unmet needs, especially for mental health (data for Inuit females not reported owing to high variability).
Interpretation: During reproductive age, Indigenous females in Canada face many disparities in health care access, use and unmet needs. Solutions aimed at increasing access to primary care are urgently needed to advance health care reconciliation.
Primary care is a fundamental human right.1 For females of reproductive age, primary care protects against prevalent health issues, such as heart disease, depression and cancer, and supports reproductive decision-making.2 As most pregnancies in Canada are unintended,3 primary care during reproductive age also serves as preconception care, helping more females enter pregnancy in good health and improving neonatal outcomes.2,4–6 Equitable health care at this life phase may therefore interrupt intergenerational cycles of disease and narrow gaps in health outcomes.7,8 Yet Indigenous females continue to experience inequitable health care.9,10 This is largely a result of colonial policies,5,11 including targeted violence and racism, residential schools, forced or coerced sterilization, and destruction of traditional lands.12–15 Although Indigenous females are highly resilient,12,14 these health care disparities are exacerbated by unique health needs imposed by social and material deprivation16 and concurrent challenges to access care in a disjointed jurisdictional system,16 resulting in medical relocations for birthing and general health care.17–19 Indigenous females are keenly aware of this reality. Nevertheless, current data among females are lacking and often group Indigenous Peoples together, which overlooks their distinct needs and diverse histories and cultures. Following calls to action by the Truth and Reconciliation Commission of Canada,12 and in partnership with national Indigenous women’s and Two-Spirit groups,20,21 we aimed to quantify current disparities related to general health care needs among “off-reserve” First Nations, Métis and Inuit females of reproductive age.
Methods
Study design
We conducted a repeated cross-sectional study using data from the annual Canadian Community Health Survey (CCHS),22 which covers about 98% of Canada’s population aged 12 years and older, excluding those living in institutions and certain remote regions, among others. The survey notably excludes First Nations Peoples living on “reserve,” defined as government land allocated for community use by ongoing colonial policy.23 Those living on “reserve” have unique challenges to health care access that cannot be examined with the CCHS, including remoteness and limited health care providers, medical facilities and resources. As the term is defined by the survey rather than being culturally safe, we have placed it in quotation marks. To produce reliable and representative estimates, the CCHS employs a complex multistage sampling strategy and releases data in 1-year files for the provinces and 2-year combined files to include the territories.22
As the survey was redesigned in 2015,22 we used cycles spanning 2015 to 2020, including 2-year files in descriptive and 1-year files in trend analyses. In 2020, data collection was halted between April and August by the COVID-19 pandemic, resulting in only 4 months of pandemic-era data collection (September–December). Response rates for 2-year cycles were 59.5%, 60.8% and 41.0%, respectively.
We recruited collaborators for an Indigenous Advisory Committee, which included representatives from Pauktuutit Inuit Women of Canada, 2 Spirits in Motion Society, Les Femmes Michif Otipemisiwak (Women of the Métis Nation) and Native Women’s Association of Canada, as well as 1 of the authors (J.L.). This committee assisted at all stages of the study. We met with these advisors twice, once before study design and once after data analysis, both times incorporating their feedback and lived experiences into the work. In between, we communicated over email to send draft study proposals, results and manuscripts for feedback, and held meetings with individual organizations when requested. We are currently planning another meeting with the committee to disseminate the findings to their communities. Further details are provided in Appendix 1, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.221407/tab-related-content.
We complied with Strengthening the Reporting of Observational Studies in Epidemiology (STROBE)24 and Guidance for Reporting Involvement of Patients and the Public (GRIPP2)25 reporting guidelines (checklists in Appendix 1), as well as Statistics Canada release guidelines.22
Population
We included all people assigned female at birth and of reproductive age, using the CCHS definition (15–55 yr22) for consistency with other studies. The CCHS refers to this group as “females,” given no data were collected on gender identity until 2019. The survey asked only participants born in Canada, the United States, Germany or Greenland (as explained in Appendix 1) to self-identify as Indigenous to Canada. Indigenous participants were further asked if they belonged to 1 or more of 3 Indigenous groups recognized by the Canadian Constitution. These groups include First Nations, a group of more than 630 culturally diverse communities that were the earliest inhabitants of present-day Canada; Métis, a group with mixed Indigenous and European ancestry that developed a distinct identity; and Inuit, a group that primarily lives in the Arctic region of Canada (known as Inuit Nunangat) and whose culture and way of life are adapted to it. The survey subsequently asked non-Indigenous participants to self-identify as belonging to 1 or more of 12 racial or cultural groups (White, South Asian, Chinese, Black, Filipino, Latin American, Arab, Southeast Asian, West Asian, Korean, Japanese or other [unspecified]).
