Conservative treatment for knee osteoarthritis includes weight loss, modification of activity, nonsteroidal anti-inflammatory drugs, physical therapy and bracing, in select cases; this should form the initial treatment approach.
Knee injectables including hyaluronic acid, cortisone, platelet-rich plasma and combination therapies may provide effective symptom relief, and the placebo effect of intra-articular injection has been shown to exceed that of nonsteroidal ant-iinflammatory drugs.
Arthroscopic management of osteoarthritic symptoms by means of arthroscopic lavage or arthroscopic debridement has been shown to have no benefit, in several high-quality randomized controlled trials.
The effect of acetominophen has been shown to be negligible; pharmaceutical-grade (but not nutraceutical-grade) chondroitin sulphate may offer some benefit for pain relief; commonly used treatments such as acupuncture, taping, shoe wedges and transcutaneous electrical nerve conduction are not supported by evidence.
Surgical and arthroplasty options, which have been shown to be effective, should be delayed as long as possible, after all possible nonoperative treatments have been exhausted.
Osteoarthritis has a high global health and economic burden and will become the fourth leading cause of disability by the year 2020, according to data from the World Health Organization.1 Official Canadian statistics estimate that 1 in 10 Canadians aged 15 years or older suffers from osteoarthritis and prevalence increases with age.2 Symptomatic osteoarthritis most commonly affects the knee; 29% of all Canadian cases of osteoarthritis involve the knee. As the population ages and rates of obesity rise, it is estimated that the number of individuals affected will increase to one in five by 2031. A recent study estimated that loss of productivity from chronic pain and loss of mobility owing to the disease costs the Canadian economy $17.5 billion annually.3
Total knee replacement represents the definitive treatment for disabling knee osteoarthritis that has not responded to nonoperative treatments, which include analgesics, weight loss, bracing, modification of activity, physiotherapy and intraarticular injections. However, this treatment is not always advisable, particularly in young patients. Treating young patients who have pain and functional limitation owing to knee involvement is a clinical challenge; these patients have been referred to as falling into a “treatment gap,” as they are too young or may be unwilling to undergo total knee replacement.4 Available clinical practice guidelines vary substantially in both their quality and specific treatment recommendations for younger patients with osteoarthritis (Box 1).5
Evidence used in this review
A single reviewer (MK) searched PubMed, MEDLINE, Embase and Cochrane databases with combinations of the terms “knee” and “osteoarthritis,” using the “related articles” function. The search was restricted to research published over the last 10 years (Apr. 1, 2007 to Mar. 31, 2017).
Articles were screened for relevance and attention was focused on recently published research, including systematic reviews, meta-analyses and randomized controlled trials. Inclusion criteria involved all clinical articles related to knee osteoarthritis. We excluded all basic science studies, case series and case reports, as well as those studies that reported on osteoarthritis involving joints other than the knee.
We review evidence for both nonoperative and surgical treatment options that are available for young patients with primary knee osteoarthritis, focusing on high-quality clinical research — including systematic reviews, meta-analyses and randomized controlled trials (RCTs) — and guidelines published in the last decade (Box 1). We discuss conflicting treatment guidelines and provide an update on emerging treatments and ongoing research.
Why the “treatment gap” for younger patients?
