A 24-year-old man was brought by ambulance to a rural hospital after a motor vehicle collision. On physical examination, he was hemodynamically unstable with a blood pressure of 60/40 mm Hg and a heart rate of 120 bpm. He had unequal upper-extremity blood pressures, muffled heart sounds and a left-sided flail chest. The patient required intubation, bilateral chest tubes and multiple blood transfusions. Point-of-care echocardiography was attempted, but the heart was not visualized owing to air artifacts and an abnormal anatomic position.
Initial radiography of the chest showed a left-sided flail segment and dextrocardia (Figure 1A). Computed tomography confirmed cardiac herniation into the right hemithorax, with associated torsion and narrowing of the right main pulmonary artery and constriction of the pulmonary veins (a video [Appendix 1] is available at www.cmaj.ca/lookup/suppl/doi:10.1503/cmaj.191446/-/DC1).
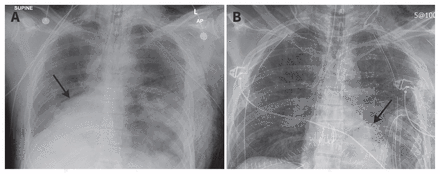
Chest radiograph of a 24-year-old man with cardiac herniation caused by blunt thoracic trauma showing (A) dextrocardia (black arrow). (B) Postoperative view showing reduction of dextrocardia and resolution of the normal heart border (black arrow).
The patient was flown in unstable condition to the nearest trauma centre and required ongoing aggressive resuscitation. On arrival, he underwent emergent bilateral thoracosternotomy to reduce the herniation and repair the pericardium (Figure 1B). He had a prolonged course in the intensive care unit secondary to difficulties with ventilation but eventually made a full recovery and was discharged home.
Pericardial rupture is uncommon, occurring in less than 0.5% of cases of blunt trauma.1 In cases of right-sided pericardial rupture, the heart can herniate into the right thorax with associated torsion of great vessels,1 which is associated with high mortality rates in patients who survive to hospital.2 Findings from chest radiography in patients with substantial thoracic trauma that should raise clinical suspicion of cardiac herniation include pneumopericardium, pneumomediastinum, a prominent cardiac silhouette or new dextrocardia. 2 Emergency consultation with thoracic or cardiac surgery is essential for definitive management of this condition, because surgical intervention is essential to restore hemodynamic stability.3 In the event of ongoing instability or cardiac arrest, resuscitative thoracotomy to detort the herniation should be considered by any physician trained in the technique.
A video of cardiac herniation after blunt thoracic trauma in a 24-year-old man is available in Appendix 1, at www.cmaj.ca/lookup/suppl/doi:10.1503/cmaj.191446/-/DC1
Acknowledgement
The authors would like to thank the large multidisciplinary team who came together to help achieve this patient’s successful outcome.
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
The authors have obtained patient consent.