Outcomes
We ascertained all available health care indicators in the CCHS, as well as sociodemographic and health information. Measures of general health care access, collected from participants in all the cycles, included whether participants had a regular health care provider; whether they had a usual place for immediate, nonurgent care of a minor health problem; and how long they usually waited for an appointment with their provider for such a problem. Measures of general health care use, collected from participants in 2015 and 2016, included frequency of consultations with a primary care physician, specialist or other health professional and whether an emergency department visit or overnight hospital admission had occurred in the past 12 months. Measures of unmet health care needs, collected from 8 provinces and 2 territories interested in these data, included whether participants did not receive needed health care in the past 12 months, reasons for unmet needs, and types of care needs that were unmet. Further details are provided in Appendix 1.
Statistical analyses
We focused on “off-reserve” First Nations, Métis and Inuit participants and present results separately. We produced descriptive statistics to characterize the sample and calculated the prevalence of health care access, use and unmet health care needs using an available-case analysis to maximize sample size. All analyses were weighted using bootstrap methods and sampling weights provided by Statistics Canada to account for complex, multistage sampling and to produce estimates representative of the Canadian population, respectively.22,26 We additionally age-standardized these measures to the 2016 Census population using the direct method and 5-year age groups to account for confounding by age.27 To quantify disparities, we computed absolute prevalence differences (in percentage points) and 95% confidence intervals (CIs) compared with non-Indigenous females.
In a post-hoc analysis, we sought to determine the extent to which disparities could be related to sociodemographic differences. To do so, we computed adjusted prevalence ratios and 95% CIs using log-binomial regression, weighted using sampling weights only (owing to software limitations), and controlled for characteristics (age, education, household income, region and region type) that are likely to influence care. As a sensitivity analysis, we calculated prevalence results without standardization. In secondary analyses, we assessed health care disparities among participants with multiple or unspecified Indigenous identities and those recently or currently pregnant, and examined the characteristics of those with missing data.
We conducted all analyses using SAS Enterprise Guide 7.1 (SAS Institute Inc.).
Ethics approval
Statistics Canada obtained informed consent from all study participants. As per Articles 2.2 and 9.21 of the Tri-Council Policy Statement: Ethical Conduct for Research Involving Humans, this research is exempt from research ethics board review as it relies on publicly available data that are legally protected by Statistics Canada.28 With guidance from our Indigenous Advisory Committee, we respected the principles of OCAP (ownership, control, access and possession),29 Inuit Qaujimajatuqangit,30 a guideline from the Canadian Institutes of Health Research,31 and the United Nations Declaration on the Rights of Indigenous Peoples,32 as described in Appendix 1.
Results
Our study population included 2902 First Nations, 2345 Métis, 742 Inuit and 74 760 non-Indigenous females of reproductive age. Among non-Indigenous females, 70.7% self-identified as White (Table 1). Compared with non-Indigenous females, First Nations, Métis and Inuit females reported worse physical and mental health and a higher prevalence of diagnosed chronic diseases, especially mood or anxiety disorders (Table 1).
