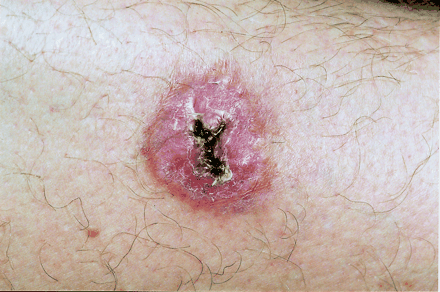
A previously healthy 54-year-old man returned from a 2-week vacation in the rain forests of Belize, where he recalled being bitten several times by mosquitoes and flies. He was well upon his return to Canada, but 6 weeks later a localized “volcano”-like eruption developed on his right shin with progressive, generalized lymphedema of his right lower extremity. His family physician prescribed a course of antibiotics for presumed cellulitis, with no improvement. Over the next 6 weeks the lesion ulcerated, and the lymphedema worsened. He was referred to our tropical medicine clinic, where he was seen to have a painful ulcer 2 х 2 cm in diameter over his right shin that had raised edges and marked central granulation tissue with serous discharge (Fig. 1).
Figure 1. Photo: Images courtesy of Dr. Shariq Haider
The differential diagnosis of such a lesion includes chronic tropical ulcers frequently caused by Vincent's organisms, Buruli ulcers caused by Mycobacterium ulcerans, cutaneous leishmaniasis and pyoderma gangrenosum.1,2 Chronic tropical ulcers typically respond to local care and systemic antibiotic therapy, and Buruli ulcers are painless and do not have raised margins. Given the clinical presentation, cutaneous leishmaniasis seemed the most likely diagnosis.
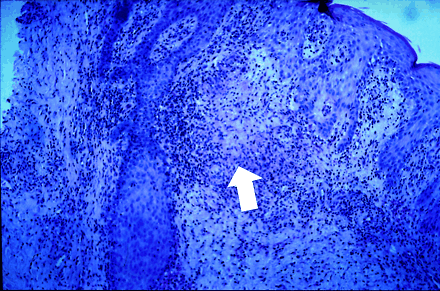
Numerous methods are available for diagnosing cutaneous leishmaniasis.3 A biopsy of the lesion showed epidermal hyperplasia and deep dermal chronic inflammation with occasional granulomas, but no amastigotes (the undifferentiated form of the Leishmania parasite found within the macrophages) (Fig. 2). Giemsa and hematoxylin–eosin staining of fluid aspirates did not yield Leishmania amastigotes; however, on day 5, culture of a biopsy specimen in M199 medium (Life Technologies Inc., Rockville, Md.) showed Leishmania promastigotes (a differentiated stage of the parasite's life cycle). A sample of the ulcer was also found to contain DNA for Leishmania braziliensis, detected using the polymerase chain reaction test and a specific primer set developed at the National Reference Centre for Parasitology, Montreal.4 Because L. braziliensis is associated with mucocutaneous leishmaniasis, our patient was given sodium stibogluconate (antimony compound) intravenously at a dose of 20 mg/kg daily for 20 days, with healing of the ulcer (Fig. 3) and resolution of the lymphedema.
Figure 3. Photo: Images courtesy of Dr. Shariq Haider
Figure 2. Photo: Images courtesy of Dr. Shariq Haider
Leishmaniasis is a heterogenous parasitic disease transmitted to humans by the bite of a sandfly. The disease is endemic in 88 countries, involving regions of Africa, Asia, the Mediterranean, and South and Central America.5 It can involve the skin but also the viscera, especially of the liver and spleen. Of particular concern is the increased number of often fatal cases of visceral leishmanisis seen mainly in southern Europe as a coinfection with HIV acquired principally through intravenous drug use.5 Most cases of cutaneous leishmaniasis are self-limited over periods of weeks; however, certain subtypes of Leishmania sp. can cause mucocutaneous disease, with destructive lesions of the oral and nasal cavities that require treatment.6 Treatment options include allopurinol, oral therapy with antifungal azole agents, topical treatments (heating, freezing, intralesional antimony compounds, paramomycin ointment) and the “gold standard” of systemic therapy with antimony compounds.7,8
The case reported here highlights the need to consider leishmaniasis in anyone returning from a tropical destination who has a progressive ulcer that does not respond to local care and systemic antibiotic therapy.
Shariq Haider Tropical Medicine Clinic Division of Infectious Diseases McMaster University Odette Boutross-Tadross Jasim Radhi Department of Pathology McMaster University Hamilton, Ont. Ndao Momar McGill University Centre for Tropical Diseases National Reference Centre for Parasitology Montréal, Que.