A 41-year-old woman presented to the emergency department with a six-day history of headache and fluctuating weakness in her left arm. Two weeks earlier, she had been prescribed prednisone 1 mg/kg per day for an active flare-up of ulcerative colitis. Clinical examination, including a full neurologic examination, was unremarkable. Computed tomography (CT) of the brain and subsequent magnetic resonance imaging (MRI) showed multifocal hemorrhagic lesions, likely secondary to extensive dural venous and cortical vein thrombosis (Figure 1A). To investigate ongoing rectal bleeding, an abdominal CT scan was ordered: it showed pancolitis and multiple focal hepatic and portal venous thromboses (Figure 1B). A therapeutic dose of intravenous unfractionated heparin was started. Flexible sigmoidoscopy confirmed mild inflammation consistent with colitis. The results of an extensive thrombophilia workup were negative. The treatment was changed to a therapeutic dose of low-molecular-weight heparin, and the patient was discharged with a maintenance dose of 20 mg/d of rivaroxaban.
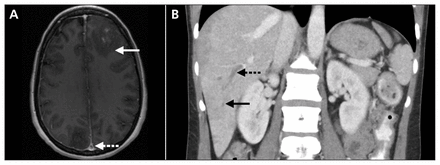
(A) Magnetic resonance imaging (T1-weighted) of the brain with gadolinium in a 41-year-old woman with a flare-up of ulcerative colitis, showing a hemorrhagic lesion (white arrow) and a sagittal sinus thrombus (white broken arrow). (B) Coronal computed tomography scan of the abdomen showing a portal vein thrombus (black broken arrow) and a hepatic vein thrombus (black arrow).
Patients with inflammatory bowel disease (IBD) have a two- to threefold increased risk of venous thromboembolism (VTE) compared with the general population.1 In a large, prospective cohort study involving patients with an IBD flare-up, the risk of VTE was increased among patients admitted to hospital (absolute risk 37.5 per 1000 person-years v. 13.9 per 1000 person-years in the control group) and ambulatory patients (absolute risk 6.4 per 1000 person-years v. 0.4 per 1000 person-years in the control group).2
The cause of VTE in patients with IBD is likely multifactorial but does include a state of hypercoagulation triggered by activation of the coagulation cascade, fibrinolysis and platelet activation during systemic inflammation.3 Most of the VTEs are deep vein thromboses in the legs and pulmonary embolisms; however, they can develop in unusual anatomic sites, including cerebral and intra-abdominal veins.4
The Canadian Association of Gastroenterology consensus statement strongly recommends anticoagulant thromboprophylaxis in patients admitted to hospital with moderate to severe IBD flare-ups without severe bleeding.5 Although outpatients with IBD flare-ups have a 16-fold increased risk of a VTE, the statement currently recommends against anticoagulant thromboprophylaxis5 in outpatients, because the absolute risk is low and is one-sixth the risk among inpatients with IBD flare-ups.2 Outpatients with active IBD should be counselled about the signs and symptoms of VTE, including the less common anatomic sites where VTEs may develop.
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
The authors have obtained patient consent.
For references, please see Appendix 1 available at www.cmaj.ca/lookup/suppl/doi:10.1503/cmaj.140251/-/DC1