The relatively young and active individual with osteoarthritis presents a challenging clinical scenario for several reasons. Such patients often seek to remain involved in sporting activities. However, as degenerative changes involving the cartilage and meniscus progress, nonoperative treatment options are often exhausted relatively quickly. The time between exhaustion of nonoperative treatment options and definitive surgical management has been described in the literature as a treatment gap.4 Those who fall into the gap are frequently younger than 60 years with early- to midstage knee osteoarthritis (Kellgren and Lawrence grade 1–3), yet may include any individual who is symptomatic and for whom nonoperative management is no longer effective.6 Such patients make up about 20% of all those affected by knee osteoarthritis, which has been estimated as 3.6 million Americans and projected to increase to 5 million by 2025.4 A recent small survey of orthopedic surgeons found that 84% perceived a need for improved treatment options for patients younger than 60 years who have osteoarthritis, and 68.4% of surgeons perceived that there is a treatment gap for these patients.6
The treatment gap exists because many nonoperative treatment options and minimally invasive surgical procedures are ineffective in long-term management of osteoarthritic symptoms. Invasive procedures such as knee arthroplasty do not meet patient expectations for continued highly active lifestyles and patients are unwilling to deal with subsequent revision arthroplasty procedures, which may be inevitable.7,8
Despite technological advances, many patients are not satisfied with their total knee replacement. A cross-sectional study of 1703 primary total knee replacements in the province of Ontario confirmed that almost one in five (19%) of patients were not satisfied with the outcome.9 The study identified that younger patients (< 70 yr) were more likely to be dissatisfied with the total knee replacement compared with those who were older at the time of the procedure.9 Similarly, a multicentre survey of 661 patients younger than 60 years who underwent total knee replacement found that many reported residual pain (33%) and stiffness (41%), and 50% were unable to return to desired sport or recreational activity.10 Recent research shows that total knee replacement is cost-effective only when performed on those with substantial functional limitations.11
Despite this, studies from the United Kingdom have found that 15% of all total knee replacement procedures are performed in patients younger than 60 years, and project a future increase.12,13 The increased risk of revision surgery in the younger population — a function of both implant longevity and increased level of activity, resulting in increased mechanical wear — heralds a particular problem with a growing need for revision surgery. A recent, large, population-based study examining 54 276 total knee replacements found the lowest implant survival rates in patients who were in their 50s at the time of index surgery.14 Younger men between the ages of 50 and 54 had a lifetime risk of revision total knee replacement of 35.0% compared with 4.4% for those aged 70 years at time of surgery.14 Quality of life and satisfaction of patients living with revision implants are much lower than for those living with primary total knee replacement.15
Which noninvasive treatments may be used for knee osteoarthritis?
Evidence-based, nonsurgical options available for managing knee osteoarthritis in both the young and older populations range from lifestyle modification and medications, to more invasive injectable therapies, some of which can be begun by primary care physicians.
Weight loss
Weight loss leads to a reduced load of forces across the knee joint and, along with exercise, may improve biomechanics and physical function. Biomechanical studies show that 1 kg of weight loss correlates to a fourfold decrease in forces across the knee.16 Frequently, weight loss alone will relieve symptoms for patients with osteoarthritic symptoms. A systematic review and meta-analysis of 44 RCTs comparing land-based exercise programs to no exercise found that exercise reduced pain burden (12 points/100, 95% confidence interval [CI] 10 to 15), improved quality of life and improved physical function (10 points/100, 95% CI 8 to 13).17 Both diet and exercise interventions have been shown to facilitate weight loss. A large RCT showed weight loss of 4.9% total body weight for diet-only intervention versus 5.7% diet-plus-exercise intervention over an 18-month period18 among people with arthritis. Low-impact aerobic exercise (swimming or elliptical training) promotes weight loss and cardiovascular health while preserving injured joint surfaces.17,19
Bracing
Knee osteoarthritis most frequently involves the medial aspect of the knee joint. Numerous studies have been published on the efficacy of unloader bracing in knee osteoarthritis, and although a recent scoping review identified that 92% of studies supported their use, 94% of available research was nonrandomized or based upon expert opinion.20 A meta-analysis of six RCTs comparing the use of a medial unloader knee brace for the treatment of medial compartment arthritis to a control orthosis found a small, statistically significant benefit favouring the brace for improvement in pain (standardized mean difference [SMD] 0.33, 95% CI 0.13 to 0.52) and function (SMD 0.22, 95% CI 0.02 to 0.41).21 Because of the low quality of available evidence, the clinical importance of these findings remains unclear.
