The Addiction and Mental Health Strategic Clinical Network (AMH SCN) collaborates with many organizations and stakeholders to improve the care provided to Albertans for addiction and mental health.
Quantitative and qualitative data direct the prioritization of AMH SCN projects.
The AMH SCN has incorporated the voices of people with lived experience in projects such as the evaluation of community-based naloxone, redesigning of emergency departments to improve the experience of youth with addiction and mental health issues and awarding of grants offered by the AMH SCN.
Mental illness and substance misuse are important public health problems in Canada. They are common, often co-occur 1 and have extensive impact on the individual, society and the health care system.2 In 2015, the Canadian Institute of Health Information reported that youth visits to the emergency department for mental health concerns have increased in Canada, while visits for other causes have remained steady or declined.3 In Alberta, the number of deaths related to opioid overdose doubled every year (from 2014 to 2017).4 Furthermore, an internal provincial report found that youth with mental illness and their caregivers find visits to the emergency department distressing.
Since 2013, addiction and mental health care has been a stated clinical and research priority at both provincial and federal levels. Many in and outside of Alberta Health Services (AHS) provide high-quality care for people who have addiction or mental health care needs. However, the need for care demonstably outpaces the available services.5 The Addiction and Mental Health Strategic Clinical Network (AMH SCN; www.ahs.ca/amhscn) was established in 2012 to enhance the prevention and treatment of mental health disorders and addiction to further the collective SCN mission to improve health outcomes for all Albertans.
The mandate of the AMH SCN is to bring research and innovation to Alberta’s system of mental health care. As such, it has established collaborations with provincial and national stakeholders, including community organizations, people with lived experience, clinicians, academic experts from institutions across Canada and groups within AHS responsible for front-line service delivery, policy and clinical knowledge, data collection and reporting. The AMH SCN has used both quantitative and qualitative research to prioritize the projects. The Strategy for Patient-Oriented Research (supported by the Canadian Institutes of Health Research, www.cihr-irsc.gc.ca/e/41204.html) emphasizes the value of patient-oriented research and patient engagement to health systems. The AMH SCN has purposefully conducted all of its projects with stakeholders and partners from different backgrounds (i.e., clinicians, administrators, patient representatives, researchers and community partners) and consciously centred the voices of people with lived experience to generate and interpret Alberta-specific data and prioritize areas of focus (see figure and Appendix 1, available at www.cmaj.ca/lookup/suppl/doi:10.1503/cmaj.190586/-/DC1).
Involvement of Albertans with lived experience of addiction or mental health care needs in innovation and research directly supports the patient-centred care focus of AHS. People with lived experience include those with direct-care needs and their caregivers, because both perspectives are vital to a health care system that strives to constantly improve patient care. The AMH SCN designed and administered a call for research projects that supported the mental health mandate of the Alberta government.6 For this call, people with lived experience were active, full members of the steering committee and a panel that reviewed the top 10 applications (based on scientific peer review) for feasibility and value to the system. Evaluations by people with lived experience were incorporated with substantial weight when funding decisions were made.
An evaluation of this process of involving people with lived experience in decisions on research funding found that many stakeholders considered that the process led to the funding of important, scientifically rigorous projects and inclusion of the perspective of people with lived experience would be a good model for future grant calls.
The Alberta Community Based Naloxone Program evaluation (co-led by the AMH SCN) ensured that the most effective ways of distributing overdose response kits to community members were enhanced.7 This resulted in increased access and use, and the AMH SCN facilitated relationships that resulted in practical improvements to the program. Community harm reduction agencies were vital in understanding how the kits were being used and in collection of front-line data for the study. Originally, the AMH SCN planned to include people with lived experience of substance use and naloxone kit use on the evaluation working group; however, when co-designing the plan with people with lived experience, we learned that they felt that it would be more effective to connect with individuals through existing community harm reduction agencies by leveraging established trusting relationships. This led to collaborative work: the agencies raise issues from individuals to the working group, and the working group works to solve the identified problems. Outcomes from this work included increasing the dose of naloxone in the kits (based on feedback that more than 1 kit was needed to reverse many overdoses) and a directive from the CEO of AHS that all emergency departments in Alberta should distribute overdose response kits without barriers (based on findings from surveys as to why kits were not available in some locations with need; https://extranet.ahsnet.ca/teams/policydocuments/1/clp-distn-naloxone-kits-hcs-214.pdf).