Self-reported characteristics of First Nations, Métis Inuit and non-Indigenous females of reproductive age who participated in the Canadian Community Health Survey, 2015 to 2020
First Nations females living “off reserve”
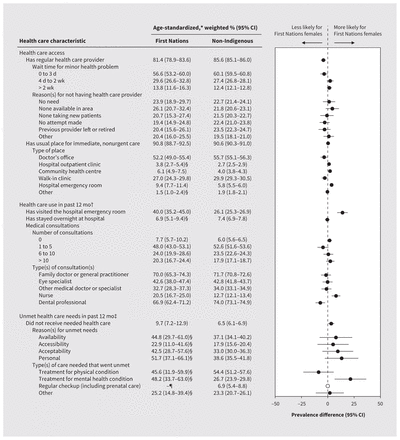
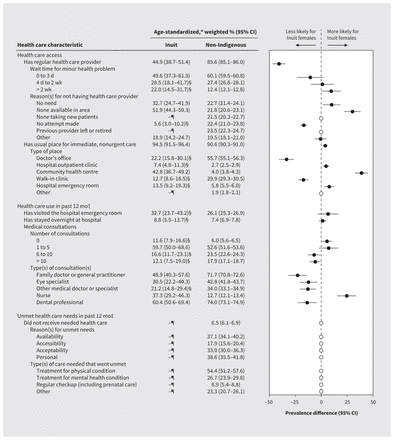
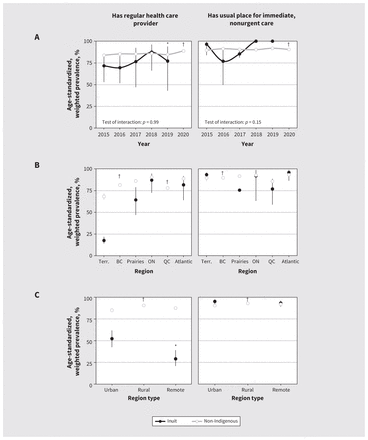
First Nations females reported lower prevalence of access to a regular health care provider than non-Indigenous females (difference −4.2%, 95% CI −6.6% to −1.8%), although wait times and reasons for not having access were similar (Figure 1 and Appendix 2, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.221407/tab-related-content). Gaps in access to a regular health care provider grew slightly in 2020 (difference 8.7%, 95% CI 1.3% to 16.1%), and were localized to the territories, Prairies and remote areas (Figure 2 and Appendix 2). First Nations females and non-Indigenous females had similar access to a usual place for immediate, nonurgent care (difference 0.2%, 95% CI −1.7% to 2.1%), even after stratification; however, 3.6% (95% CI 1.8% to 5.4%) more First Nations females accessed this care in an emergency department. In the past year, 13.9% (95% CI 8.9% to 18.9%) more First Nations females than non-Indigenous females visited an emergency department for any care, although we found no differences in overnight hospital admissions. Despite similar numbers of health care consultations, more First Nations females were seen by nurses and fewer by dental professionals. Slightly more First Nations females reported unmet needs (difference 3.2%, 95% CI 0.3% to 6.1%), especially for mental health (difference 21.5%, 95% CI 6.5% to 36.5%).
Age-standardized, weighted prevalence of health care access, use and unmet health care needs among First Nations and non-Indigenous females of reproductive age in Canada, 2015–2020. Note: CI = confidence interval. Data were not collected between April and August 2020. Depending on the measure, higher prevalence may be a positive or negative indicator of health care equity; please interpret carefully. Empty circles represent data that are not assessable. *Standardized to the 2016 Canadian Census population using 5-year age groups. †Measures of health care use were collected only in the 2015–16 cycle of the Canadian Community Health Survey. ‡Measures of unmet health care needs were optionally collected by a subset of provinces and territories (listed in Appendix 1, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.221407/tab-related-content; tabular and unstandardized data are presented in Appendix 2, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.221407/tab-related-content. Percentages of missing data for each health care variable are presented in Appendix 3, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.221407/tab-related-content). §This estimate has a coefficient of variation > 15% and ≤ 35% which, according to Statistics Canada release guidelines, represents high sampling variability; use with caution. ¶This estimate has a coefficient of variation > 35% which, according to Statistics Canada release guidelines, is too unreliable to be published.
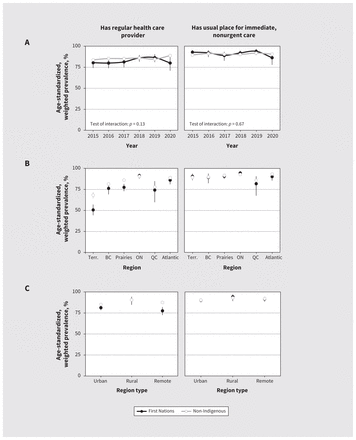
Age-standardized, weighted prevalence of health care access among First Nations and non-Indigenous females of reproductive age in Canada, 2015 to 2020. A) Prevalence by year, excluding territories. B) Prevalence by Canadian region. C) Prevalence by region type. Note: BC = British Columbia, ON = Ontario, QC = Quebec, Terr. = territories. Data were not collected between April and August 2020. Tabular and unstandardized data are presented in Appendix 2, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.221407/tab-related-content.
