Abstract
Background
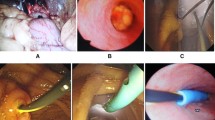
Several studies have shown the efficacy and effectiveness of the combined endoscopic–laparoscopic “rendezvous” technique for treatment of gallbladder and bile duct stones without complications, particularly pancreatitis. The so-called rendezvous technique consists of laparoscopic cholecystectomy standards with intraoperative cholangiography followed by endoscopic sphincterotomy (EST). The sphincterotome is driven across the papilla through a guidewire inserted by the transcystic route. This method allows easier and faster cannulation, thus avoiding papillary edema and pancreatic trauma. The aim of this study was to evaluate whether this method is effective in eliminating ductal stones and to verify whether the risk of postprocedure pancreatitis is diminished.
Methods
From January 2002 to September 2004, we enrolled 256 patients with cholecystocholedolithiasis detected by transabdominal ultrasound and magnetic resonance cholangiopancreatography. One hundred and twenty of these had one or more patient-related risk factors for post-endoscopic retrograde cholangiopancreatography (ERCP) pancreatitis, so they were randomized into two groups of 60 patients. In group A, the patients were treated in a single step with videolaparoscopic cholecystectomy, intraoperative cholangiography, and EST during the surgical procedure with the rendezvous technique. In group B, preoperative ERCP and EST were performed by using a traditional method of bile duct cannulation.
Results
No cases of post-ERCP pancreatitis were observed in group A, whereas six cases of acute post-ERCP pancreatitis occurred in group B (five mild and one moderate) (p = 0.0274). No procedure-related mortality was recorded.
Conclusion
In cholecysthocholedocholithiasis, the combined laparoscopic–endoscopic approach prevents post-ERCP pancreatitis in cases with patient-related risk factors for this complication.

Similar content being viewed by others
References
Andriulli A, Leandro G, Niro G, Mangia A, Festa V, Gambassi G, et al. (2000) Pharmacologic treatment can prevent pancreatic injury after ERCP: a meta-analysis. Gastrointest Endosc 51: 1–7
Arcidiacono R, Gambitta P, Rossi A, Grosso C, Bini M, Zanasi G (1994) The use of a long-acting somatostatin analogue (Octreotide) for prophylaxis of acute pancreatitis after endoscopic sphincterotomy. Endoscopy 26: 715–718
Baillie J, Paulson EK, Vitellas KM (2003) Biliary imaging: a review. Gastroenterology 124: 1686–1699
Carr-Locke DL (2002) Therapeutic role of ERCP in the management of suspected common bile duct stones. Gastrointest Endosc 56: 170–174
Cavallini G, Tittobello A, Frulloni L, Masci E, Mariani A, Di Francesco V, et al. (1996) Gabexate for the prevention of pancreatic damage related to endoscopic retrograde cholangiopancreatography. N Engl J Med 335: 919–923
Davis WZ, Cotton PB, Arias RS, Williams DM, Onken JE (1997) ERCP and sphincterotomy in the context of laparoscopic cholecystectomy; academic and community practice patterns and results. Am J Gastroenterol 92: 597–601
European Association for Endoscopic Surgery Committee (1998) Diagnosis and treatment of common bile duct stones (CBDS). Surg Endosc 12: 856–864
Fanti L, Agostoni M, Casati A, Guslandi M, Giollo P, et al. (2004) Target-controlled propofol infusion during monitored anaesthesia in patients undergoing ERCP. Gastrointest Endosc 60: 361–366
Frazee RC, Robert J, Symmonds R, Hendricks JC, Snyder S, et al (1993) Combined laparoscopic and endoscopic management of cholelithiasis and choledocholithiasis. 166: 702–705
Freeman ML, DiSario JA, Nelson DB, Fennerty B, Lee JG, Bjorkman DJ, et al. (2001) Risk factors for post ERCP pancreatitis: a prospective multicenter study. Gastrointest Endosc 54: 425–434
