A 34-year-old otherwise healthy Vietnamese man, living in Canada for four years, attended the emergency department with a three-week history of abdominal pain and fever. He had a leukocyte count of 14.64 (normal 4.0–10.0) × 109/L, alanine transaminase level of 65 (normal 8–60) U/L and serum glucose level of 6.1 (normal 3.2–9.0) mmol/L. Abdominal ultrasonography and subsequent computed tomography showed two hypodense lesions in the right lobe of the liver (Appendices 1 and 2, available at www.cmaj.ca/lookup/suppl/doi:10.1503/cmaj.171344/-/DC1).
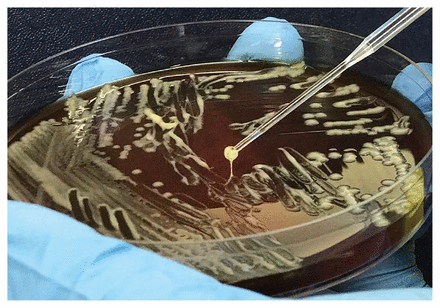
Percutaneous drainage of the lesions showed pus, with gram-negative bacilli in both the aspirate and blood cultures. The bacterial colonies were visibly mucoid and later identified as Klebsiella pneumoniae, susceptible to ceftriaxone and ciprofloxacin. The string test, which is a quick screening method providing phenotypic evidence of hypermucoviscous strains of K. pneumoniae, showed strings measuring greater than 5 mm in length (Figure 1).1 Genetic testing later confirmed the presence of magA and rmpA genes, which encode virulence factors responsible for the K1 capsular polysaccharide serotype and mucoid phenotype, respectively.1,2 After partial drainage of the abscesses and one week of treatment with ceftriaxone, the patient was discharged home. He received 11 weeks of oral ciprofloxacin until clinical and radiographic resolution of the abscesses was shown.
Positive string test on a hypervirulent strain of Klebsiella pneumoniae from a liver abscess in a 34-year-old man with fever and abdominal pain, shown by a bacteriology inoculation loop generating a viscous string longer than 5 mm by stretching bacterial colonies on an agar plate.
Pyogenic liver abscesses are typically polymicrobial and due to underlying biliary tract pathology; albeit 20%–40% of cases are considered cryptogenic.2 Hypervirulent (hypermucoviscous) phenotypes of K. pneumoniae are an emerging cause of pyogenic liver abscess and can be associated with impaired glucose tolerance.3 Although initially described in the mid-1980s in Taiwan, these hypervirulent strains of K. pneumoniae are increasingly recognized as a monomicrobial cause of cryptogenic liver abscess in Western countries.1,2 Metastatic foci such as endophthalmitis and meningitis occur in about 10%–16% of cases.1,2 Although our patient’s K. pneumoniae isolate was susceptible to most β-lactam antibiotics, carbapenem-resistant strains of K. pneumoniae showing a hypermucoviscous phenotype have been recently reported and are a cause for global concern in an era of antimicrobial resistance.3
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
The authors have obtained patient consent.