Abstract
Background: Preterm labour occurs in about 10% of all pregnancies and is the most important cause of premature birth. Women with preterm labour are admitted to hospital to have the contractions stopped. Thereafter, many women remain in hospital until delivery. We conducted a randomized clinical trial to compare hospital care with home care of women who had been admitted to hospital for preterm labour.
Methods: After they had received treatment for an acute episode of premature labour, women at 2 regional perinatal centres associated with teaching hospitals were randomly assigned to home care or hospital care. Eligible women (n = 250) were aged 18 years or older, lived within 50 km of the hospital, had a gestational age between 20 and 35 weeks, had no prior preterm delivery and were experiencing their first episode of preterm labour and first admission to hospital for preterm labour. Analysis was by intention to treat.
Results: There were no significant differences between the 2 groups in mean gestational age at delivery (home: 37.52 weeks, hospital: 37.50 weeks) or in mean birth weight (home: 2974 g, hospital: 3020 g). There were no significant differences between the 2 groups with respect to the proportions of babies born before term or the mean duration of neonatal hospital stay, neonatal intensive care unit stay and intermediate care nursery stay. The mean duration of the first stay in hospital for the women in the home group (3.8 days) was significantly shorter than the mean duration for women in the hospital group (6.1 days). In addition, the mean duration of all maternal stays in hospital was significantly shorter for the women in the home group (3.7 days) than in the hospital group (5.0 days).
Interpretation: Home care management is an efficient and acceptable alternative to hospital care for women experiencing preterm labour.
Preterm labour, which is defined as the presence of persistent increased uterine activity (3 or more contractions per hour) associated with progressive cervical changes before 37 weeks' gestation,1,2,3 complicates between 8% and 10% of all pregnancies.4,5,6,7 It represents the single most frequent cause of premature births.2,8,9 The goal of preterm labour management is to diagnose the condition promptly, treat it adequately and prevent its recurrence.10,11 Management usually includes varying combinations of parenteral hydration, monitoring of uterine activity, evaluation of cervical change, administration of tocolytics and in-hospital bedrest.2,10,12 Criteria used to judge the successful inhibition of premature labour include the arrest of uterine contractions, term delivery at or after 37 weeks' gestation and birth weight of 2500 g or more. Some women remain in hospital until delivery, whereas others are discharged home with medication and instructions to restrict their physical activity. In-hospital management has not been shown to improve perinatal outcomes in the treatment of women with a high-risk singleton pregnancy,11,13 although there are many proponents of this treatment for women with preterm labour.14,15,16 Given the rise in health care costs, physicians have been forced to modify medical management by sending women home earlier, often without special follow-up programs. There is a dearth of information on the impact and the safety of early hospital discharge programs for women experiencing preterm labour.
Spending time in hospital appears to have detrimental psychological effects on expectant women,17,18,19,20 and their families.21 Published reports on alternative approaches to the management of preterm labour focus mostly on the efficacy of ambulatory monitoring of uterine activity, program implementation and home monitoring of uterine activity with or without visits from nurses.8,16,22,23,244 Dahlberg25 and Harmon and Barry26 have described prenatal home care programs that included home visits by nurses, assessment, teaching, supervision, telephone accessibility and medical referral. The objective of such programs is to provide support and care in the more familiar and less costly home environment. Although preliminary observations25,26 suggest that this approach does have potential, further assessment in the form of clinical trials is required.
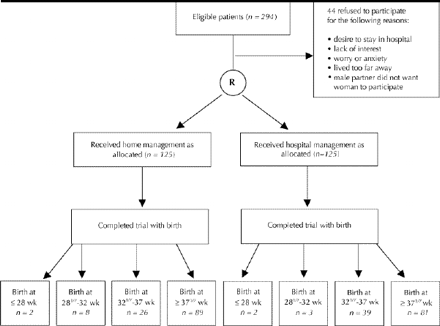
The goal of this randomized clinical trial (RCT) was to compare the neonatal and maternal outcomes of home care versus hospital care for women with preterm labour (Fig. 1). The primary neonatal outcomes were gestational age and birth weight. The secondary neonatal outcomes were the rate of preterm birth, the duration of neonatal hospital stay and the number of admissions to the neonatal intensive care unit (NICU). The maternal outcomes were the number of maternal admissions to hospital and length of stay.
