A previously healthy 30-year-old man presented to the emergency department with a 2-week history of dyspnea, dry cough and skin lesions. The patient has sex with men. He immigrated from Thailand to the United States 5 years before. On physical examination, we heard bilateral rhonchi and found umbilicated papules on his face, chest and neck (Figure 1). Laboratory investigations showed a new diagnosis of HIV-1 infection with a viral load of 207 000 copies/mL and CD4 counts of 13 (normal 500–1200) cells/mm3, as well as positive results for serum and cerebrospinal fluid cryptococcal antigen with titres of 1:2560 and 1:10, respectively. Computed tomography of the chest showed bilateral centrilobular ground glass opacities. Mucicarmine stain of a biopsy of a papule and Grocott–Gomori methenamine-silver nitrate stain of bronchoalveolar lavage fluid showed budding yeasts consistent with cryptococcosis. We diagnosed disseminated cryptococcosis. The patient completed a 2-week course of liposomal amphotericin B and flucytosine, transitioning to oral fluconazole. Antiretroviral therapy was started after induction therapy completion with liposomal amphotericin B and flucytosine. At 6-week follow-up, dyspnea had resolved and the papules were fading.
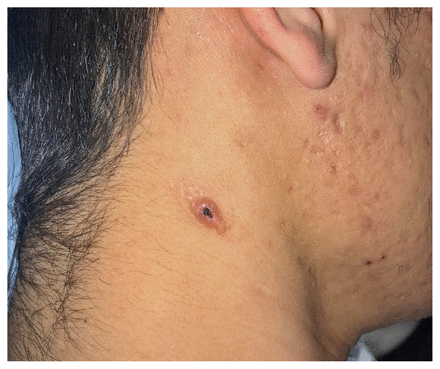
Umbilicated skin papule on the neck of a 30-year-old man with a recent diagnosis of HIV. A skin biopsy showed budding yeasts on mucicarmine stain and Grocott–Gomori methenamine-silver stain consistent with cryptococcosis.
Cutaneous lesions are seen in about 15% of patients with disseminated cryptococcosis, and the characteristic umbilicated papules mimic molluscum contagiosum.1 Differential diagnosis for patients from Thailand with HIV who present with papules should also include talaromycosis and disseminated Mycobacterium avium complex. As most cutaneous cryptococcal lesions represent disseminated infection, a lumbar puncture to evaluate for meningoencephalitis is warranted in patients with skin lesions consistent with cryptococcosis, in addition to serum cryptococcal antigen testing. Routine evaluation for central nervous system (CNS) and pulmonary involvement is important as CNS symptoms may develop indolently, with patients often having no headache or meningeal signs, as seen in this patient.
Treatment of cryptococcal meningoencephalitis requires an extended course of antifungal drugs.2 The start of antiretroviral treatment should be delayed for 2–10 weeks in patients with cryptococcal meningoencephalitis to reduce the risk of immune reconstitution inflammatory syndrome.3
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
The authors have obtained patient consent.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/