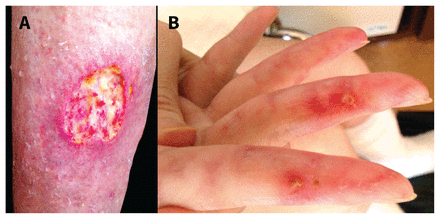
A 43-year-old woman presented to our rheumatology clinic with a 2-month history of progressive, painful ulcerations after the appearance of purpura on the extensor surfaces of her lower legs (Figure 1A). She also had ulcerations and chilbains on her fingers (Figure 1B) and in her mouth. She had a fever, malar rash, alopecia and polyarthritis without nodular lesions or livedo reticularis. Ten years before presentation, she received a diagnosis of systemic lupus erythematosus (SLE) after presenting with polyarthritis. At that time, she had pancytopenia and hypocomplementemia, and tested positive for antibodies against double-stranded DNA. She was successfully treated with prednisone and had stabilized on a maintenance dose. However, 2 years before presentation she had stopped steroid treatment.
(A) A cutaneous ulceration on the extensor surface of the right lower leg of a 43-year-old woman with systemic lupus erythematosus. (B) Ulcerations and chilblain lupus on the patient’s fingers.
Laboratory findings showed lymphopenia, hypocomplementemia and antibodies against double-stranded DNA and cardiolipin, but the result of her lupus anticoagulant test was negative. Skin biopsy showed lymphocyte infiltration into the blood vessel wall, leukocytoclastic vasculitis with fibrinoid necrosis and panniculitis with calcium deposition. There was no evidence of thrombosis, pyoderma gangrenosum, infection, diabetic ulcer or neoplasm. Culture from the lesion was negative. Based on symptoms and pathology, we diagnosed cutaneous ulceration caused by lupus vasculitis. After treatment with prednisone 30 mg, followed by starting hydroxychloroquine 200 mg and belimumab 200 mg/week, the patient’s ulcerations resolved over 6 months.
Although cutaneous involvement, such as malar and discoid rashes, is common in patients with SLE, ulceration is uncommon. 1 In a retrospective study of 670 patients with SLE, 76 (11%) patients developed vasculitis; of these, only 11 had ulcers or ischemic lesions.2 Typical histological findings include leukocytoclastic vasculitis with fibrinoid necrosis of the vessel wall and polymorphonuclear cell infiltration.1 Belimumab and hydroxy-chloroquine are recommended therapies for the cutaneous manifestations of SLE3 and are effective therapies for refractory cutaneous lupus erythematosus.
Acknowledgement
The authors thank Editage (www.editage.com) for English language editing.
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
The authors have obtained patient consent.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/