Fig. 1: Profile of randomized clinical trial for women experiencing preterm labour. R = randomization.
Methods
The pregnant women who were invited to participate in this RCT had a singleton pregnancy of between 20 and 35 weeks' gestation, with a diagnosis of preterm labour, and had been admitted to one of 2 regional perinatal centres, one in Montreal and the other in Quebec City. Preterm labour was diagnosed using the following 3 criteria: persistent uterine contractions for more than one hour that were not responsive to bedrest and hydration, documented cervical changes and intact fetal membranes. Women were approached by the research assistant within 48 hours of admission to hospital if they met the following eligibility criteria: first episode of preterm labour and first admission to hospital for preterm labour, no history of preterm delivery, gestational age between 20 and 35 weeks, maternal age of 18 years or more, and residence within 50 km of the hospital. Women were excluded from the study if there was more than one complication of pregnancy at the time of randomization, cervical dilatation that was greater than 4 cm and effacement that was greater than 80%, a diagnosis of intrauterine death or a diagnosis or suspicion of fetal malformation. Women were approached with information about the study after their contractions had resolved spontaneously or in response to tocolytic treatment.
Women who agreed to take part in the study were randomly assigned to either home care with visits from nurses (experimental group) or traditional hospital care (control group). Block randomization was carried out using sealed opaque envelopes, with block sizes randomly varying between 2 and 6 subjects. Sociodemographic and perinatal information was obtained for the women who had agreed to participate in the study. Data from the women who refused to participate were not collected because the hospital ethics committees prohibited access to their charts.
Prior to randomization, treatment for preterm labour included bedrest, hydration, intravenous and oral tocolytic therapy, and betamethasone in various combinations according to the judgement of the treating obstetrician. After the cessation of uterine contractions, the women were transferred to the perinatal unit at which point they were randomized. After randomization, women assigned to the experimental group were discharged from the hospital, whereas those in the control group remained in the hospital until their obstetrician discharged them home.
Experimental group (early discharge and home care)
The care plan and the frequency of visits were determined on an individual basis. Home visits were conducted by registered nurses working in the perinatal unit. The attending obstetrician completed the medical prescription, and external uterine and fetal heart rate monitoring were carried out in the home by the nurses; monitor strips were reviewed by the nurses and were sent daily to the perinatologist for interpretation. If any concerns arose regarding fetal status, the nurse took the strip immediately to the perinatologist for interpretation and discussion of appropriate management. During the visit, the nurse obtained blood and urine samples, which were taken to the laboratories. One-on-one teaching and psychosocial support were considered to be priorities. The goal was to maximize each pregnant woman's ability to participate in her care and to react quickly if a problem should arise. The nurse who provided teaching based on each woman's needs completed a teaching checklist. Each woman had a self-monitoring diary to record uterine activity, fetal movements, maternal activity, medication and her thoughts or comments. She was instructed to contact her physician or to report to the hospital for evaluation if she became aware of any sign or symptoms associated with early labour, or if she experienced 4 or more contractions per hour that persisted for more than one hour despite oral hydration and bedrest.
Nursing visits were provided from 9 am to 5 pm. When possible, the visits were scheduled on the same day of each week, preferably on weekdays. The nurse could be contacted by telephone to answer any questions or address concerns between visits. An answering machine was available 24 hours a day to tape messages from the pregnant women. Women who experienced a change in their condition or who had any concerns regarding their health status during nonoperational hours were advised to notify their attending physician or, if necessary, to go to the emergency department, or to call the provincial emergency telephone number of 911. Although the average home visit lasted approximately one hour, it was adjusted according to each woman's needs. Any concerns that arose during the visit were immediately reported to the attending physician by telephone. The nurses assessed additional needs such as a homemaker or child care and, when required, such services were arranged through family and community resources. The home care nurse documented each visit on each woman's chart. The home care chart included information from any previous admissions to hospital. After each visit, one copy of the report was sent to the attending physician.