Métis
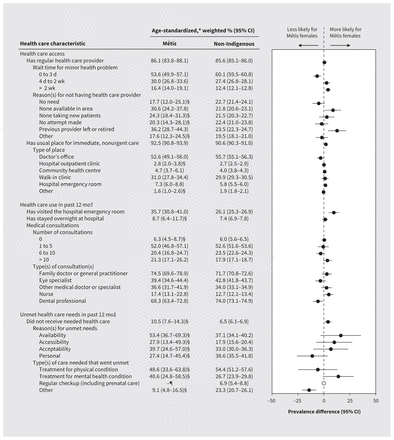
Métis females had similar access to a regular health care provider compared with non-Indigenous females (difference 0.5%, 95% CI −1.7% to 2.7%), but more reported waiting longer than 2 weeks for an appointment (Figure 3 and Appendix 2). Not having access was more often because of low availability and because their previous provider had left or retired. Slightly more Métis females had access to a usual place for immediate, non-urgent care (difference 1.9%, 95% CI 0.3% to 3.5%). After stratification by year, region and region type (Figure 4 and Appendix 2), we found no differences in access to a regular health care provider or a usual place for immediate, nonurgent care between Métis and non-Indigenous females. In the past year, 9.6% (95% CI 4.6% to 14.6%) more Métis females visited an emergency department for any care, although we found no differences in overnight hospital admissions. The number of health care consultations was similar, but 4.7% (95% CI 0.2% to 9.2%) more Métis females were seen by nurses and 5.7% fewer (95% CI −10.5% to −0.9%) were seen by dental professionals. Slightly more Métis females reported unmet needs (difference 4.0%, 95% CI 0.7% to 7.3%), especially for mental health (difference 13.9%, 95% CI −1.1% to 28.9%).
Age-standardized, weighted prevalence of health care access, use and unmet health care needs among Métis and non-Indigenous females of reproductive age in Canada, 2015–2020. Note: CI = confidence interval. Data were not collected between April and August 2020. Depending on the measure, higher prevalence may be a positive or negative indicator of health care equity; please interpret carefully. Empty circles represent data that are not assessable. *Standardized to the 2016 Canadian Census population using 5-year age groups. †Measures of health care use were collected only in the 2015–16 cycle of the Canadian Community Health Survey. ‡Measures of unmet health care needs were optionally collected by a subset of provinces and territories (listed in Appendix 1, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.221407/tab-related-content; tabular and unstandardized data are presented in Appendix 2, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.221407/tab-related-content. Percentages of missing data for each health care variable are presented in Appendix 3, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.221407/tab-related-content). §This estimate has a coefficient of variation > 15% and ≤ 35% which, according to Statistics Canada release guidelines, represents high sampling variability; use with caution. ¶This estimate has a coefficient of variation > 35% which, according to Statistics Canada release guidelines, is too unreliable to be published.
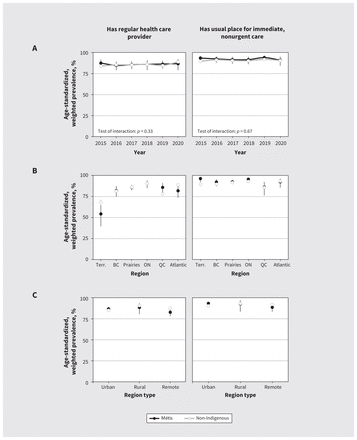
Age-standardized, weighted prevalence of health care access among Métis and non-Indigenous females of reproductive age in Canada, 2015– 2020. A) Prevalence by year, excluding territories. B) Prevalence by Canadian region. C) Prevalence by region type. Note: BC = British Columbia, ON = Ontario, QC = Quebec, Terr. = territories. Data were not collected between April and August 2020. Tabular and unstandardized data are presented in Appendix 2, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.221407/tab-related-content.