Physical therapy and quadriceps strengthening
Strengthening exercises and physical therapy work to strengthen the leg muscles, particularly the quadriceps, to reduce load and direct knee joint stress during movement.22 A systematic review of 26 RCTs that evaluated various strengthening exercise programs in the setting of knee osteoarthritis found moderate improvements in pain, physical function and quality of life.23
Oral and topical nonsteroidal anti-inflammatory medications
Nonsteroidal anti-inflammatory medications taken orally are the most commonly prescribed treatment for osteoarthritis, prescribed to 65% of patients with osteoarthritis in the United States.24 A recent network meta-analysis assessed the effectiveness of different preparations and doses of nonsteroidal anti-inflammatory drugs for osteoarthritis pain from 74 RCTs and identified diclofenac 150 mg/day to be the most efficacious in terms of relieving pain and improving physical function.25 However, nonsteroidal anti-inflammatory drugs taken orally have potentially important gastrointestinal, renal and cardiovascular risks. Daily nonsteroidal anti-inflammatory drug use has been associated with a fourfold increase in the risk of upper gastrointestinal bleeding, and a meta-analysis of 280 RCTs identified an increase in major vascular events by one-third with the use of a COX-2 inhibitor.26,27
Topical nonsteroidal anti-inflammatory drugs are commonly used for the treatment of osteoarthritic pain because of their lower-risk profile compared with oral formulations.28 Numerous guidelines support use of topical agents and meta-analyses and systematic reviews have shown that topical diclofenac and ketoprofen are beneficial for those with knee osteoarthritis.28–30 A review of comparative studies found no statistically significant differences in the efficacy of topical and oral formulations.31 Reported adverse effects are rare, with the most commonly reported a mild skin reaction.30 Given the reported efficacy of topical agents, we suggest using topical agents initially before beginning oral agents, given the difference in safety concerns.
Oral opioid medications
There are concerns regarding the safety and effectiveness of opioid medication taken orally. A recent systematic review showed that nonsteroidal anti-inflammatory drugs and opioids provided similar pain relief for patients with osteoarthritis.32 Published clinical practice guidelines vary in their recommendations; we suggest that given their potential adverse effects, opioids should not be used as a first-line treatment option for patients with osteoarthritis (Table 1). If opioid medications are used, we suggest following a recent Canadian guideline and recommendations.39
Current clinical practice guideline recommendations for treating knee osteoarthritis33
Which injectable therapies may be used?
Commonly used intra-articular therapies include viscosupplementation, corticosteroids or combination therapies.40
Viscosupplementation
Basic science research has shown that knees affected by osteoarthritis are deficient in hyaluronic acid, a naturally occurring polysaccharide within synovial fluid, which acts as a viscoelastic shock absorber.41 Viscosupplementation aims to restore the viscoelastic properties of synovial fluid and contains anti-inflammatory and chondroprotective properties.42 Many formulations are available and vary with regard to molecular weight (low or high formulations), method of production (avian-derived or synthetic), cost and dosing (multiple or single intra-articular injection).42 While a Cochrane systematic review of 76 RCTs found improvements in knee pain and function for viscosupplementation in comparison with placebo, several other meta-analyses have produced conflicting results.33,43,44 Available data from RCTs have had small sample sizes and been methodologically poor.33 Recent evidence from a meta-analysis of 68 RCTs suggests that high-molecular-weight formulations (> 3000 kDa) show both statistically significant and clinically important thresholds of efficacy with pain relief as well as an improved safety profile.45
Corticosteroids
Corticosteroid anti-inflammatory drugs are commonly used to treat symptoms of knee osteoarthritis. A 2015 Cochrane systematic review concluded that intra-articular corticosteroid injection results in short-term improvement in pain (< 6 mo) with effects decreasing over time.46 These findings were corroborated in research in 2016 that found intra-articular cortisone injection reduced pain more than sham or no intervention (SMD −0.40, 95% CI −0.58 to −0.22). Available studies are of low quality, however, with substantial heterogeneity among trials.47 The long-term use of intra-articular cortisone has also been brought into question with the finding from a recent well-conducted RCT that found that repeated (four times per year over two years) intra-articular injection of 40 mg of corticosteroids results in greater cartilage volume loss than in patients receiving a saline control injection.48 Owing to these findings, we suggest that intra-articular cortisone be used infrequently for symptomatic control of arthritis.
