Molecular epidemiology of tuberculosis
Tuberculosis is a leading cause of death and illness in the world. Advances in molecular epidemiology have improved our understanding of how Mycobacterium tuberculosis is spread. In this issue, 2 groups of investigators describe how they used DNA fingerprinting to determine whether patients with newly diagnosed tuberculosis had isolates belonging to genetically similar clusters of recent infection or had unique isolates representing reactivated disease. They gathered epidemiologic data to delineate groups at risk of new infection. In Vancouver, Eduardo Hernández-Garduño and colleagues found that Canadian-born Aboriginals and patients with a history of injection drug use are at high risk, and in Montreal, Sophie Kulaga and coworkers identified Haitian immigrants as particularly vulnerable.
Figure. Photo by: Science Photo Library
In a related commentary, Megan Murray discusses the dynamics of transmission among foreign-born people. She reminds the medical community that new Canadians should be a target of infection control strategies.
Diagnosing dysmorphic signs in children
Humans grow in different ways. Dysmorphology is a branch of clinical genetics dedicated to interpreting atypical patterns of growth and structural defects. An accurate diagnosis allows the families of children with dysmorphic signs access to accumulated knowledge about the relevant condition. Alasdair Hunter uses case examples to illustrate that the diagnostic approach to dysmorphism is not much different from that of other medical disciplines and discusses how cytogenetic and molecular techniques continue to improve our ability to make precise syndrome diagnoses. In a related article, Alison Sinclair describes how the development of fluorescence in-situ hybridization (FISH) has greatly increased the sensitivity and specificity of traditional methods of karyotyping and has moved from the laboratory to routine use.
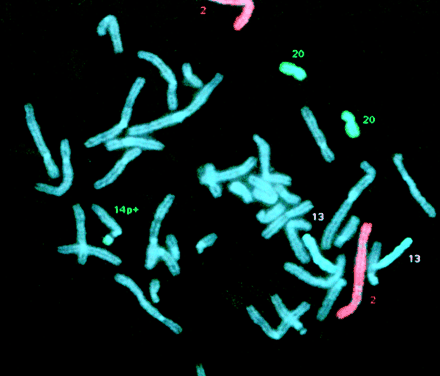
Figure.
Survival following in-hospital CPR
Cardiopulmonary resuscitation (CPR) was first described in the 1960s and is now an integral part of resuscitation after cardiac or respiratory arrest. In TV medical dramas, 75; of patients survive following CPR, but in reality the results are different. Peter Brindley and colleagues, using 2 years of records from Edmonton teaching hospitals, provide survival data and outcome details for 247 hospitalized patients who experienced witnessed and unwitnessed cardio-pulmonary arrests. Among witnessed arrests, 1 in 2 patients were resuscitated, 1 in 3 survived 24 hours, 1 in 4 survived to discharge and 1 in 5 returned home. Of 104 unwitnessed arrests, only 1 patient survived to discharge. This knowledge is important for physicians, patients and families who are engaged in discussions about end-of-life care in the hospital setting.
See page 343
Hormone replacement therapy
In early July, one of the arms of a large study of women's health was stopped prematurely. To the surprise of women and their physicians around the world, it was clear that hormone replacement therapy (HRT) with estrogen and progestin was causing significant harm. HRT has been prescribed to women for years to preserve health and prevent disease, most notably to decrease the risk of coronary artery disease and osteoporosis, and was the second most commonly prescribed medicine in the United States in 2000. Salim Yusuf and Sonia Anand describe the importance of this large, well-designed and carefully conducted study and comment on the implications for the future health of women. In a related commentary, Anna Day highlights the importance of randomized controlled trials in preventive medicine, with particular attention to women's health. In another commentary, David Sackett weighs heavily into the often “traditional” assumptions that underlie preventive medicine.

Figure. Photo by: Health Canada

