Abstract
BACKGROUND: Analgesics that contain codeine are commonly prescribed for postoperative pain, but it is unclear how they compare with nonopioid alternatives. We sought to compare the effectiveness of codeine and nonsteroidal anti-inflammatory drugs (NSAIDs) for adults who underwent outpatient surgery.
METHODS: We conducted a systematic review and meta-analysis of randomized controlled trials comparing codeine and NSAIDs for postoperative pain in outpatient surgery. We searched MEDLINE and Embase from inception to October 2019 for eligible studies. Our primary outcome was the patient pain score, converted to a standard 10-point intensity scale. Our secondary outcomes were patient-reported global assessments and adverse effects. We used random-effects models and grading of recommendations assessment, development and evaluation (GRADE) to assess the quality of evidence.
RESULTS: Forty studies, including 102 trial arms and 5116 patients, met inclusion criteria. The studies had low risk of bias and low-to-moderate heterogeneity. Compared with codeine, NSAIDs were associated with better pain scores at 6 hours (weighted mean difference [WMD] 0.93 points, 95% confidence interval [CI] 0.71 to 1.15) and at 12 hours (WMD 0.79, 95% CI 0.38 to 1.19). Stronger NSAID superiority at 6 hours was observed among trials where acetaminophen was coadministered at equivalent doses between groups (WMD 1.18, 95% CI 0.87 to 1.48). NSAIDs were associated with better global assessments at 6 hours (WMD −0.88, 95% CI −1.04 to −0.72) and at 24 hours (WMD −0.67, 95% CI −0.95 to −0.40), and were associated with fewer adverse effects, including bleeding events.
INTERPRETATION: We found that adult outpatients report better pain scores, better global assessments and fewer adverse effects when their postoperative pain is treated with NSAIDs than with codeine. Clinicians across all specialties can use this information to improve both pain management and opioid stewardship.
Outpatient surgical procedures are now more common than inpatient procedures, given the development of less invasive techniques, the drive for health care efficiency, and improvements in anesthesia and pain management. 1–4 Postoperative pain management after outpatient procedures often includes low-potency or low-dose opioids.5 Codeine use is widespread in this setting and codeine remains the most commonly prescribed opioid in many countries, including Canada.6–9 However, its efficacy is variable, its potency is low and its use is associated with risks of severe adverse effects and misuse.10 Amid the ongoing opioid crisis, management of pain and potential opioid misuse is important across all medical and dental specialties.11
Nonsteroidal anti-inflammatory drugs (NSAIDs) are an alternative to low-potency opioids. The potency, effects and toxicity of NSAIDs depend on the degree to which they inhibit cyclooxygenase 1 and 2 activity. Their main adverse effects are gastrointestinal bleeding, renal impairment and myocardial infarction with long-term use.12–15 Postoperative pain can be effectively managed with NSAIDs, and NSAIDs have been shown to reduce opioid consumption in postoperative patients.16
Given how commonly these medications are used, and the uncertainty in their comparative efficacy and safety, we sought to compare pain and safety outcomes for codeine-based medications and NSAIDs among adults who underwent outpatient surgery through a systematic review and meta-analysis of randomized controlled trials (RCTs).
Methods
We report this meta-analysis according to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines.17
Search strategy and study selection
With the assistance of a medical librarian, we systematically searched MEDLINE and Embase from inception to Oct. 28, 2019. Our search strategy is described in Appendix 1, eTables 1 and 2, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.201915/tab-related-content.
We included RCTs that compared oral codeine with oral NSAIDs prescribed to adult outpatients having acute postoperative pain. Our primary outcome of interest was efficacy, defined as the level of pain, measured by a validated pain scale. Secondary outcomes included patient-reported post-treatment global assessment score, and safety, measured by reported adverse effects. We included trials in which acetaminophen was coadministered with codeine or NSAIDs. We excluded trials in which intravenous drugs or drugs other than acetaminophen were coadministered. We also excluded trials that used medications that are no longer available because of safety concerns (e.g., zomepirac, indoprofen).