Control group (hospital care)
Women assigned to the control group received the usual in-hospital medical and nursing care according to their medical status. The usual procedures for hospital discharge were followed. Women were not expected to remain in hospital for any longer than would have normally been the case. The nurses in the perinatal unit provided the same teaching as that received by the experimental group using the same teaching checklist. Women had a self-monitoring diary to record uterine activity, fetal movements, maternal activity, medication and their thoughts or comments. External uterine and fetal heart rate monitoring were carried out as prescribed. Women who had been discharged from the hospital were encouraged to call regarding their symptoms and concerns on an emergency basis at any time or, if necessary, to go to the emergency department or the obstetric ward.
A measure of term delivery
The ultimate goal of prenatal care is to prolong pregnancy to term. We created a measure that allowed us to quantify (as a percentage) the extent to which women were able to reach their goal of a term delivery. Term delivery was defined as 38 weeks' and also as 40 weeks' gestation. The formulae for these calculations are as follows:
% of term delivery at 38 weeks = 100 × (GADel - GARan)/(266 days - GARan), where GADel is gestational age at delivery and GARan is gestational age at randomization.
Similarly, % of term delivery at 40 weeks = 100 × (GADel - GARan)/(280 days - GARan).
For example, if a woman had been randomized at 200 days of pregnancy and delivered at 240 days, the extent to which her pregnancy approached delivery at 40 weeks would be 50% (namely, [240-200]/[280-200] = 40/80).
Statistical analyses
A sample of 132 women per group was required based on the assumptions of a 2-tailed α of 5%, a 10% probability of a type II error (β), a 1-week difference between the means and a standard deviation of 2.5 weeks for gestational age. Of the 294 women who were eligible to participate in the RCT, the final sample of 250 women produced a power of 89% to detect a difference in the means for gestational age of more than one week.2
The analysis was by intention to treat. Student's t-test was used to compare means, with adjustment for inequality of variances when necessary. The 𝛘2 and the Fisher exact test were used to compare proportions. One-way ANOVA and Pearson's 𝛘2 tests were used to examine differences between the 2 groups in neonatal and maternal outcomes. The critical α was set at p < 0.05.
Results
Both groups of women who participated in the study were comparable with respect to the following baseline sociodemographic characteristics: maternal age, education, marital status, family income and employment during pregnancy (Table 1). In each group, the majority were working full-time (home: 73.9%, hospital: 75%) and working a day shift (home: 69.6%, hospital: 73.4%). Most of the women were born in Quebec (home: 81.5%, hospital: 84.1%). They were also comparable regarding the following baseline obstetric characteristics: gestational age at randomization, effacement and dilatation at randomization (data not shown), gravidity, parity, abortions (data not shown), number of live children (data not shown), proportion receiving tocolytic and betamethasone medications, method of labour onset, duration of labour and method of delivery (Table 1). Regarding gestational age at baseline, the frequency distributions were quite similar: 20–24 weeks (home: 6.4%, hospital: 3.2%), 25–29 weeks (home: 40.8%, hospital: 40.8%) and 30–34 weeks (home: 52.8%, hospital: 56%). There was no significant difference between the groups for gestational age at baseline (p = 0.12).
Table 1.