Combination therapies
Combination therapies involve simultaneous injection of more than one therapy for improved pain control through their synergistic effect. Commonly used combination therapies include intra-articular corticosteroid and hyaluronic acid. An RCT comparing hyaluronic acid with a combination therapy including triamcinolone hexacetonide showed earlier onset of pain relief with the combination formulation.40 Platelet-rich plasma and hyaluronic acid combinations are now being used, with early clinical results suggesting decreased pain and functional limitations compared with platelet-rich plasma or hyaluronic acid alone.49,50
What surgical treatments are effective?
Realignment procedures or arthroplasty are the primary surgical treatments for patients with disabling symptoms of osteoarthritis not adequately controlled with nonoperative treatment.
Tibial osteotomy
Knee realignment procedures may allow for arthroplasty to be avoided or delayed; usually allow for continued high level of activity; and can preserve native joint mechanics. In cases where osteoarthritic changes are isolated to the medial or lateral compartment of the knee, the most common is high tibial osteotomy on one side to offload the diseased compartment. A Cochrane systematic review that evaluated 21 RCTs comparing osteotomy with other treatments for patients with unicompartmental osteoarthritis concluded that such procedures improved pain and function, although available evidence was of limited quality.51 A study using Finnish registry data of 3195 procedures done between 1987 and 2008 showed overall joint survivorship of 89% (95% CI 88 to 90) at five years and 73% (95% CI 72 to 75) at 10 years.52 Survivorship was found to be increased in patients younger than 50 years (hazard ratio [HR] 1.41, 95% CI 1.23 to 1.64) compared with those older than 50 (HR 1.26, 95% CI 1.11 to 1.43).52 Although there is concern regarding increased complexity of total knee replacement following high tibial osteotomy, meta-analysis of published data suggests no differences in functional outcomes, survivorship or complication rates when total knee replacement is performed in those with or without previous high tibial osteotomy.53
Unicompartmental knee arthroplasty
In cases of monocompartmental osteoarthritis — that is, where only one joint surface is involved — unicompartmental knee arthroplasty may allow for native joint mechanics to be conserved better than with total knee replacement in selected patients. Consideration has to be given to increased risk of revision in the younger patient, as registry data from Australia and Sweden show that patients younger than 55 years are at significantly higher risk.54 In the literature, estimated survival for unicompartmental knee arthroplasty is reported to be 93% at 10 years and 89% at 15 years.55 Return to sport and physical activity is higher with unicompartmental knee arthroplasty than with total knee replacement, with reported rates in the literature from 36% to 89% after total knee replacement and from 75% to > 100% (i.e., that more patients participated in sports postoperatively than preoperatively) after unicompartmental knee arthroplasty. 56 Results of total knee replacement following unicompartmental knee arthroplasty in the literature are slightly poorer than primary total knee arthroplasty.57
Total knee replacement
Total knee replacement is often the definitive treatment for end-stage osteoarthritis after nonoperative treatment has been exhausted, and recent high-quality evidence has shown that total knee replacement is effective in reducing pain and improving function.58 Increasingly, total knee replacement is being done in patients younger than 60 years. Implant survival is affected by patient factors such as activity level, bone quality and age, as well as implant factors such as bearing surfaces and fixation method.59 Although cementless techniques have been proposed along with alternative bearings surfaces, no high-quality randomized studies have yet shown the improvements of such techniques over current arthroplasty methods.60
What treatments are not supported by evidence?
For some treatments, available evidence shows no effect, or even harm.
Across most guidelines, nutritional supplements, including glucosamine and chondroitin, which were thought to be promising, are either not recommended, or it is acknowledged that the evidence supporting their use is not sufficient to make recommendations (Table 1). However, a recent RCT evaluating 800 mg/day pharmaceutical-grade chondroitin sulphate compared with celecoxib and placebo in more than 600 patients found chondroitin to be similar to celecoxib and superior to placebo in reducing pain and improving function, with low risk for adverse events.61 Nutraceutical- grade chondroitin, however, has been shown to be ineffective in numerous studies, likely owing to variations in preparation, composition and purity. Primary care physicians may consider the use of oral pharmaceutical-grade chondroitin sulphate in the treatment of knee osteoarthritis.
