The crisis in hospital emergency departments (EDs) across Canada, which has led to strikes, walkouts, investigations and finger-pointing, is directly linked to shortages of hospital beds, say emergency physicians.
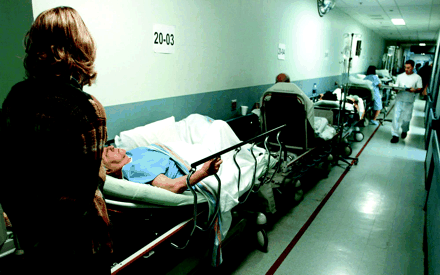
Figure. A 40% cut in hospital beds since 1994 makes this is a familiar ED scene across Canada. Photo by: Canapress
A string of high-profile problems at EDs in several provinces have turned a spotlight on patients enduring long waiting times for treatment or admission to hospital. These incidents include:
• The death of Dorothy Madden, a 74-year-old Winnipeg woman who waited 6 hours in St. Boniface Hospital's ED before going into cardiac arrest.
• The demotion of Dr. John Witt, former head of the ED at the Royal University Hospital in Saskatoon, after he wrote a letter to the provincial minister of health calling for increased funding because ED overcrowding was endangering patients (CMAJ 2004; 170[10]:1527).
• The mass resignation of 21 doctors at the Nanaimo Regional General Hospital on Vancouver Island over the doctor–patient ratio in the ED.
Overcrowding that denies patients timely treatment is a common theme in all of these situations, says Dr. Alan Drummond, chair of public affairs for the Canadian Association of Emergency Physicians (CAEP). But, unlike the prevailing political wisdom that attributes overcrowding to too many patients seeking urgent treatment for non-emergencies, Drummond and his organization point to another cause. They say the real issue is the shortage in acute care hospital beds.
“The correct approach to solving overcrowding is in fact to increase acute care bed capacity and increase bed flexibility and appropriate utilization of beds. That's really what it comes down to,” says Drummond, who practises emergency medicine in Perth, Ont.
Over the past decade there has been a 40% decrease in hospital bed capacity in Canada. Closing beds translates into more patients being “warehoused” on stretchers and treated in corridors in hospital EDs when they need to be admitted.
An aging population, increased numbers of homeless and de-institutionalized people and emerging infectious diseases are all straining the capacities of emergency medical staff, emergency physicians say.
There are some savings to be made by improving primary care — but not enough to equal what provinces need in extra hospital capacity, says Dr. Les Vertesi, an emergency physician at the Royal Columbian Hospital in New Westminster, BC.
Diverting the “walking wounded” through programs like Telehealth Ontario, mass influenza vaccinations and by promoting the use of walk-in clinics won't ease those stresses enough, doctors and policy analysts say. The less seriously ill are not the ones who need hospital admission, the doctors contend.
“The sickest people are the ones who require the beds, and that's what we don't have,” says Vertesi. “If we got rid of all the lower category patients it wouldn't help one bit.”
Vertesi is also BC's representative on the new national Health Council, created last June to monitor the way the Canada Health Act is being implemented. Vertesi sits on a task force that will examine the problem of surgical waiting lists, but says that can't be investigated without acknowledging the link between waiting times for surgery and the lack of beds available for patients who arrive via the ED. “They're competing for the same beds.”
Vertesi is worried that the Council's narrow mandate won't allow a thorough examination of ED overcrowding. CAEP has the same concern, citing their proposal to provincial health ministers 2 years ago to host a forum on emergency services in Canada. The response, a November 2002 letter from Nova Scotia's Jamie Muir, the health minister then chairing the first ministers' group, completely ignored the request.
Dr. Joel Lexchin, an emergency physician and associate professor at York University's School of Health Policy and Management, also cites bed blockages as the key to ED overcrowding, although other measures — such as improved home care to keep patients with chronic illnesses out of the ED — are also needed.
He also recommends better communication between specialists and general practitioners to help manage people with chronic illnesses, as well as long-term, stable health care funding, to enable hospitals and health-care regions to plan ahead for 5 years or more.
Montreal's Regional Health Board has had some success in dealing with overcrowding. Over the last 2 years, the board has increased home care services and improved access to medical clinics and outpatient services to free beds within hospitals, says Julie Boucher, who oversees EDs for the board. The board has also developed a management guide to improve coordination between emergency physicians and those coordinating admissions. Some hospitals have hired medical coordinators who are on-site or on-call 24/7.
There has been progress, but the board's goal, to ensure no patient waits more than 12 hours on a stretcher to get a hospital bed, hasn't been reached.
In Ontario, Liberal Premier Dalton McGuinty campaigned on promises to open 1600 more hospital beds, hire 8000 nurses and make it easier for international medical graduates to practice medicine — promises he has since delayed, given the province's fiscal woes.
In Halifax, where charge nurse Del MacKinnon works in emergency at the Queen Elizabeth II Health Sciences Centre, the province did open 21 new long-term beds in early April. The decision was part of a 10-point plan responding to charges by unionized staff that patient backlogs were endangering lives. “Hopefully the turnover will open up other beds [for acute care patients],” says MacKinnon.
Other proposed solutions include the type of pilot program tried in Rivière-du-Loup, Que., where pharmacists were an integral part of ED medical teams, analyzing patient files and responding to drug allergies, incorrect dosages or prescriptions and drug interactions.
These solutions may help reduce backlogs, but will not eradicate them because they don't address the underlying cause, maintains Drummond and CAEP. “The principal problem for emergency medicine is overcrowding, and we have a solution: increase bed capacity. The question is whether we have the political will to enact that solution.” — Laura Eggertson, CMAJ

