Although increased physician diversity has been shown to improve patient care and reduce health care disparities,1,2 the current demographics of the profession do not reflect the population of Canada as a whole, including the proportion of Black Canadians. 3,4 The racial homogeneity of the medical profession did not occur by chance; rather, it is the product of discriminatory policies that have systematically prevented Black and other racialized students from pursuing medical training. Historians have shown that discriminatory admission policies were common in North American medical schools well into the middle of the twentieth century, and these continue to have a measurable impact on the number of Black medical school graduates in the present day.5,6
Argueza and colleagues7 argued that medical training institutions that want to address the crisis of representation must first turn their attention inwards and “thoroughly investigate how systemic racism is built into their walls.” After a reckoning with its own history of anti-Black admissions policies, the School of Medicine at Queen’s University chose to make this history a permanent fixture of its undergraduate curriculum. We discuss the development of this antiracist curriculum that uses local history as a lens for examining how institutional racism has shaped the history of the medical profession.
Anti-Black admissions policies at Queen’s School of Medicine
In 1918, Queen’s University instituted a ban on Black medical students, pressuring its 15 Black students to leave the program and barring future admissions (Figure 1). At that time, the university pointed the finger at residents of Kingston, who allegedly refused to be treated by Black students, which led to insufficient clinical training opportunities for them. However, recent research by Edward Thomas, a PhD candidate at Queen’s, uncovered a different motivation for the ban. Archival documents suggest that Queen’s University expelled its Black students in hopes of currying favour with the American Medical Association, an organization that publicly supported segregated medical education. Although the ban has not been officially enforced at Queen’s since 1965, the university senate’s motion to ban Black medical students remained on the books until 2018, when it was formally repealed.8
The graduating class of the Queen’s Faculty of Medicine on the steps of Jackson Hall in 1914. This cohort was one of the last to include Black students before the school’s ban on Black medical students in 1918.
Image courtesy of Queen’s University Archives
The curriculum
After the ban was officially repealed, the Commission on Black Medical Students was tasked with properly acknowledging the historic injustices perpetuated by the School of Medicine. One of the commission’s goals was to develop curricular content about the ban, both as a form of ongoing remembrance and as an introduction to the topic of anti-Black racism in medicine. The new session, “Who gets to be a doctor?,” was designed to complement the existing history of medicine program at Queen’s. Historians have made many arguments about the importance of history for medical education, including that history “offers essential perspective about the causes of persistent inequalities and possible solutions.”9 Since students are most engaged when the relevance of history to contemporary social problems is made explicit, the curriculum links the history of the ban directly to the profession’s lack of diversity in the present. Students are then asked to apply their historical knowledge in a discussion of current efforts to reform the medical admissions process.
The session occupies 3 curricular hours, a 1-hour directed independent learning module before the session and a 2-hour discussion-based class session. The independent module, created with Articulate Storyline 360 software, is used to deliver the bulk of the historical content to reserve in-class time for discussion and reflection. Students read about 2 historical instances of discrimination at Queen’s, namely a ban on female medical students from 1883 to 1943, and the ban on Black students from 1918 to 1965. These case studies were developed with the goal of accurately recounting past events; exploring the roles played by school administration, faculty and students; and identifying the impact of these events on individuals, the institution and the medical profession at large. Although the module primarily focuses on racism in medical admissions, the inclusion of the ban on female medical students allows students to consider how different forms of discrimination have intersected over time. The second part of the module describes how admissions policies and the demographics of the profession have evolved in recent decades. Particular attention is paid to the efforts of student activists, who were responsible for many reforms that reshaped the profession beginning in the 1960s.