Using a standardized, pilot-tested form, 2 physicians screened titles and abstracts. The same physicians subsequently reviewed full texts of potentially eligible studies, independently and in duplicate, to assess for inclusion. They resolved disagreements with discussion.
Risk of bias assessment
We assessed individual studies’ risk of bias using the Cochrane risk of bias assessment tool, which includes assessment of random sequence generation, allocation concealment, blinding of participants and personnel, outcome assessment, incomplete outcome data, selective reporting and other sources of bias.18 Two authors assessed risk of bias, independently and in duplicate, and resolved disagreements by discussion. For the purposes of subgroup testing based on risk of bias, we dichotomized studies into high or low risk; we considered studies high risk if they had more than 1 bias category rated as high risk.
Data extraction
We developed and piloted a standardized, data extraction form. A single author extracted data, which was then verified independently by a second author. We collected study characteristics, patient characteristics, interventions and outcomes. Our primary outcome was pain, measured on a 10-point scale. If studies reported more than 1 pain score, we preferentially used the patient-reported pain intensity score in the following order: 10-point scale, visual analogue scale, pain intensity difference score or sum of pain intensity difference. In the absence of these options, we used pain relief, mean peak pain relief or total pain relief, in that preferred order. We converted all pain measures to a 10-point scale to facilitate comparison. We collected data on pain scores at 0 to 6 hours, 6 to 12 hours, 12 to 24 hours, 24 to 48 hours, 48 to 72 hours and more than 3 days after treatment. Our secondary outcomes were global assessments, on a 4-point scale, and adverse effects. We extracted all reported outcomes of adverse effects.
When multiarm trials included ineligible treatment arms, we extracted data only on the treatment arms meeting our eligibility criteria. When more than 1 arm within a single trial was eligible for inclusion (e.g., 1 codeine arm and 2 NSAID arms) we halved the “shared” group into 2 groups with halved sample size, then performed 2 direct comparisons, per Cochrane methodology.19 This method was chosen despite its limitations to allow separate trial arm comparisons for subgroup testing. We checked manuscripts by the same authorship for double-counting.
Statistical analysis
We calculated the Cohen κ statistic to evaluate interrater agreement. We converted all continuous outcome measures to a common reference scale, namely a 10-point scale of pain intensity (where lower is better) and a 4-point global assessment scale (where higher is better).20 If pain scores were reported using a scale where higher is better (opposite to the direction of the standard scale), then we inverted the data to maintain a consistent direction that lower is better. When the standard deviation (SD) of each group was not reported, we imputed the SD from the standard error, 95% confidence interval (CI), interquartile range, and p value; if these were not available, we imputed SDs from a similar study, per Cochrane methodology.19
We pooled all continuous outcomes using the weighted mean difference (WMD) and 95% CI, after conversion to the reference scale.20 This was to facilitate ease of clinical interpretation, so that a WMD of 1.0 would be equivalent to a 1-point difference on a 10-point scale for pain and a 1-point difference on a 4-point scale for global assessments. We set the minimal clinically important difference at 1.0 on a 10-point scale for pain, and 0.5 on a 4-point scale for global assessments.21,22 We pooled all binary outcomes using relative risks (RRs) and 95% CIs. We used a DerSimonian–Laird random effects model for all meta-analyses. We performed Grading of Recommendations Assessment, Development, and Evaluation (GRADE) quality and evidence assessments.
We used the Cochran χ2 test, I2 and the τ statistic to evaluate statistical heterogeneity. We conducted a priori subgroup analyses to evaluate the presence or absence of acetaminophen cointervention, type of NSAIDs (selective versus nonselective), surgery type and risk of bias. We predicted that acetaminophen would benefit both NSAID and codeine interventions, and we predicted that nonselective NSAIDs would be more effective than selective NSAIDs. If there were at least 10 studies available for meta-analysis, we assessed publication bias using funnel plots and the Egger test.23 We performed statistical analyses using Stata statistical software version ( Version 15.1). All comparisons were 2-tailed using a threshold p ≤ 0.05.
