Lessons learned
Territorialism, delay and poor communication plagued Canada’s response to the listeriosis outbreak that killed 22 people in 2008, says Ontario Chief Medical Officer of Health Dr. David Williams.
The Canadian Food Inspection Agency waited nearly a month to inform health officials that contaminated ready-to-eat meats were being distributed to grocery stories — a dangerous delay in issuing a product recall, Williams stated in his Report on the Management of the 2008 Listeriosis Outbreak in Ontario (www.health.gov.on.ca/english/public/pub/disease/listeria/listeriosis_outbreak_rep.pdf).
Williams’ report, along with separate “Lessons Learned” reports simultaneously released by the Canadian Food Inspection Agency, The Public Health Inspection Agency of Canada, and Health Canada combine to create an impression that oversight of food safety in Canada was largely haphazard at the time of the outbreak.
The agencies and department state in their postmortems, though, that they have introduced new policies and procedures to redress the deficiencies (www.inspection.gc.ca/; www.phac-aspc.gc.ca; and www.hc-sc.gc.ca/fn-an/pubs/securit/eclosion_listeriosis_outbreak-eng.php).
Not everyone, though, is convinced that the agencies have fixed their flaws.
“The recurring theme appears to be problems with communication, roles and responsibilities and information transfer — those were problems identified during the severe acute respiratory syndrome and Walkerton, Ontario, [contaminated water] outbreaks in repeated reports over the years,” says Dr. Kumanan Wilson, a scientist at the Ottawa Health Research Institute and Canada Research Chair in public health policy.
A reciprocal information transfer agreement between the federal and provincial governments and the increased independence of Canada’s public health agency could help manage future outbreaks, Wilson adds.
Others suggest centralization of authority is required, in the form of a new food safety agency.
“Basically, what Canada needs is a more cohesive, systemic approach to managing food safety crises,” says Sylvain Charlebois, an associate professor at the University of Regina’s faculty of business administration.
“Right now, we don’t have a system in place that would allow us to recognize correlations between incidents occurring in Saskatchewan and incidents occurring in Ontario,” Charlebois says.
Still to come is a report by Sheila Weatherill, former president of the Edmonton Health Authority in Edmonton, Alberta, who was appointed by Prime Minister Stephen Harper to investigate means of avoiding future outbreaks of food-borne disease (CMAJ 2009;180 [5]:503).
Weatherill’s report is expected July 20. — Krista Seggewiss, Ottawa, Ont.
CPR in clinics
Province of Quebec Coroner Catherine Rudel-Tessier has urged the Collège des médecins du Québec to revise its regulations for private health care clinics to ensure that all physicians and nurses working in such facilities are trained in cardiopulmonary resuscitation and that such facilities are equipped with defibrillators.
Rudel-Tessier’s recommendations emerged from a review of the death of Jean-Jacques Sauvageau from a pulmonary embolism suffered in the waiting room of the Clinique Médicale Viau in St. Léonard, Quebec, on Jan. 11, 2008. Witnesses testified Sauvageau arrived at the clinic in severe respiratory distress and was dispatched to the waiting room, where he eventually slumped over and his dentures fell to the floor.
The doctor on duty, Dr. Jacques Chaoulli, took Sauvageau’s pulse but made no effort to resuscitate him. Chaoulli left the waiting room and instructed his nurse to call 911 to have the body removed.
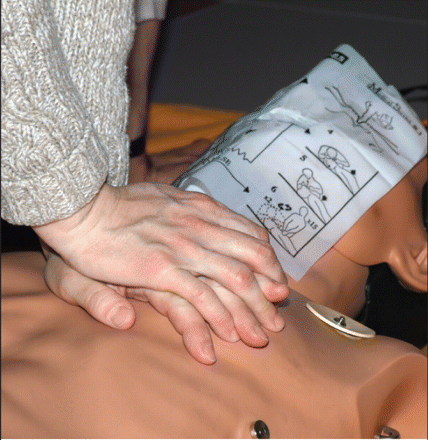
Quebec’s coroner would like health care clinic staff to be trained in cardiopulmonary resuscitation, here being performed on a dummy. Image courtesy of Photos.com
Audio tapes of 911 calls presented at the hearing indicated that an Urgences Santé official urged both Chaoulli and a nurse to do heart compressions. But they responded that “it’s useless, he’s dead,” Rudel-Tessier told a press conference. Another patient in the waiting room called 911 for resuscitation instructions and expressed distress that “the doctors were doing nothing.”
Chaoulli later took issue with Rudel-Tessier’s findings, stating that the incident points to the need for all walk-in clinics to have dedicated triage nurses. Chaoulli is the physician who successfully challenged Quebec’s ban on private health insurance for medically necessary services. The Supreme Court of Canada ruled that the ban violated provincial human rights law (Chaoulli and Zeliotis v. A.G. Quebec et al.). — Wayne Kondro, CMAJ