Inuit
Considerably fewer Inuit females had access to a regular health care provider than non-Indigenous females (difference −40.7%, 95% CI −47.1% to −34.3%) and more reported waiting longer than 2 weeks for an appointment (Figure 5 and Appendix 2). Not having access was more often a result of low availability than making no attempt. More Inuit females had access to a usual place for immediate, nonurgent care (difference 3.9%, 95% CI 1.5% to 6.3%), with more accessing this care at a community health centre or an emergency department. After stratification (Figure 6 and Appendix 2), gaps in access to a regular health care provider fluctuated over time (data up to 2019) and were found in the territories and Prairies, as well as in urban and remote areas. Gaps in access to a usual place for immediate, nonurgent care were also found in the Prairies. In the past year, 6.6% (95% CI −3.3% to 16.5%) more Inuit females than non-Indigenous females visited an emergency department for any care, although this difference was not statistically significant, and we found no differences in overnight hospital admissions. Additionally, 5.6% (95% CI 1.0% to 10.2%) more Inuit females had no health care consultations and, among those who did, considerably more (24.6%, 95% CI 15.4% to 33.8%) were seen by a nurse. Given Statistics Canada release guidelines, data about unmet needs and from 2020 were too unreliable to be published, based on coefficients of variation greater than 35%.
Age-standardized, weighted prevalence of health care access, use and unmet health care needs among Inuit and non-Indigenous females of reproductive age in Canada, 2015–2020. Note: CI = confidence interval. Data were not collected between April and August 2020. Depending on the measure, higher prevalence may be a positive or negative indicator of health care equity; please interpret carefully. Empty circles represent data that are not assessable. *Standardized to the 2016 Canadian Census population using 5-year age groups. †Measures of health care use were collected only in the 2015–16 cycle of the Canadian Community Health Survey. ‡Measures of unmet health care needs were optionally collected by a subset of provinces and territories (listed in Appendix 1, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.221407/tab-related-content; tabular and unstandardized data are presented in Appendix 2, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.221407/tab-related-content. Percentages of missing data for each health care variable are presented in Appendix 3, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.221407/tab-related-content). §This estimate has a coefficient of variation > 15% and ≤ 35% which, according to Statistics Canada release guidelines, represents high sampling variability; use with caution. ¶This estimate has a coefficient of variation > 35% which, according to Statistics Canada release guidelines, is too unreliable to be published.
Age-standardized, weighted prevalence of health care access among Inuit and non-Indigenous females of reproductive age in Canada, 2015–2020. A) Prevalence by year, excluding territories. B) Prevalence by Canadian region. C) Prevalence by region type. Note: BC = British Columbia, ON = Ontario, QC = Quebec, Terr. = territories. Data were not collected between April and August 2020. Tabular and unstandardized data are presented in Appendix 2, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.221407/tab-related-content. *This estimate has a coefficient of variation > 15% and ≤ 35% which, according to Statistics Canada release guidelines, represents high sampling variability; use with caution. †This estimate has a coefficient of variation > 35% which, according to Statistics Canada release guidelines, is too unreliable to be published.
Post-hoc, secondary and sensitivity analyses
In a post-hoc analysis, many disparities remained when we computed prevalence ratios adjusted for sociodemographic variables. Having a regular health care provider was still less likely for Inuit females (adjusted prevalence ratio 0.86, 95% CI 0.85 to 0.87) and First Nations females (adjusted prevalence ratio 0.98, 95% CI 0.98 to 0.99) than for non-Indigenous females (Table 2). Visiting an emergency department in the past year remained more likely for First Nations females (adjusted prevalence ratio 1.37, 95% CI 1.36 to 1.37) and Métis females (adjusted prevalence ratio 1.31, 95% CI 1.30 to 1.32). Unmet health care needs remained more likely among First Nations females (adjusted prevalence ratio 1.45, 95% CI 1.42 to 1.48) and Métis females (adjusted prevalence ratio 1.72, 95% CI 1.68 to 1.75). In a sensitivity analysis, prevalence results calculated without age standardization were similar to results of the primary analysis (Appendix 2). In secondary analyses, numerically more females with multiple or unspecified Indigenous identities reported unmet needs (difference 9.5%, 95% CI −1.6% to 20.6%) and, in contrast to all other groups, fewer had access to a usual place for immediate, non-urgent care in urban and rural areas (difference −14.2%, 95% CI −27.5% to −0.9%) (Appendix 3, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.221407/tab-related-content). Among those recently or currently pregnant, 18.6% (95% CI −24.7% to −12.5%) fewer Indigenous females had access to a regular health care provider and 16.9% (95% CI 3.2% to 30.6%) more visited an emergency department in the past year (Appendix 3). Moreover, among this group, gaps in primary care access grew numerically wider over time outside the territories, especially in 2020, and persisted in largely all Canadian regions and region types (Appendix 3). In our overall cohort, younger and socioeconomically disadvantaged people were more likely to be missing data, although they reported similar health to complete cases (Appendix 3).