Results
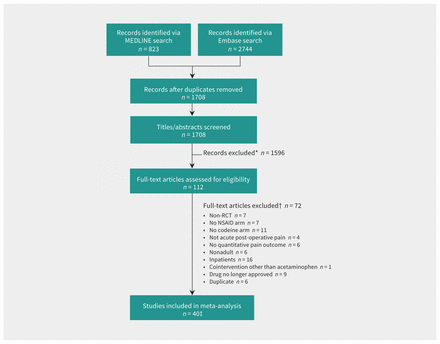
The results of our search strategy are summarized in Figure 1. We found a total of 1708 articles, and did not encounter any instances of double-counting. Screening, review and consensus ultimately resulted in 40 RCTs, 102 treatment arms (40 codeine treatment arms and 62 NSAID treatment arms), and 5116 patients (1872 patients prescribed codeine, and 3243 patients prescribed NSAIDs) being included for meta-analysis (Table 1 and Appendix 1, eTables 3 and 4). Various types and doses of NSAIDs were used. Codeine doses ranged from 15 mg to 90 mg, consistent with the most common outpatient formulations. The quality of studies included in the meta-analysis was high, with generally low risk of bias (Appendix 1, eFigures 1 and 2) and no evidence of publication bias (Appendix 1, eFigures 3, 4 and 5). The overall findings are summarized in the GRADE evidence profiles (Table 2 and Table 3).
Flow chart for study selection. Note: NSAID = nonsteroidal anti-inflammatory drug, RCT = randomized controlled trial. *Reasons for exclusion: non-RCT, no NSAID arm, no codeine arm, not acute postoperative pain, no quantitative pain outcome measure, nonadult study, inpatient use, cointervention with analgesic other than acetaminophen, drug no longer approved for use in humans and multiple combinations thereof. †See Appendix 1 for full table of exclusions. The same inclusion/exclusion criteria were applied to both stages of review. Full-text review was used when titles and abstracts were ambiguous. An article could be excluded for more than one reason. ‡Cohen κ = 0.80 (95% confidence interval 0.68 to 0.91).
Summary of included studies
GRADE evidence profile for pain and global assessment scores, codeine compared with NSAIDs
GRADE evidence profile for adverse effect outcomes, codeine compared with NSAIDs
Pain
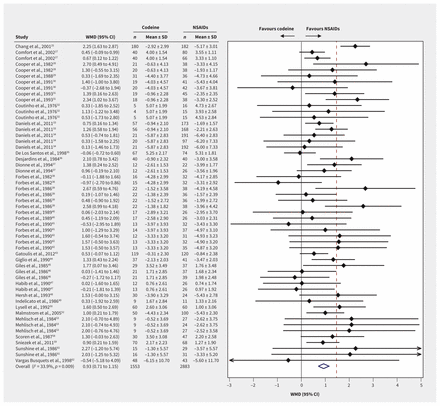
Pain at ≤ 6 hours after treatment was reported for 4436 patients from 54 trial arm comparisons (Figure 2). High-quality evidence showed that patients who received NSAIDs had lower pain scores than those who received codeine, with a WMD of 0.93 points on a 10-point scale (95% CI 0.71 to 1.15, p = 0.009, I2 = 33.9%). When comparing studies that either did not coadminister acetaminophen or used it with both NSAID and codeine groups, we found that patients using NSAIDs had even lower pain scores (WMD 1.18 points, 95% CI 0.87 to 1.48, test of interaction p = 0.05). NSAIDs had weaker superiority when acetaminophen was coadministered only with the codeine group (WMD 0.73 points, 95% CI 0.43 to 1.03). We did not detect any other subgroup effects (Appendix 1, eTable 5).
Forest plots of the weighted mean differences (WMD) and 95% confidence intervals (CIs) of pain scores at ≤ 6 hours among postoperative patients who were prescribed codeine or nonsteroidal anti-inflammatory drugs (NSAIDs). Note: SD = standard deviation.
