There are many hypotheses as to why allergy rates are soaring worldwide. It’s the product of changes in the environment. It’s genetic. It’s a function of society’s excessive obsession with hygiene and improvements in hygiene within developing countries. Or it could be a resulting of the shifting climate, dietary alterations or changing food manufacturing practices.
Whatever the root cause, though, there’s little doubt that allergies are imposing an increasing burden on the health care system and taking an increased toll in terms of human lives.
A World Allergy Organization survey indicated that an average of 22% of the populations of 30 countries had an allergy or an allergy-related ailment such as asthma (www.worldallergy.org/wad2007/allergy_practice_worldwide.pdf). Meanwhile, the United States Centers for Disease Control and Prevention estimated that there was an 18% increase (to 3 million) in the number of American children under age 18 who had a food or digestive allergy between 1997 and 2007 (www.cdc.gov/nchs/data/databriefs/db10.pdf).
A survey of 10 596 Canadian households concluded that the prevalence of “confirmed” peanut allergy among Canadians was 0.61%, while the prevalence for tree nuts, fish, shellfish and sesame seeds was 0.68%, 0.10%, 0.73% and 0.03%, respectively (www.sciencedirect.com/science/article/pii/S0091674910005373).
The advocacy group, Anaphylaxis Canada, estimates that between 20 to 50 Canadians die annually as a consequence of an anaphylactic reaction. But Beatrice Provolo, director of marketing and communications for the group, stresses that the number is but an estimate as deaths from anaphylaxis may be characterized as something else in hospitals, such as a heart attack or suffocation. “What we know from our counterparts in the US, and given that our societies aren’t that different in terms of food availability and common types of food allergies, is that they report anywhere from 150-to-200 deaths per year, and Canada is likely only 10% of that,” she says.
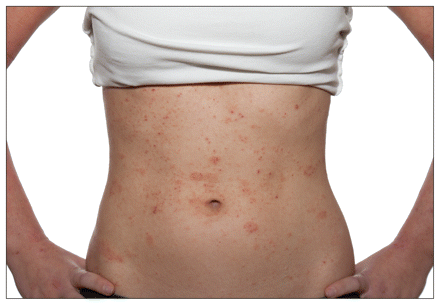
A World Allergy Organization survey indicated that an average of 22% of the populations of 30 countries had an allergy or an allergy-related ailment such as asthma.
Image courtesy of © 2011 Thinkstock
The hygiene hypothesis is the most commonly offered explanation for the rising allergy rates, particularly among children. It posits that allergies are the product of inadequate childhood exposure to bacterial and animal products in the soil, leading to the production of the antibody immunoglobulin (IgE), says Dr. Charles Listgarten, a community allergist in Toronto, Ontario.
Essentially, excessive hygiene results in inadequate stimulation of a child’s immune system, he adds. “It’s felt that by cleaning up our lifestyle, we’ve promoted allergy production.”
Others have posited that allergies may be rising because increased usage of preservatives in food alters the human immune system, or because climate change has extended plant pollination seasons, resulting in more exposure to allergens.
But Dr. Susan Waserman, an allergist and clinical immunologist at McMaster University in Hamilton, Ontario, says those propositions are little more than speculation.
For example, she notes, there are those who believe that the manner in which foods are prepared increases allergy rates. “The way we prepare peanuts, through roasting rather than boiling, seems to either change the allergenicity or make people develop specific IgE antibodies. There are places, like in Thailand and China, [where people] eat peanuts, but do not prepare them the same way we do, and don’t have the prevalence of allergies.”
Another possibility could be that parents, in some cases, are introducing their children to allergens at an earlier age, says Dr. Moshe Ben-Shoshan, an allergy researcher with the Department of Pediatrics at the Montreal Children’s Hospital in Quebec.
Ethnicity and age of exposure could also play roles, Ben-Shoshan adds, citing a study that indicated consumption of peanuts at an earlier age substantially lowers the risk rate for later developing an allergy to peanuts (http://ddr.nal.usda.gov/bitstream/10113/42633/1/IND44389411.pdf).
The exposure hypothesis posits that introduction of foods earlier on in childhood helps a child to build a tolerance to a particular allergen, Ben-Shoshan says. But he adds that the ability of children to tolerate an allergen quickly fades as they age.
There is inadequate evidence to support other hypotheses for increasing allergy rates, such as one holding that intestinal flora dictate whether an individual will have allergies or another that climate change increases overall pollen counts, Waserman says.
The uncertainties are vast, Ben-Shoshan says. “We don’t know exactly why some people get allergies to foods and others don’t. We think there is an interaction between genetic and environmental factors. But we still don’t know.”
Ben-Shoshan says that until the root cause is ascertained, all that can be done for allergy sufferers is to either avoid exposure to the allergen or use an epinephrine injector in cases where a patient is at risk of anaphylaxis. Current research is focusing on expanding treatment options to include the use of desensitization and tolerance techniques in cases where a patient is at high risk of anaphylaxis, he adds.
Others hope to develop methods of more readily identifying children at risk through genetic testing, Lisgarten says. “If you can do a genetic analysis that can reliably predict their risks of developing allergies in the future, that would be great.”