Results from weighted unadjusted and adjusted log-binomial multivariable regression*
Interpretation
We found that “off-reserve” First Nations, Métis and Inuit females reported higher morbidity and continue to face various disparities in health care access, use and unmet needs. Specifically, fewer Indigenous females reported having access to a regular health care provider, especially in the territories and Prairies; more waited longer for an appointment; and more used hospital services for nonurgent care. Despite more Indigenous females visiting an emergency department to access care, similar numbers were admitted overnight, possibly because they sought nonurgent care or, in some instances, as a result of racism in triage.33 As well, while more Indigenous females had health care consultations with nurses, fewer had them with eye and dental professionals, despite additional health care coverage for these types of care among First Nations and Inuit females.34 Consistent with these disparities, more First Nations and Métis females reported unmet needs, especially for mental health care. After sociodemographic adjustment, health care disparities persisted, suggesting that systemic barriers, such as racism leading to distrust of health care systems, may be chiefly responsible.
These findings did not surprise our Indigenous advisors. Although our health care system is centred on care providers who know and guide their patients,35 care for Indigenous Peoples has never mirrored this ideal. In remote areas outside of “reserves,” many Indigenous people rely on visiting health care providers who rarely return to provide longitudinal care.36 Even when primary care is accessible, culturally safe and traumainformed care rarely is, as few are trained to deliver such care; systemic racism and discrimination, however, continue to be pervasive.5,10,16,37–40 Indigenous people living “off reserve” also experience higher levels of mobility in Canada, which limits continuity of care.41 Indigenous people are therefore left to make an impossible choice: navigate the system alone and repeatedly recount their medical history to new health care providers who have not had the opportunity to build trust with them, or receive no care at all.38,42–44 Although, to our knowledge, no previous studies focused on females and few distinguished between Indigenous identities, all consistently reported disparities in primary care access, use and unmet needs among Indigenous Peoples in Canada.38,39,43–49 They additionally saw similar regional variations, which they attributed to decisions on health care spending and allocation.50 Meanwhile, the COVID-19 pandemic has magnified these issues, prompting national staff and supply shortages35 and widening gaps.39,49 Despite limited pandemicera data, we also found widening gaps in primary care access among recently or currently pregnant Indigenous females in 2020.
To strive toward health care reconciliation,51,52 culturally safe primary care for Indigenous females is urgently needed. As fewer Canadian medical graduates specialize in family medicine every year,53 our Indigenous advisors and others54 suggest leveraging more accessible health care providers to reduce the disparities we found in primary care access. Indigenous communities are already leading this charge, restoring the traditional practice of midwifery55,56 to deliver healthy babies in their own communities,57,58 including in remote,59 “on-reserve”60 and urban61 settings across Canada. Besides perinatal care and education, midwives could provide nearly all essential sexual and reproductive care across the life course when fully trained and licensed,62 including screening and treatment of sexually transmitted infections, contraceptive services and abortion care. Additional solutions to reduce disparities include creating health care spaces that are safe, supportive and tailored to Indigenous Peoples; mandating cultural competency training for health care providers; and standardizing health care policies between levels of government.63,64 Above all, solutions must acknowledge the effects of colonialism on health care63 and the distinctions-based Indigenous concepts of health, which view individual health as inseparable from that of the community and environment.65
Limitations
Given CCHS exclusions, our findings are not generalizable to the 44% of First Nations people living on “reserve,”66 nor to incarcerated or institutionalized populations, all of whom experience unique barriers to care. Moreover, our analysis is limited by the reductive classification of Indigenous females into 3 heterogenous groups and of non-Indigenous females together. As 29% of the reference group self-identified as belonging to racialized communities (which also experience discrimination in health care), this may explain why some disparities were modest. Selection and self-report biases may have affected our findings, given the low response rates to the CCHS survey, sensitive topics discussed and distrust felt by many Indigenous Peoples. No information was collected on culturally safe care or quality of care. Questions grouped all nurse types, including nurse practitioners, together. In addition, the CCHS did not ask about gender identity until 2019, limiting our analysis to those who were assigned female at birth. In 2020, data were collected for only 4 months during the pandemic, limiting our ability to assess its full impact on disparities. Lastly, our findings are restricted to Western medical care, which Indigenous females may be wary to seek, thereby limiting our knowledge of care sought elsewhere. Although these limitations unequally affect their communities’ data, our Indigenous advisors approved the CCHS as it was the only available data set to quantify national health care disparities; this lack of adequate data is likely a legacy effect of colonization and “othering,” and underscores calls from our Indigenous advisors and others67 for better Indigenous health data practices and community engagement by survey developers.
