- © 2008 Canadian Medical Association
National organ allocation mechanism to be sought
It is, to be sure, a bold claim. But the head of the nation's blood program says the days of incoherence in Canada's myriad organ donation programs are entirely numbered.
Canadian Blood Services Chief Executive Officer Dr. Graham Sher says the federal, provincial (except Quebec) and territorial governments have agreed in principle to develop an “integrated national organ donation system,” including national oversight and allocation mechanisms for all organs and tissue.
But it will be some years before the fragmentation that now typifies organ donation programs ((CMAJ 2006;175[9]:1043-5) actually ends. Sher says a national registry and mechanism for allocating organs, similar to the US United Network for Organ Sharing; standardized consent policies; nation-wide wait lists for all available organs; mandatory organ sharing and other requisite elements of a national organ donation and transplantation program will be “phased-in” over a number of years. And then only after “extensive” nation-wide consultations.
The “first step” in that process was the Aug. 12, 2008 announcement that the various levels of government would collectively pump $35 million over 5 years into the development of 3 specialized national donor registries: for highly sensitized patients; for paired exchanges between living donors in different provinces; and for urgent status patients. To that end, Canadian Blood Services was designated as responsible for developing the 3 registries, as well as for “public eduation and awareness, support for leading clinical practices and system performance improvement, and the development of a strategic plan.”
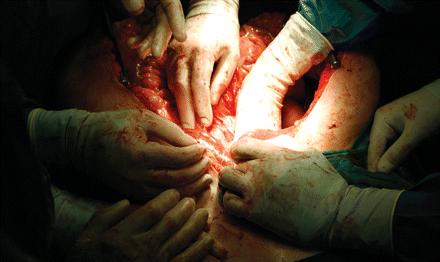
Surgeons extract the liver and kidney of a brain-dead woman for organ transplant. Image by: Reuters / Fabrizio Bensch
The national not-for-profit organization also gobbled up the Canadian Council for Donation and Transplantation, an independent nonprofit corporation which had been struck in 2001 and given roughly $18 million over 5 years to provide advice to the Conference of Deputy Ministers of Health. The now-defunct advisory body told CMAJ in 2006 that it had no interest in becoming any form of national oversight agency.
Sher says Canadian Blood Services received assurances from the provinces that they'll set aside the relentless jurisdictional wrangling that has historically characterized organ donation programs in the interest of finally improving Canada's woeful organ donation rates. According to the Canadian Organ Replacement Register, there were 4195 Canadians awaiting organ transplants at the end of 2007, in which 2188 transplants were performed.
“It's a very clear signal on the part of the provinces to get their collective act together to create a national system and to provide national support mechanisms to the local and provincial transplant programs that don't exist today at the national level,” Sher says. “I get a very strong sense of commitment on their part to work collaboratively to make sure there is a national system in place. I think there are very legitimate questions and concerns around where does the role of the national system start and end, and where do the roles of the provincial systems start and end, and where do the roles of the local transplant programs begin and end. And I think that's part of what we will address at the conference in September. But there are certain things that can only be done at a national level effectively that can't be done across different provinces differently and I think that's the one advantage of what's being generated here.”
Canada should take its lead from international developments, Sher adds. “We want to make sure there isn't a sense of territoriality here. This isn't a function grab by Canadian Blood Services. We were asked to take this on and we will work collaboratively with the provincial programs to make sure that all roles and responsibilities are clearly defined. But I think other countries have shown us, whether it's Spain or the United States, and now the UK [United Kingdom] and Australia, that what is needed is national oversight and national allocation authority so that the programs can work collaboratively to optimize the donation and transplantation opportunities.”
Sher adds that Canadian Blood Services received assurances from all levels of government that the monies needed to develop national mechanisms would be provided, once the business plans for such initiatives are developed.
A condition of Canadian Blood Services involvement was that the hundreds of millions of dollars that will ultimately be needed would ultimately be made available, he says. “We are not going to subsidize the new organ donation programs out of blood donation revenues. Absolutely not. Any new initiatives that will be undertaken will have to be appropriately funded.”
All levels of government were apprised of the massive amounts of money that will be needed, Sher says, noting that Australia recently invested $150 million to bolster its system, while the UK funnelled £7 million into its regime.
The first step in developing the requisite mechanisms will be the national conference to be held in Ottawa in September 2008. It will address a range of policy issues, including standardization of consent policies, mandatory hospital reporting of ICU or emergency department deaths and incentives for donation.
“Everything is on the table,” Sher says. “Certainly, my view, from Canadian Blood Services' perspective, is that there are no sacred cows in there. We need to challenge some of the long-held assumptions that things are better done at a provincial program level and ask the question about whether it is better done nationally.”
Air pollution death toll to soar
Canadians might want to consider wearing masks as they move about their daily chores after a Canadian Medical Association study indicated that 21 000 citizens will die this year as a result of the effects of air pollution.
That will rise to 39 000 by 2031, by which point the economic costs of air pollution will rise to $18 billion from $8 billion, according to the report, released Aug. 13, 2008, and entitled “No Breathing Room: National Illness Costs of Air Pollution.”
The cumulative totals by 2031?
Roughly 800 000 dead and an economic cost of $250 billion.
The extrapolations, based on a set of algorithms developed by a team of university researchers for the Ontario Medical Association in 2000, also indicate that over 9000 hospital visits, 30 000 emergency department visits and 620 000 visits to doctors' offices this year will be due to air pollution.
CMA Technical Advisor on Health and the Environment Dr. Ted Boadway says the national algorithms are based on the combined health effects and economic costs of 2 pollutants: ozone and particulate matter. Arguing that the methodology can withstand any measure of scrutiny, Boadway says that, if anything, it underestimates the impact of chronic diseases.
Limitations would include the lack of uniform provincial submissions to the Canadian Institute for Health Information, whose data was used to derive the staggering findings.
The Illness Costs of Air Pollution software, downloadable at www.cma.ca, allows Canadians to forecast the health damages of air pollution on a provincial (or even down to a census division) level.