Canadian doctors need to stop prescribing high doses of opioids to patients with pain and slowly taper off patients already on high doses, urged experts at the federal Opioid Conference Nov. 18 in Ottawa.
“If opioids were a new drug ... they would almost certainly be pulled,” said Dr. Jason Busse of the Michael G. DeGroote National Pain Centre in Hamilton, Ontario. The benefits of opioids are “statistically significant but clinically small,” and “you’ll get the same level of improvement whether you are prescribed a low or high dose,” he explained.
“We know that 100% of patients engaged in long-term opioid therapy will develop dependence,” Busse said. As patients develop tolerance, that means “higher doses, higher risk of addiction, higher risk of overdose, higher risk of fatal overdose.”
Busse and other experts advocated for better prescribing guidelines, stronger monitoring and consequences for overprescribing, as well as efforts to discourage patients from starting or continuing opioids.
Current Canadian and American guidelines on opioid prescribing are “more eminence based than evidence based,” that is, heavily informed by expert opinion rather than hard data, said Busse. For example, the United States Centre for Disease Control recommendations on the benefits of opioids for chronic non-cancer pain “considered a total of zero published studies,” he said. For the updated Canadian guidelines, due to be submitted to a journal by March, “we’re considering 104 published randomized controlled trials.”
The new guidelines won’t be popular with the drug companies, noted keynote speaker, Dr. David Juurlink, who is part of the team developing the guidelines. He’s also the head of Clinical Pharmacology and Toxicology, Sunnybrook Health Sciences Centre in Toronto. “They aren’t going to be popular with doctors who think they’ve been doing it right all along by prescribing extraordinary doses, but the notion that high doses of opioids is an intervention that affords patients benefits in excess of harms is a notion that can’t die out soon enough.”
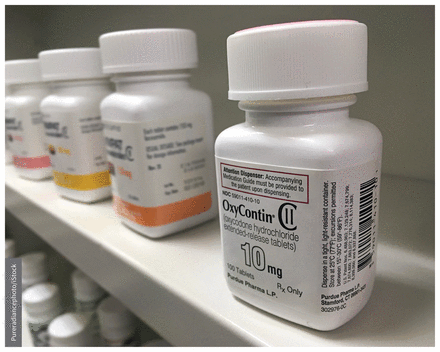
Experts at a federal opioid conference on Nov. 18 urged a variety of measures to slash prescribing of the drugs.
Image courtesy of Pureradiancephoto/iStock
Juurlink said Canadian doctors have opened a “bit of a Pandora’s box and flooded the market with drugs that don’t work as well as we were taught and aren’t as safe as we were taught.”
How did this happen?
“We really have been misled about the role of these drugs and how to use them, by companies who have made billions of dollars in the process. It’s time for some de-education,” Juurlink told CMAJ.
During his address, Juurlink delved into the evolution of the current problem. For example, Purdue Pharma’s educational materials included a free book which was distributed to most Canadian medical students. It downplayed oxycodone’s negative effects, stating, for example, that the risk of addiction was only 1%. Juurlink says there’s no evidence this is true.
But physicians wanted to be able to help patients with chronic pain. “It was a message we wanted to hear, so sales have gone through the roof.”
Purdue pled guilty to misbranding its product in the United States and paid $600 million in damages in 2007.
Federal Minister of Health Dr. Jane Philpott echoed Juurlink’s concerns, telling the conference’s 250 invited attendees that Canada’s dispensing levels are the second highest in the world, “… and those dispensing levels are strongly associated with harm … . People can transition from prescription use to problematic use and sometimes seeking drugs illicitly.”
Properly used, opioids can help people in serious pain, said Philpott. “We need to balance the risks with the benefits and make sure there are appropriate safeguards in place.”
“We can’t prescribe them as we have in the past 20 years,” added Juurlink. “We’ve caused so much harm to pain patients with that practice.”
It’s hard to justify starting with doses more than 50–60 mg/d, he told CMAJ. “By the time you get into the 100s [of mg/d] that’s a testament of the failure of opioids to solve your patient’s problem. Some patients are taking 1000 mg/d; he knows of one taking 5000.
But he cautions doctors against abandoning patients and cutting them off. “I can’t say that strongly enough. When that happens it’s a disaster. The patient goes into withdrawal and will take whatever they can get their hands on.” He advocates slowly tapering down doses but acknowledges that won’t work in all cases.
Efforts to reduce opioid prescribing should be paired with increased access to non-drug treatments for pain, emphasized many speakers.
“Patients living with chronic pain need alternatives,” said Busse. “Things like mindfulness training, cognitive behavioural therapy ... these things show evidence of working but they’re not readily available and for too many patients living with chronic pain they’re simply unaffordable.”
Initiatives
Medical regulators need to hold prescribers accountable for following the opioid guidelines, said Dr. Karen Mazurek, deputy registrar at the College of Physicians and Surgeons of Alberta. The college has written a draft standard of practice requiring physicians to do so. “If they can’t they have to provide a good reason and it must be written on the chart,” Mazurek said.
In 2017, the college is also going to run quarterly large-scale audit and feedback interventions. “Monitoring high-risk patients and high-risk prescribers is not enough,” she explained. “We need to make sure those guidelines reach every single physician in this country.” To do that, medical regulators need “real-time data” on opioid prescribing, Mazurek said.
Electronic prescribing can also help mitigate harms. Canada Infoway has received $40 million in federal funds to develop a national electronic prescribing system to replace paper prescriptions, which can be lost, forged or filled at multiple pharmacies, said Michael Green, president and CEO of the agency.
The new e-prescription system will provide a direct link between prescribers and pharmacists, and capture data on “all prescriptions, not just dispensed drugs.” This information will be fed back to provincial and territorial prescription monitoring programs, Green said. Infoway will test the system in Ontario and Alberta by March 2018.
In addition to closer monitoring of prescribing, other experts urged increased patient education about the risks of opioids. “Professional standards include requirements to communicate the harms and risks of opioid use and this needs to be mandatory,” said Sylvia Hyland of the Institute for Safe Medication Practices Canada. “If patients are well aware of the harms ... and they’re aware of the alternative options they’ll be in better position to make informed decisions.”
“We’re working with neighborhood pharmacies to develop specific information to give patients and families, not only when a prescription is filled but when the patient comes back for a refill,” she said.
Dr. Cara Tannenbaum of the Canadian Deprescribing Network noted the success of a similar intervention that involved giving patients information about benzodiazepines, in which one in four discontinued the drug. She also suggested linking opioid prescriptions to the renewal of drivers’ licenses.
“In Denmark, the government said we won’t renew your driver’s license if you’re on benzodiazepines ... the reduction in benzodiazepines was 66%,” Tannenbaum explained. “It says on the oxycodone label: do not operate heavy machinery, do not drive under the influence. Should there be a Canadian policy that holds people accountable?”
The Canadian Medical Association also recognizes that opioid prescribing patterns are “one of many contributing factors to this crisis.” The CMA is committed to working with partners to develop a “coherent and comprehensive national strategy,” stated Past-President Dr. Cindy Forbes.











