Abstract
Background: Medical Savings Accounts are an attempt to reduce health care costs by transferring responsibility for expenditures to patients, while providing them with state-supported base amounts to cover some of the costs. We wondered whether such a system would actually be effective, given the fact that medical care expenditures (and illness) are unequally distributed across the population.
Methods: We used the Manitoba Population Health Research Data Respository to assess costs incurred by individual residents of Manitoba for all physician visits and admissions to hospital between 1997 and 1999, and we calculated an average expenditure per person per year over the 3 years.Results: During fiscal years 1997–1999, physician and hospital costs that could be attributed to individual Manitoba residents averaged $730 each year. Most users accounted for very little expenditure. About 40% of the entire population of Manitoba used less than $100 each, and 80% used less than $600. The highest-using 1% of the Manitoba population accounted for 26% of all spending on hospital and physician care, whereas the lowest-using 50% accounted for 4%. When examined by age category, the results were similar. Even in the highest age category, most of the population falls into the low-usage category. If the entitlement under a Medical Savings Account scheme was set at the current average cost of $730 per year, then total spending by government on health care for this healthy group would increase (by $505 million) rather than decrease. If the “catastrophic threshold,” above which the insurer would pay costs, was set at $1000 per year, then the sickest 20% of Manitoba residents would become personally responsible for just over $60 million of current health care costs. The net result is a 54% increase in spending on hospital and physician costs that can be allocated to individuals.
Interpretation: Medical Savings Accounts will not save money but will instead, under most formulations, lead to an increase in spending on the healthiest members of the population.
How should Canadian medicare be updated for the 21st century? One suggestion has been to replace direct payments to health care providers by Medical Savings Accounts (MSAs), which would allow individuals to decide when and where they would get health care and, thereby, improve access to services not currently covered by medicare. Proponents argue that this would reduce costs by encouraging more responsible behaviour by patients and would increase choice.1,2,3 Solomon puts the savings at $6 billion per year in primary care costs alone.4 Detractors of the plan suggest that MSAs compromise equity by transferring resources from the sick to the healthy and from the poor to the relatively better off, and may not be feasible when applied to those with chronic poor health.5,6 Hurley7 and Schaafsma8 have argued that MSAs are unlikely to control expenditure effectively. Analysis of experiments, particularly in Singapore, yields mixed results.9 What has been missing is Canadian data.
MSAs can be formulated in a variety of ways. The common feature is that individuals receive “entitlements,” which may be based on factors such as age and sex, or past health care use, from the provincial government. This allowance would be used to pay for routine medical care up to a pre-set amount. An insurer (government or private) would pick up costs above a defined “catastrophic” threshold. Between the entitlement and the catastrophic level is a “corridor.” Costs that fall within the corridor would be the responsibility of the individual. Publicly paid health care costs would accordingly depend on the specific design of such plans, particularly the levels at which the entitlement and the catastrophic thresholds were set, the extent (if any) of copayments above the catastrophic threshold and the rules governing surplus funds. In some cases, any surplus can be kept to use for noninsured services or future health care costs, while in others they are given on a “use it or lose it” basis.
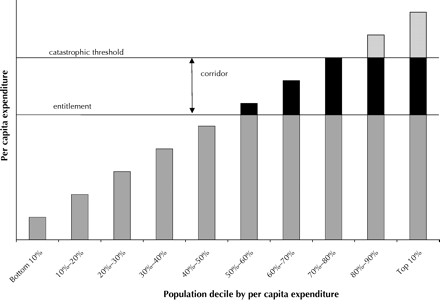
The higher the entitlement and the lower the catastrophic threshold, the greater the public responsibility for health care costs (see Fig. 1).
Fig. 1: Hypothetical distribution of per capita expenditures, in which individuals are given an entitlement represented by the lower line and are expected to pay all physician and hospital costs up to that level out of the entitlement. There are no copayments for physician and hospital costs above the catastrophic cost threshold, which, in this case, would be paid by the government. Spending that falls into the corridor between the entitlement and the catastrophic cost lines is the main target for creating efficiencies. Individuals must either forgo such expenditure or pay for it out of pocket.
