Mortality after imprisonment
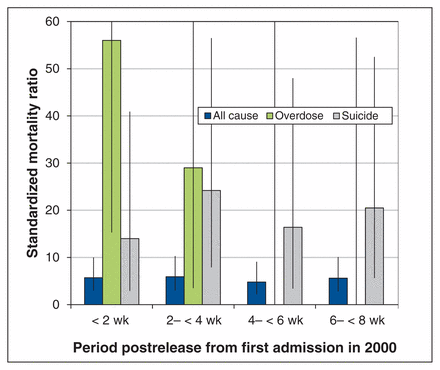
International research shows that those who experience incarceration have poor health compared with the general population. Is the same true in Canada? This retrospective study linked data on adults admitted to provincial custody in Ontario in 2000 with data on deaths between 2000 and 2012, comparing them with data for the general population. Of the 48 166 included in the final sample, 90.1% were men; 69.0% identified themselves as white, 12.4% as black and 7.2% as Aboriginal. The crude death rate (in custody or after release) was 7.1 (95% confidence interval 6.9–7.3), with a mean age at death of 47.5 years. The most common causes of death were injury and poisoning (38.2%), including overdose (13.6%) and suicide (8.2%), and cardiovascular diseases (15.8%) and neoplasms (14.5%). Rates of suicide and overdose were higher in the first few weeks after release (Figure 1). Life expectancy for those incarcerated in 2000 was 72.3 years for women and 73.4 years for men, which is 10.6 years less for women and 4.2 years less for men compared with the general population. Those who have spent time in custody should be recognized as being at increased risk of death, say the authors. CMAJ Open 2016;4:E153–61.
Standardized mortality ratio for all causes, overdose and suicide, by period postrelease from first admission to provincial custody in 2000, n = 46 442. Standardized to the Canadian population in 2000; 95% confidence intervals shown with vertical lines. (Excludes 960 people who were transferred to federal custody.)
Disclosing HIV serostatus to sexual partners
In October 2012, the Supreme Court of Canada ruled that people living with HIV must disclose their HIV status before having sex that poses a “realistic possibility” of HIV transmission. The court further clarified that the realistic possibility of transmission was negated in circumstances where condoms were used, penile–vaginal intercourse occurred and the viral load was low (< 1500 copies/mL). The authors sought to determine what proportion of people living with HIV would face a legal obligation to disclose, by analyzing cross-sectional survey data from a cohort of 176 people (44% women) in Vancouver living with HIV who inject drugs. Most of those in the study (94%) had a low viral load, and 60% self-reported condom use. If both condom use and a viral load of less than 1500 copies/mL were required to avoid criminal liability for HIV nondisclosure, about 44% of those in the study would face a legal obligation to disclose. Factors associated with having to disclose included female sex, having 1 recent sexual partner (v. more than 1) and self-reporting a stable relationship (Table 1). The authors point out that current case law in Canada may disproportionately affect the most marginalized and vulnerable women living with HIV, which reinforces the need for public health initiatives to address barriers to HIV treatment and support safe HIV status disclosure within marginalized communities. CMAJ Open 2016;4:E169–78.
Bivariable and multivariable logistic regression analyses of factors associated with facing a legal obligation to disclose HIV serostatus to sexual partners among 176 people living with HIV who inject drugs