Primary and secondary neonatal outcomes
There were no significant differences between the groups in gestational age at delivery (p =0.96) or birth weight (p = 0.60) (Table 2). A similar proportion of babies were born at 37 completed weeks in both groups (relative risk [RR] 0.96, 95% confidence interval [CI] 0.73–1.28; p = 0.80). When the birth weights were assessed by category (< 1500 g, 1501–2000 g, 2001–2500 g, 2501–3000 g, > 3000 g) or dichotomized (≤1500 g or >> 1500 g; RR 1.968, 95% CI 0.52–7.50), statistical analyses revealed no significant differences between the 2 groups. Approximately the same number of babies from the home group were admitted to the NICU compared with those from the hospital group (p = 0.70) as well as to the intermediate care nursery (p = 0.80). A similar number of babies in both groups had either multiple health problems (a combination of respiratory, cardiac, hematological, neurological problems) or other health problems. In addition, there were 7 babies in the home group who had an Apgar score of less than 8 at 5 minutes compared with one baby from the hospital group (p = 0.05). The mean length of stay in the NICU for the babies in the home group was similar to that of babies in the hospital group (p = 0.98). However, with regard to the mean length of stay within the intermediate care nursery, the babies in the home group stayed an average of 18.8 days whereas those in the hospital group stayed 12.1 days. This disparity was not statistically significant (p = 0.09).
Table 2.
Maternal outcomes
The mean durations of antenatal time spent in hospital before randomization for women in both groups were similar (1.5 and 1.52 days respectively, p = 0.87). The mean duration of the first maternal stay in hospital for the home group (3.8 days) was significantly lower than the mean for the hospital group (6.1 days, p = 0.0001) (Table 3). The majority of the women (99.2%) in the home group stayed 10 days or less for the first stay in hospital compared with 91.9% of the women in the hospital group. In addition, the mean duration of all stays in hospital for the women in the home group (3.7 days) was significantly lower (p = 0.03) than the mean for the women in the hospital group (5.0 days). None of the differences between the 2 groups for the total duration of maternal readmissions to hospital and the duration of each readmission were significant (data not shown).
Table 3.
A measure of term delivery
When the 38-week term delivery end point was applied (Table 4), 69 of 125 women in the home group and 64 of 125 in the hospital group were able to surpass this end point (delivery > 38 weeks). This means that more than half of the women in each group were able to continue their pregnancy beyond the minimal limit for term delivery. If 40 weeks was chosen as the end point, then 44 women in the home group continued their pregnancy to within 81%–100% of this objective compared with 50 women in the hospital group. None of these differences were statistically significant.
Table 4.
Interpretation
This study has several strengths. Treatments were randomly allocated. We carefully monitored compliance with the prescribed intervention, and a satisfactory contrast in terms of differences in the number of days spent in hospital was achieved.
This RCT was originally set up to investigate differences between the 2 study arms in terms of the primary neonatal outcomes, gestational age and birth weight at delivery, instead of as an equivalence trial.5 The primary neonatal outcomes are not significantly different for the home and the hospital groups. The difference between the means for gestational age is 0.02 weeks, whereas the difference between the mean birth weights is 46 g. Our findings corroborate those of Blondel and Mellier27 who conducted a meta-analysis of 7 RCTs concerning home visits during pregnancy involving various complications. In their analysis, they found no difference between the experimental and control groups in the number of deliveries before 37 completed weeks. Furthermore, they found no significant difference in birth weight between the 2 groups when the babies weighed less than 2500 g.
There were no significant differences in the secondary neonatal outcomes: the rate of preterm birth, the number of admissions to the NICU and to intermediate care, the mean duration of neonatal hospital stay and the mean duration in both levels of care. However, there is a difference of 1.8 days between the mean durations of all neonatal stays in hospital and a difference of 0.2 days between the means for time spent in intensive care, with the babies from the experimental group spending slightly more time in the unit. There is also a difference of 6.7 days between the mean duration of time in hospital for intermediate care, with the babies from the home group spending slightly more time in this unit. These findings corroborate those of the meta-analysis by Colton and colleagues:28 there were no significant effects found overall and in any stratum with regard to infant referral to the intensive care unit.