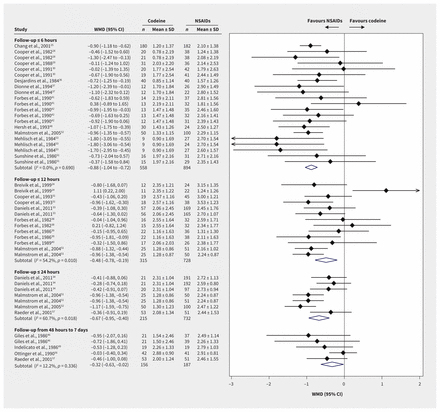
Pain at ≤ 12 hours after treatment was reported for 1660 patients from 19 trial arm comparisons (Figure 3). High-quality evidence showed that patients who received NSAIDs had lower pain scores than those who received codeine, with a WMD 0.79 points on a 10-point scale (95% CI 0.38 to 1.19, p < 0.001, I2 = 62.7%). We did not find any subgroup effects. We found smaller differences between treatments at longer outcome horizons, with no subgroup effects.
Forest plots of the weighted mean differences (WMD) and 95% confidence intervals (CIs) of pain scores at ≤ 12 hours among postoperative patients who were prescribed codeine or nonsteroidal anti-inflammatory drugs (NSAIDs). Note: SD = standard deviation.
Secondary outcomes
Global assessments showed statistically significant superiority of NSAIDs over codeine at all time measurements (Figure 4). Global assessment scores at ≤ 6 hours were available for 1452 patients and 21 trial arm comparisons. The WMD on a 4-point scale was −0.88 points at ≤ 6 hours (95% CI −1.04 to −0.72), −0.48 points at ≤ 12 hours (95% CI −0.78 to −0.19) and −0.67 points at ≤ 24 hours (95% CI −0.95 to −0.40). The minimal clinically important difference threshold of 0.5 was surpassed at 6 hours and 24 hours, according to high-quality evidence, indicating clinical importance. Between 2 and 7 days, the WMD was −0.32 points (95% CI −0.63 to −0.02), based on the smaller number of studies that reported this time horizon. Subgroup testing showed no interactions (Appendix 1, eTable 6).
Forest plots of the weighted mean differences (WMD) and 95% confidence intervals (CIs) of global assessment scores by time horizon among postoperative patients who were prescribed codeine or nonsteroidal anti-inflammatory drugs (NSAIDs). Note: SD = standard deviation.
Patients who received NSAIDs reported significantly fewer total adverse effects than those who received codeine. Moreover, fewer patients in the NSAID group reported nausea (10.4% v. 20.6%, WMD 10.2%, 95% CI 2.3% to 23.0%), vomiting (5.3% v. 18.8%, WMD 13.0%, 95% CI 2.7% to 36.6%), dizziness (3.4% v. 8.4%, WMD 5.0%, 95% CI 1.5% to 11.2%), drowsiness (5.6% v. 8.6%, WMD 3.0%, 95% CI −0.3% to 8.4%), and headache (4.5% v. 8.0%, WMD 3.5%, 95% CI 1.5% to 6.2%). Fewer patients in the NSAID groups reported any adverse effect than in the codeine group (28.9% v. 42.4%, WMD 13.6%, 95% CI 8.1% to 19.6%). Eight trials (895 patients) specifically reported bleeding or hematoma as a separate outcome measure. These bleeding events were less frequent in the NSAID arms, but no statistically significant difference was observed in the event rate between the 2 treatments (0.9% v. 1.5%, WMD 0.6%, 95% CI −0.4% to 4.0%).
Interpretation
We found high-quality evidence that outpatient postoperative adults taking NSAIDs reported less pain at 6 and 12 hours than those taking codeine in a meta-analysis of RCTs. The mean effect size for this superiority was below the minimal clinically important difference threshold of 1.0; however, the 95% CI included the threshold and did not include zero. This showed that many patients experience a clinically important benefit with NSAIDs over codeine. Furthermore, the risk of an inferior clinical effect from NSAIDs was statistically negligible.64,65
We also observed that when NSAIDs and codeine were coadministered with equivalent doses of acetaminophen, NSAID superiority was above the threshold for a minimal clinically important difference. This shows that, with or without acetaminophen coadministration, NSAIDs delivered a clinically superior analgesic effect over codeine. We observed comparative NSAID analgesic efficacy with various NSAID types, selective and nonselective NSAIDs, with various surgical procedures and at various time horizons between 6 hours and 7 days. Although a variety of pain scores were used by investigators, these were converted easily to a 10-point scale, allowing reference calculations and ease of clinical interpretation. We had suspected that the pain scores and results might be influenced by the presence or absence of acetaminophen coadministration, type of NSAID, type of surgery and risk of bias. However, we found no evidence of any statistically significant interaction effects contradicting our main results.