Freeman ML, Guda N (2004) Prevention of post-ERCP pancreatitis: a comprehensive review. Gastrointest Endosc 59: 845–864
Freeman ML, Nelson DB, Sherman S, Haber GB, Herman ME, Dorsher PJ, et al. (1996) Complications of endoscopic biliary sphincterotomy. N Engl J Med 335: 909–918
Gottlieb K, Sherman S, Pezzi J, Esber E, Lehman GA (1996) Early recognition of post-ERCP pancreatitis by clinical assessment and serum pancreatic enzymes. Am J Gastroenterol 91: 1553–1557
Huntigton TR, Bohlman TW (1997) Laparoscopic biliary guidewire: a simplified approach to choledocholithiasis. Gastrointest Endosc 45: 295–297
Iodice G, Giardello C, Francica G, Sarrantonio G, Angelone G, Cristiano S, et al. (2001) Single-step treatment of gallbladder and bile duct stones: a combined endoscopic–laparoscopic technique. Gastrointest Endosc 53: 336–338
Ko CW, Lee SP (2002) Epidemiology and natural history of common bile duct stones and prediction of disease. The NIH State-of-the Science Conference: ERCP for diagnosis and therapy. Gastrointest Endosc 56(Suppl): 165–169
Lella F, Bagnolo F, Colombo E, Bonassi U (2004) A simple way of avoiding post-ERCP pancreatitis. Gastrointest Endosc 59: 830–834
Long WB, Shwarz W, Ring EJ (1984) Endoscopic sphincterotomy assisted by catheterization antegrade. Gastrointest Endosc 30: 36–39
Loperfido S, Angelini GP, Benedetti G, Chilovi F, Costan F, De Berardinis F, et al. (1998) Major early complications from diagnostic and therapeutic ERCP: a prospective multicenter study. Gastrointest Endosc 48: 1–10
Masci E, Toti G, Mariani A, Curioni S, Lomazzi A, et al. (2001) Complications of diagnostic and therapeutic ERCP: a prospective multicenter study. Am J Gastroenterol 96: 417–423
Pasha TM, Therneau T, Petersen BT (1997) Economic analysis of gabexate mesilate in post-ERCP pancreatitis [Abstract]. Gastroenterology 112: A471
Petelin JB (2002) Surgical management of common bile duct stones. Gastrointest Endosc 56(Suppl): 183–189
Shorvon PJ, Cotton PB, Mason RR (1985) Percutaneous transhepatic assistance for duodenal sphincterotomy. Gut 26: 1373–1376
Singh P, Das A, Isemberg G, Wong RCK, Sivak MV, Agrawal D, Chak A (2004) Does prophylactic pancreatic stent placement reduce the risk of post-ERCP acute pancreatitis? A meta-analysis of controlled trial. Gastrointest Endosc 60: 544–550
Testoni PA, Bagnolo F (2001) Pain at 24 hours associated with amylase levels 5 times greater than the upper normal limit as the most reliable indicator of post-ERCP pancreatitis. Gastrointest Endosc 53: 33–39
Testoni PA, Bagnolo F, Caporuscio S, Lella F (1999) Serum amylase measured four hours after endoscopic sphincterotomy is a reliable predictor of postprocedure pancreatitis. Am J Gastroenterol 94: 1235–1241
Testoni PA, Caporuscio S, Bagnolo F, Lella F (1999) Twenty-four hour amylase predicting pancreatic reaction after endoscopic sphincterotomy. Endoscopy 31: 131–136
Testoni PA, Lella F, Bagnolo F, Caporuscio S, Cattani L, Colombo E, et al. (1996) Long-term prophylactic administration of octreotide reduces the rise in serum amylase after endoscopic procedures on Vater’s papilla. Pancreas 13: 61–65
Tham TCK, Carr-Locke DL (1999) Endoscopic treatment of bile duct stones in elderly people. Br Med J 318: 617–618
Tham TC, Vandrvoort J, Wong RC, Carr-Locke DL (1996) Endoscopic sphincterotomy with gallbladder left in situ versus open surgery for common bile duct calculi. Lancet 348: 264
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lella, F., Bagnolo, F., Rebuffat, C. et al. Use of the laparoscopic–endoscopic approach, the so-called “rendezvous” technique, in cholecystocholedocholithiasis. Surg Endosc 20, 419–423 (2006). https://doi.org/10.1007/s00464-005-0356-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-005-0356-6