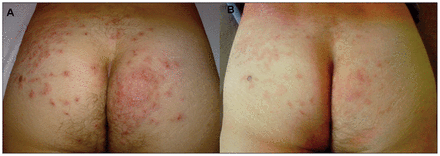
A 43-year-old man was referred for an itchy red papular eruption on his buttocks that began one month earlier during a two-week trip to Guadeloupe. The eruption began 48 hours after he spent time on the beach, and it had not responded to topical antibiotic treatment. He described the itching as intense and constant. He was otherwise well. Clinical examination revealed multiple excoriated and lichenified papules on his buttocks and lower back (Figure 1). The rest of the examination was unremarkable. History of exposure, symptoms and clinical findings were consistent with the diagnosis of hookworm folliculitis. Treatment with a single oral dose of ivermectin resulted in complete resolution of clinical signs and symptoms within 10 days.
(A) Multiple excoriated and lichenified papules of the buttocks and lower back of a 43-year-old man after a visit to Guadeloupe. (B) Complete resolution after a single oral dose of ivermectin.
Cutaneous larva migrans is caused by zoonotic skin-penetrating larvae, mainly Ancylostoma ceylanicum and Ancylostoma braziliense.1 In Western countries, the condition is usually seen in travellers returning from the tropics. The typical clinical manifestation (called a creeping eruption) is a serpiginous burrow 1–5 cm long.2 The infestation uncommonly presents as a papular rash that may be misdiagnosed as scabies or as a bacterial infection, as occurred in our patient. Patients often become infected when walking barefoot, sitting or lying on beaches contaminated by feces of infected animals. Although hookworm folliculitis most commonly occurs on the feet, the buttocks are the second most common site of involvement.2 Humans are accidental hosts, and larvae usually remain trapped in the upper dermis of the skin. The diagnosis is usually clinical, and no further investigation is needed.3,4
Several features may help differentiate between hookworm folliculitis and bacterial folliculitis. Pruritus is not a symptom of superficial bacterial folliculitis. In addition, in hookworm folliculitis, the hair shaft is generally not seen in the centre of the pustule, and there will be a lack of improvement despite treatment with a topical antibacterial agent. Expert opinions recommend treatment with a single oral dose of ivermectin; oral albendazole may be used as an alternative treatment.2–4 Even without treatment, spontaneous resolution usually occurs within two to eight weeks, after the trapped larvae die. There is no risk of relapse.4
Acknowledgement
The authors thank Dr. Denis Malvy for his contributions to the article.
Footnotes
-
Competing interests: None declared.
-
This article has been peer reviewed.