We evaluated patient global assessments and found moderate-to high-quality GRADE evidence that NSAIDs were statistically and clinically superior to codeine at all time points. The magnitude of difference on a 4-point scale was about 1 point at 6 hours, 0.5 points at 12 hours and 0.7 points at 24 hours. Global assessments of pain intervention can be interpreted clinically as a composite patient-reported outcome that incorporates patients’ experiences of analgesia efficacy, tolerability and adverse effects. We also found moderate-to high-quality GRADE evidence of fewer adverse effects from NSAIDs than from codeine, with significantly lower rates of any adverse effects, and of the most commonly reported adverse effects (i.e., nausea, vomiting, dizziness, headache). One common hesitation with the use of NSAIDs in a postoperative setting is the potential increased risk of bleeding, but we found moderate-quality evidence to the contrary. We found more bleeding or hematoma events with codeine treatment, although the event rates between the 2 treatments were not statistically different.
Codeine remains the most commonly prescribed opioid in Canada, despite its many shortcomings.6–9,66 Codeine is a prodrug that requires metabolism to morphine by the CYP2D6 enzyme for analgesic effect. Overall, about 10% of ingested codeine is metabolized to morphine; however, there is substantial individual-level variability in CYP2D6 enzyme expression, ranging from nonmetabolizing people without any morphine conversion to ultra-rapid metabolizers with extremely high morphine conversion.67–69 Consequently, routine codeine dosages can result in a spectrum of effects ranging from no analgesia to life-threatening levels of circulating morphine. These unique pharmacogenetic features have raised a number of safety concerns, particularly with respiratory depression.69,70 This is in addition to codeine’s many common adverse effects, including nausea, vomiting, constipation, urinary retention and sedation, all of which reduce compliance and increase rescue medication usage.71 Our findings are consistent with codeine’s known disadvantages. We suspect that the anti-inflammatory mechanism of action of NSAIDs are better suited to the acute pain of postoperative patients.16
These findings are of general importance to any clinician performing painful medical procedures. The various trials in our meta-analysis evaluated a range of procedures, different NSAID types and various degrees of acetaminophen coadministration. The low-to-moderate heterogeneity, combined with the consistent statistically significant findings, allows for generalizable results with broad clinical application. In all surgery types, subgroups and outcome time points, NSAIDs were equal or superior to codeine for postoperative pain, with higher global assessments and fewer adverse effects.
Limitations
We found low-to-moderate heterogeneity in our analysis because of the variety of interventions and dosages. However, NSAIDs showed consistent equivalence or superiority, but there may be some dosages of codeine or NSAID for which our findings do not apply. The overall results may not generalize to all types of patients. Many of the trials analyzed came from the dental literature; however, our findings remained consistent when excluding dental studies from analysis (data not shown).
Conclusion
In our meta-analysis of RCTs, we found that patients randomized to NSAIDs following outpatient surgical procedures reported better pain scores, better global assessment scores, fewer adverse effects and no difference in bleeding events, compared with those receiving codeine. These findings strengthen existing evidence and are broadly generalizable to patients across surgical disciplines. Further studies should assess the comparative effectiveness of other nonopioid analgesics, and test these findings in other populations and settings.
Acknowledgements
The authors thank Toni Tidy and Christian Sirko (Department of Anesthesia, McMaster University), and Natalie Wainwright (Department of Anesthesiology and Pain Medicine, University of Toronto), for their assistance with data checking and organization.
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
Contributors: All of the authors contributed to the conception and design of the work, and the acquisition, analysis, and interpretation of data. All of the authors drafted the manuscript, revised it critically for important intellectual content, gave final approval of the version to be published and agreed to be accountable for all aspects of the work.
Data sharing: All data are presented in the article and appendices. No additional data are available.
- Accepted March 10, 2021.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/