Conclusion
“Off-reserve” Indigenous females of reproductive age in Canada face increased health care needs, owing to higher morbidity, but have less access to primary care, increased use of hospital services for nonurgent issue, and more unmet needs, impeding advances toward health equity. To alleviate these disparities, our Indigenous advisors recommend that Canada leverage more accessible and culturally competent health care providers and that survey developers try to fill outsized gaps in Indigenous health data. Future work should monitor these disparities over time and fill large gaps in our findings, such as by ascertaining data on “reserves.”68
Acknowledgements
The authors would first like to acknowledge the First Nations, Métis and Inuit Peoples, communities and Nations across Canada and Turtle Island, noble custodians of traditional and unceded territories on which this manuscript was written. The authors from the Public Health Agency of Canada (PHAC) would also like to acknowledge the individuals and organizations who helped shape and support the research from the onset and interpret the data through their wisdom, viewpoints and lived experiences, including our Indigenous Advisory Committee, composed of representatives from Les Femmes Michif Otipemisiwak — Women of the Métis Nation (Melanie Omeniho, Lisa Pigeau, Victoria Pruden), Native Women’s Association of Canada (Lee Allison Clark, Dr. Keri Cheechoo, Lynne Groulx, Holly Patterson, Lisa Poulin, Mindy Smith), Pauktuutit Inuit Women of Canada (as requested, names not listed based on organizational policy to speak as one collective voice), 2 Spirits in Motion (Dr. Jonathon Potskin), and Dr. Leason from the University of Calgary. The authors are also deeply grateful for the support of the federal government’s Indigenous Women’s Advisory Committee. A detailed account of the engagement process is presented as part of the Guidance for Reporting Involvement of Patients and the Public reporting guideline in Appendix 1 (see www.cmaj.ca/lookup/doi/10.1503/cmaj.221407/tab-related-content); the authors hope it may serve as a starting point for future community-based participatory research involving Indigenous communities. Authors from PHAC also extend their sincere thanks to Dr. Margaret de Groh from the Applied Research Division (PHAC) and to colleagues from the Indigenous Relations Team (PHAC); the Surveillance Health Information Policy and Coordination Unit Team (Indigenous Services Canada); and the Centre for Indigenous Statistics and Partnerships (Statistics Canada) for taking the time to provide feedback throughout the project. This research would not have been possible without the voices of these Indigenous leaders, health researchers, and policy analysts. Meegwetch!
Footnotes
↵* Sebastian Srugo and Christina Ricci contributed equally to this work. Collaborators are listed in the acknowledgements.
Competing interests: Christina Ricci and Sebastian Srugo receive salary support from the Public Health Agency of Canada (PHAC). Chantal Nelson reports receiving payment as a contract instructor from Lakehead University and Carleton University. No other competing interests were declared.
This article has been peer reviewed.
Contributors: Sebastian Srugo and Christina Ricci conceived the study. Sebastian Srugo analyzed the data and drafted the manuscript. All of the authors and collaborators from our Indigenous advisory group contributed to designing this study (but none were involved in designing the Canadian Community Health Survey), interpreting the data, and revising the manuscript critically. All of the authors gave final approval of the version to be published and agree to be accountable for all aspects of the work.
Data sharing: Data contained in these tables are based on the Canadian Community Health Survey (CCHS), Statistics Canada, 2015 to 2020. Data from this study cannot be shared publicly owing to confidentiality agreements between Statistics Canada and participants of the CCHS. To access the data, researchers must apply to Statistics Canada (https://www.statcan.gc.ca/en/microdata). Program files are available from the corresponding author, Sebastian Srugo.
Disclaimer: The content and views expressed in this article are those of the authors and do not necessarily reflect those of the Government of Canada.
- Accepted July 7, 2023.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/