In her defence of the alternative views on Lyme disease diagnosis behind Bill C-442, Zubek1 is certainly right to focus on the patients in her response to CMAJ’s article on Lyme disease.2 Many people who are under the impression that they have Lyme disease based on alternative approaches to diagnosis are disabled and in need of an open-minded approach to care. What will not help is a flawed diagnosis.
Lyme disease is making ecological inroads in Nova Scotia, southern Ontario and elsewhere, but Zubek writes from British Columbia. From her letter, one might think Lyme disease is everywhere, regularly missed, and that all we have to do to sort things out is employ alternative testing from specialty laboratories in the United States or diagnose Lyme disease based on any array of nonspecific findings.
In actual fact, ticks of all stages are under regular surveillance in BC using methods capable of detecting all strains of Borrelia with sensitive polymerase chain reaction methodology.3 As in the 1990s, only 1 in 200 Ixodes ticks in the province carry the pathogen, it is the standard North American strain, and this prevalence remains 50- to 100-fold less than in highly endemic areas in the US Northeast.
Henry’s observations4 that family physicians do treat enlarging circular rashes as Lyme disease means that we have considerable vigilance on the front line, but given the broad array of dermatologic entities that may cause such a rash, also implies that an appropriate degree of overtreatment is going on, not that every case is Lyme disease. In the area of testing, a definitive study has shown that “specialty labs” not only failed to perform better than reference laboratories in finding Borrelia infection, but also, outrageously, labelled more than 50% of healthy controls as having it.5,6
The term junk science applies when one holds onto a nontestable hypothesis, fails to test it and expects one’s critics to do so. In 2015, we should not state that a clinical diagnosis based, not on specific Borrelia-associated pathology, but on any array of nonspecific symptoms, is the best we can do.
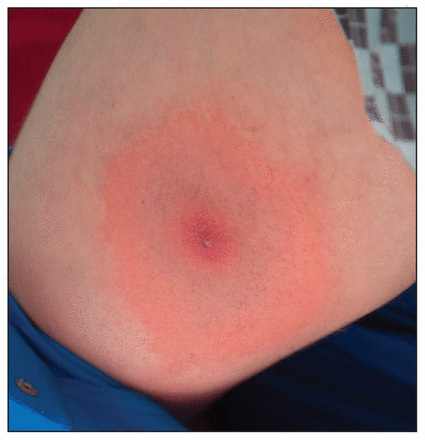
Image courtesy of nyul/iStock
I welcome Zubek’s advocacy for a stronger model of patient care for people with difficult chronic symptoms, but note that flawed and premature conclusions about etiology hurt the very patients we are trying to help.