The lines representing the entitlement and the catastrophic threshold can be set at different levels, and might vary by age and sex or by the individual's past health experience. The net financial effect depends upon 3 factors: the levels at which the entitlement and the catastrophic threshold are set; what individuals who spend less than their entitlement are allowed to do with the surplus; and how much expenditure falls into the corridor.
Regardless of the clinical and ethical implications of these models, from an economic viewpoint most formulations of MSAs are aimed at those individuals spending a moderately high amount, whose total expenditure falls into the corridor. Those patients currently incurring catastrophic costs are in little position to reduce their expenditure and would have no incentive to do so, because most models attempt to shield these patients, at least in part, from their full bills. Patients who currently use less than their entitlement would have no reason to reduce their use of health care services, unless they were permitted to either accumulate savings for future health care costs or redirect savings toward currently uninsured services. Their per capita expenditure is small to begin with, limiting the potential savings from this group. If the range of services to which they can direct their entitlement is expanded beyond currently covered services, or they are allowed to keep the surplus, total expenditure for this healthy group might increase. If any use of the health care system is forgone to conserve the future value of the MSA or to avoid approaching the corridor, it will be greatest among the disadvantaged. If some of this forgone service is for preventive care or early intervention, health status could be compromised and future health care costs may rise.
Methods
The Manitoba Population Health Research Data Repository captures standardized data based on almost every physician and hospital contact in Manitoba. This information (including patient identification numbers, physician claims, diagnoses, costs, hospitalization and institutionalization data) is maintained and controlled by the provincial department of health, Manitoba Health. All records deposited in the repository have been processed by Manitoba Health to remove patient identifiers such as name and address, while preserving the capacity to link records together to form individual histories of health care use. The database includes direct information on physician billings, excluding some patient visits outside the province and some physician salaries (i.e., those of trainees and those paid for specific services such as ICU coverage).10 The costs of inpatient hospital care and day surgery procedures have been estimated by applying the Manitoba average cost per weighted case to each discharge.11 Total cost of care for an inpatient or day surgery patient includes all physician services received during the hospital stay. This study looks only at physician visits and hospital stays, the core services fully insured under the Canada Health Act. (Additional analysis, which we are currently planning, will look at other costs such as pharmaceutical drugs and home care, which different provinces cover differently.) We first assigned costs to individuals, then divided the population into deciles based on their annual expenditure. If health care use were evenly distributed across the population, then the lowest-using 50% would be incurring about 50% of the cost.
In any one year, some individuals are in the high-cost category because they are chronically ill, whereas others are there only temporarily because of fleeting ill health. Most MSA formulations allow individuals to allocate surpluses in one year to extraordinary costs in subsequent years. We calculated the average annual expenditure for each resident of Manitoba over the 3-year period from 1997 to 1999. This captures, in part, the extent to which some individuals are persistently high- or low-cost users of the system, because it represents typical costs faced by an individual. If we used single-year data, the results would be much more skewed. (Full analysis requires more elaborate modelling over a longer time period.)
Results
Based on our data for fiscal years 1997–1999, the average resident of Manitoba accounts for $730 spent each year on physicians and hospitals. This figure is lower than that reported by the Canadian Institute for Health Information (CIHI),12 because we allocated costs to individual patients and then aggregated the results. Some costs are not captured in our analysis, either because they are not attributable to individual patients (such as the costs of running some clinics in hospitals) or because we have no patient-specific data, as in the case of costs attributable to Northern nursing stations, blood products or CancerCare Manitoba. Finally, our methodology accounts for hospital costs differently from that of the CIHI.12
Manitoba data show that most users fall into the very low usage category, with few gains to be had from reductions in resource use. Indeed, 40% of the population used less than $100 each for physician and hospital services combined (Fig. 2); 80% used less than $600. A small, but very expensive, proportion fall into the catastrophic costs category, which would still be paid by some form of government insurance under many formulations of MSA models. These individuals have little control over their use of resources, both because they are very sick and because they have often been admitted to hospital. Hospital costs are largely beyond the control of the patient. For the 3-year average, we found that the highest-using 1% of the Manitoba population accounted for 26% of spending on hospital and physician care, whereas the lowest-using 50% accounted for 4%.