A significant difference was found between the 2 groups in the overall total duration of maternal time spent in hospital: total times spent in hospital for the home group were significantly lower than those of the hospital group. The duration of the first stay in hospital for the women in the home group was longer than anticipated (one woman had a total duration of 20 days for the first stay in hospital). More women in the home group were not readmitted to hospital compared with those in the hospital group. Our findings are contrary to those of 2 meta-analyses conducted in France. Blondel and Bréart22 found no differences in the length of stay in hospital and in admission rates between the experimental and control groups in the pooled data. In a second meta-analysis of 7 studies, Blondel and Mellier27 found no significant differences between the experimental and control groups regarding length of stay in hospital and rate of admission to hospital. However, when the number of hospital visits is considered for medical surveillance, the intervention group visited the hospital less often than the control group.
The majority of the women in the home group were able to reach term delivery. A principal goal of obstetric care is the prevention of prematurity.16 Indeed, the ultimate goal for the treatment of preterm labour is the delivery of a healthy term neonate because it is known that neonatal outcomes are greatly improved when intrauterine life is extended. If fetal status is acceptable, prolonging pregnancy decreases the incidence of several neonatal morbidity factors such as respiratory distress, patent ductus arteriosus, prolonged intensive care and the overall number of days spent in hospital.29 Although great strides have been made in the reduction of maternal mortality and morbidity, there has been a less significant reduction in perinatal morbidity and mortality.30
Several limitations arise from this RCT. First, the reasons for keeping certain women in hospital were not necessarily related to the women's condition; in certain cases, their physicians were just reluctant to release them. Second, some physicians had to be reminded of the research protocol in which they had agreed to participate; after much discussion and encouragement from other colleagues, they did adhere to the research protocol. Continuous communication with medical staff31 is important for the success of any RCT. Third, women in the hospital group were being discharged earlier than they might have been because their physicians were aware that no major incidents had arisen with the home group: no fetal deaths had occurred and no women had been sent to the hospital for emergency readmission or delivery. Some women may have spent less time in the hospital because health care system reform in Quebec involves more ambulatory care and shortened hospital stays.
Home care should be considered as a viable alternative to hospital care for women experiencing preterm labour. We suggest that hospital-based care should be reserved for women experiencing serious conditions necessitating intense medical surveillance and nursing care. Home care programs should be affiliated with hospital services rather than community health care services, because hospital health care professionals have more skills and knowledge with which to handle emergencies. The effects of transferring the burden from professionals in hospitals to family members in the home, however, need to be examined further. We fully endorse the expression “there is no place like home” for women experiencing preterm labour.
Acknowledgments
We would like to thank the following nurses who made this study possible: Dominique Vincent, Martine Lachance, Rachel Bois and Yvette Franck Giguère. Special thanks are also extended to the research assistants: Marilyn Aita, Elaine Perreault and Andéanne Morin.
This research was funded by Health Canada through the National Health Research and Development Program (NHRDP) Project No. 6605-3881-301.
Footnotes
-
This article has been peer reviewed.
Contributors: Dr. Goulet and Ms. Gévry designed and prepared the manual for home visits by nurses. Ms. Gévry, Dr. Lemay, Dr. Gauthier, Ms. Lepage and Dr. Fraser were in charge of recruiting subjects and data collection. Ms. Polomeno interpreted the findings. Dr. Goulet and Ms. Polomeno drafted the article. Their coauthors made substantial contributions to revisions of the manuscript.
Competing interests: None declared.
Reprint requests to: Dr. Céline Goulet, Professor, Faculté des Sciences Infirmières, Université de Montréal, Case postale 6128, Succursale Centre-Ville, Montréal QC H3C 3J7; fax 514 343-2306; [email protected]
References
- 1.
- 2.
- 3.
- 4.
- 5.
- 6.
- 7.
- 8.
- 9.
- 10.
- 11.
- 12.
- 13.
- 14.
- 15.
- 16.
- 17.
- 18.
- 19.
- 20.
- 21.
- 22.
- 23.
- 24.
- 25.
- 26.
- 27.
- 28.
- 29.
- 30.
- 31.