Substantial increases in visits to the emergency department by youth with addiction or mental health issues6,8 led the AMH SCN and the Emergency Strategic Clinical Network to investigate the experience of youth and families in Alberta’s emergency departments. Although this work included quantitative analysis of visits throughout the province and mapping of time spent in the emergency department by the patient from a systems perspective, the patient and family experience was the focus of the study design, data analysis and resulting suggestions. Youth and families co-designed the surveys used to gather qualitative data from patients to ensure language was patient friendly and the questions meaningful to people with lived experience. Youth and families played an integral role in validating the qualitative analysis through focus groups and webinars, and in the presentation of these findings back to operational leaders, physicians, front-line staff and researchers. This led to suggestions not typically addressed within the health care system: focussing on providing patient comforts to youth and families in the emergency departments (e.g., charging cables and art supplies), and the importance of providing support and resources for family members who accompany youth to the emergency department. Incorporating these suggestions is an ongoing project supported by the AMH SCN.
The AMH SCN has encountered several challenges over the years. First, patients with addictions and mental health disorders face considerable stigma in society and also from other fields of medicine. Second, there is a lack of providers (e.g., the number of psychiatrists in the province does not meet the guidelines from the Canadian Pyschiatric Association). Funding to support implementation-orientated research in Canada is also limited, which results in challenges to changing clinical practice. When practitioners face pressure to provide service, adoption of new initiatives can be limited. There is also an inherent tension between academic researchers and health care systems because they have different incentives. The AMH SCN must work to bridge that divide to ensure that key priorities are being moved forward in a manner that benefits both.
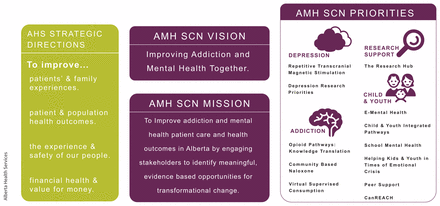
Strategic directions and priorities of the Addiction and Mental Health Strategic Clinical Network (AMH SCN).
Image courtesy of Alberta Health Services
As the SCN approach is novel, it must be an iterative and learning system. The AMH SCN works to ensure that the voices of patients with lived experience are at the centre of all projects and to strengthen the relationships with the diverse stakeholders who deliver addiction and mental health care in Alberta. Documenting experiences through the implementation science and change management is critical for other organizations to learn from the SCN’s experiences in trying to change practice. This includes ongoing evaluation of how the AMH SCN engages with people with lived experience and stakeholders in general. Key outcomes are based on the Alberta Quality Matrix for Health from the Health Quality Council of Alberta.
Footnotes
Competing interests: Kay Rittenbach is an employee of Alberta Health Services (AHS). Frank MacMaster and Nick Mitchell are remunerated through contracts with AHS. No other competing interests were declared.
This article has been peer reviewed.
Contributors: Kay Rittenbach and Frank MacMaster conceived the work. Kay Rittenbach wrote the original draft of the manuscript. Frank MacMaster and Nick Mitchell drafted the work and reviewed it critically for important intellectual content. All of the authors gave final approval of the version to be published and agreed to be accountable for all aspects of the work.
Funding: This work did not receive external funding. Members of the Addiction and Mental Health Strategic Clinical Network have received funding from the Canadian Institutes of Health Research, the Canadian Research Initiative in Substance Misuse, Alberta Innovates and the University Hospital Foundation Johnson & Johnson Alberta Health Innovation Partnership.