Fig. 2: Annual per capita expenditure (hospital and physician) by decile, Apr. 1, 1997, to Mar. 31, 2000.
Our data also show that costs for physician services are almost as skewed as total costs. A more limited MSA model expected to cover only physician services would confront the same problems.
Neither can the model be salvaged if (as would surely be the case) payments were tailored to each age–sex category. Table 1 shows per capita expenditure by decile for each population subgroup and further divides the highest decile into subgroups. Even within age categories, most people either fall into the low-usage category in which few savings are to be had, or into the catastrophic cost category, where they have little control over the costs they incur.
Table 1.
Interpretation
It is important to note that different versions of MSAs will change the precise financial outcomes. We are beginning such modelling exercises. Our results suggest that no feasible model can significantly reduce costs unless the entitlement is set so low and the catastrophic threshold so high that there is no longer reasonable insurance against health care costs.
What is the bottom line on costs? Suppose we set the entitlement at the mean expenditure, $730 per resident with no adjustment for age and sex. Some 80% of the population are currently using less than the entitlement. None of these individuals would have any incentive to reduce their health care costs unless they were permitted to allocate any surplus toward currently uninsured services or to save it for future health care costs. If they could allocate the surplus to services other than physicians and hospitals, government spending for this healthy group of Manitoba residents could well increase. In an extreme case, in which individuals were given the entitlement and allowed to invest the surplus or use it for other purposes, expenditure on this group would increase from an average of $167 to $730 a year. This would increase spending on this healthy group by slightly more than $505 million per year.
If we set a catastrophic threshold at $1000, the sickest 20% of Manitobans would find themselves responsible for just over $60 million of health care costs. Most of this amounts to a tax on the sickest members of society, who would have to pay all costs between $730 and $1000. There are few opportunities for people to react to the incentives created by MSAs, because few people have total costs that fall into the corridor. However, if individuals start to forgo medically necessary treatment, inappropriate cost- consciousness may well increase the burden of catastrophic coverage in future years.
The net effect of increasing spending on the healthy by $505 million and reducing spending on the sick by $60 million is that the burden on the provincial health care budget increases by $445 million per year. This represents a 54% increase in the costs that we were able to attribute to individuals for physician and hospital costs.
Results will vary depending on how and at what levels the entitlements and catastrophic thresholds are set. No formulation will save the province money unless it imposes heavy taxes on the sickest individuals or sets the entitlement so low as to, in effect, eliminate insurance coverage. Contrary to assumptions that individuals make unnecessary use of the system, or that health care use is relatively evenly distributed, our findings emphasize that the majority of provincial residents already make few demands on the system.
Proponents of MSAs have argued that these mechanisms can reduce costs, while giving people more control and expanding access to services not currently provided. Our results suggest that MSAs will not save money but will instead, under most formulations, lead to an increase in spending on the healthiest members of the population. MSAs may indeed be able to increase access and choice, but they will do so by driving up costs, with little attention to the appropriateness or health benefits of this increased spending. When one adds to the mix concerns about equity and implications for preventive care, MSAs have very little to recommend them. It is past time that they be buried.
Footnotes
-
This article has been peer reviewed.
Contributors: Evelyn L. Forget was involved in the design of this project and data interpretation and wrote the first draft. Raisa Deber had the original idea for this project, contributed to its design and made critical revisions to the manuscript. Leslie L. Roos was involved in the study design and data acquisition and analysis. He also made critical revisions to the manuscript.
Acknowledgements: We would like to thank Randy Walld for his superb assistance with the data analysis.
Funding from the Canadian Population Health Initiative supported this study. The results and conclusions are those of the authors; we are indebted to Health Information Services, Manitoba Health, for providing data. No official endorsement by Manitoba Health is intended or implied.
Competing interests: None declared.