A 32-year-old heterosexual Japanese man presented with a 2-week history of painful gangrene-like cheilitis (Figure 1A) and generalized asymptomatic pustular eruptions (Figure 1B). He had a history of HIV infection and was undergoing antiretroviral therapy. His latest CD4 count was 0.53 × 109/L. He had had sexual intercourse with a female partner several weeks before presentation. There were no noticeable genital ulcers. Blood tests showed no remarkable abnormalities except for a positive rapid plasma reagin test result at a titre of 1:256 and a positive Treponema pallidum hemagglutination assay. We diagnosed secondary syphilis and started the patient on oral amoxicillin 3 g/d and probenecid 750 mg/d for 2 weeks, as part of a regimen that has been suggested in Japan.1 Although World Health Organization guidelines recommend intramuscular administration of benzathine penicillin G 2.4 million units in a single dose for treating infectious syphilis in adults and adolescents, including people living with HIV,2 benzathine penicillin G is unavailable in Japan. All symptoms resolved 1 week after treatment without any complications. We were unable to contact the patient’s partner and advised the patient to notify her.
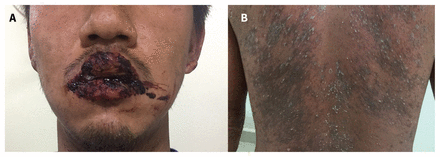
(A) Painful gangrene-like lesions on the lips of a 32-year-old man with HIV infection and secondary syphilis. (B) Asymptomatic pustular eruptions on the patient’s back.
Secondary syphilis is known to have variable clinical symptoms; in particular, symptoms can be atypical in patients with HIV infection.3 Although various oral manifestations occur in patients with secondary syphilis, the most common presentation consists of slightly elevated plaques and oval-shaped ulcers; gangrene-like cheilitis is uncommon. Similarly, skin lesions usually present as symmetric macular, papular or maculopapular lesions; however, patients sometimes develop pustular lesions.3
Syphilis is widespread globally and still imposes a substantial global health burden.4 Clinicians should be aware of uncommon lesions that can occur in patients with syphilis, not only to achieve appropriate diagnosis and treatment, but also to prevent the spread of infection.
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
The author has obtained patient consent.