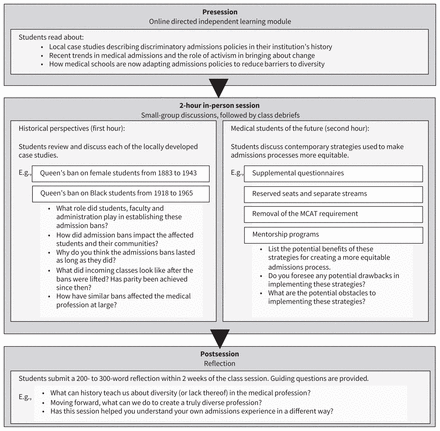
The 2-hour in-class session aims to foster critical analysis of the content introduced in the online module. About 100 students are seated in randomly selected small groups of 6 or 7 within a larger lecture hall. Groups have 15 minutes to review each case study from the module and answer the corresponding discussion questions (Figure 2). During this time, 2 instructors (1 historian and 1 clinician) circulate around the room and, after each case, debrief with the full class. In the second hour, groups are asked to investigate 1 of 4 current programs designed to diversify admissions, and then discuss the pros and cons of each. During this discussion, students are invited to share their own personal experiences and suggest other strategies for reforming admissions processes. In feedback from the session, students have suggested that a representative of the admissions committee be invited to participate in this discussion, an excellent suggestion that would allow students to provide feedback on our institutional policies.
Outline of the “Who gets to be a doctor?” session, including sample discussion questions. Note: MCAT= Medical College Admission Test.
Within 2 weeks of the in-class session, students must submit a written reflection (200–300 words), with guiding questions provided. This reflection serves as a structured opportunity for students to articulate what they took away from the session and how the discussion may have changed their perspective on their own admissions experience.
Reflections and future directions
Since Fall 2019, this curriculum has been delivered to 6 separate classes of medical students at Queen’s (about 600 students), both in person and virtually via video call. Although the implementation of the curriculum met institutional goals, it is difficult to quantitatively measure how successfully it addressed the broader goal of inculcating antiracist principles. Anonymously collected student feedback suggests that the session was effective in improving students’ knowledge of the history of anti-Black racism at Queen’s, as well as systemic racism within the profession more broadly. We received no reports of student discomfort with the session.
The session will be a fixture in the School of Medicine’s undergraduate program as a mandatory session for first-year students. It is currently placed within the “Introduction to Physician Roles” course, where it complements other sessions on professionalism, advocacy and medical ethics. This session is not a one-off, but rather a foundation upon which a robust antiracist curriculum can be built. Since the introduction of “Who gets to be a doctor?,” new sessions have been added throughout pre-clerkship to address issues of oppression, diversity and social justice, while other content has been amended or revised. Queen’s students have also spearheaded efforts to improve racial representation in learning materials and to reform the admissions process to increase the number of Black and Indigenous students enrolled each year.
The session’s place in the undergraduate program serves not only as a reminder of the institution’s past mistakes; it is an acknowledgement that medical schools are racialized organizations. As medical schools publicly commit themselves to the principles of equity, diversity and inclusion, it is important to recall that these institutions have not been raceneutral, despite the existence of seemingly race-neutral structures, including admissions processes.10 The profession’s lack of diversity has its origins in blatant structural discrimination. It is only by studying history that leaders and educators may be better equipped to address the inequities of the present.
Using the framework presented in Figure 2, this curriculum could be adapted and replicated at medical schools across different national contexts. Medical educators interested in adopting this framework would benefit from reaching out to historians or archivists at their own institutions, whose expertise can guide the development of local case studies. Through interdisciplinary collaboration, institutions can examine their own history, support the pursuit of historical justice for those affected by policies at a particular school, and develop relevant content for their students.
Afterword
We want to acknowledge our positionality with respect to this work. Mala Joneja is an associate professor in the Department of Medicine at Queen’s University. She is a woman of colour and previous director of diversity and equity for the School of Medicine, and previous chair of the Commission on Black Medical Students, Queen’s University. Shikha Patel is a fourth-year medical student at Queen’s University. She is a woman of colour and a settler. Sabreena Lawal is an incoming resident in the Department of Otolaryngology — Head and Neck Surgery at the University of Ottawa, and a graduate of Queen’s University School of Medicine. She is a Black woman, the previous Ontario regional director of the Black Medical Students Association of Canada and a previous student member of the Commission on Black Medical Students, Queen’s University. Jenna Healey is the Hannah Chair in the History of Medicine and assistant professor in the Department of History at Queen’s University. She is a settler and a member of the Commission on Black Medical Students, Queen’s University.
Acknowledgements
The authors wish to thank the Queen’s Medicine Curriculum Committee and the Commission on Black Medical Students (CBMS) for their time in consultation about the curriculum design. The authors also thank Edward Thomas for sharing his research, which spurred the development of the CBMS and provided content for 1 of the case studies taught to students.
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/