Acupuncture, transcutaneous electrical nerve conduction, knee tape,62 lateral wedge insoles63 and naturopathic or homeopathy alternatives are commonly used nonpharmacologic approaches that are not supported by evidence.
Acetaminophen is widely available and often used, given its presumed safety profile and low cost. Clinical guideline recommendations regarding its use are variable, and results from a network meta-analysis comparing various nonoperative treatments found acetaminophen to be one of the least efficacious treatment options (effect size 0.18, 95% CI 0.04 to 0.33).64
Surgical management of the degenerative knee by means of arthroscopic lavage or debridement has been shown to have no clinical benefit compared with nonoperative treatments.65,66 In the case of mechanical symptoms in the absence of osteoarthritic changes in the joint, we suggest considering a referral to an orthopedic specialist for determination of whether arthroscopy is warranted.
How do the various treatments compare?
Comparative effectiveness was previously difficult to discern with traditional meta-analytic methods. Network meta-analysis, however, has allowed for multiple comparisons by using direct evidence from comparative studies as well as indirect evidence from comparisons of treatments with a common reference.67 A network meta-analysis of 137 RCTs compared the effectiveness of nonoperative treatments, including oral and intra-articular placebo, intra-articular corticosteroids and hyaluronic acid, as well as various oral pain medications.64 Oral naproxen, ibuprofen and diclofenac were superior to acetaminophen, and diclofenac had the greatest effect size of comparators taken orally. A critical finding from the study is that intra-articular treatment options (corticosteroids and hyaluronic acid) were more effective for pain relief than oral agents, with hyaluronic acid the most efficacious with respect to both pain and function (effect size 0.63, 95% credible interval [CrI] 0.39 to 0.88). This analysis further clarified the placebo effect of an intra-articular injection and reported that none of the nonsteroidal anti-inflammatory drugs taken orally had treatment effects greater than an intraarticular placebo.64
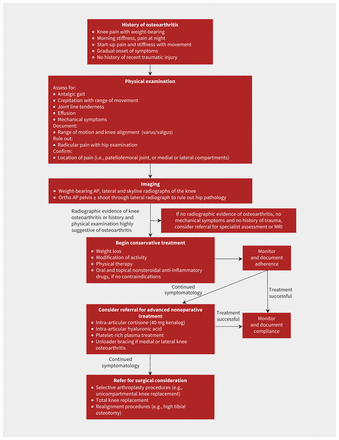
Figure 1 shows a suggested algorithm for conservative management of knee osteoarthritis.
Suggested algorithm for conservative management of knee osteoarthritis. Note: AP = anteroposterior, MRI = magnetic resonance imaging.
What are the emerging therapies?
The market for newer biological treatments for osteoarthritis is growing rapidly and corresponds to an exponential increase in the number of publications on such treatments. More than 80 RCTs and 23 systematic reviews have evaluated platelet-rich plasma, with more than 30% of these published in the last two years. Platelet-rich plasma is autologous blood with supraphysiologic concentrations of platelets containing bioactive proteins and growth factors to promote the body’s healing process. Use of platelet-rich plasma in knee osteoarthritis was evaluated in a recent meta-analysis of 10 RCTs, which found that intra-articular injection of platelet-rich plasma was associated with significant improvements in pain and functional outcomes compared with hyaluronic acid or saline injections.68 However, there is substantial heterogeneity among RCTs with regard to platelet and leukocyte concentration, use of activating agents and growth factor concentrations, the role of which will need to be clarified by future research. Notwithstanding, the market for platelet-rich plasma is expected to surpass US$451 million annually by 2024.69 Biological interventions such as platelet-rich plasma may play a larger role in managing the treatment of young patients with osteoarthritis. Future large RCTs are needed to answer critical questions regarding indications and composition of such treatments.
There is growing interest in the possibility of using stem cell– based treatments for knee osteoarthritis. A systematic review of randomized and observational studies concluded that although results from the available literature supported decreased pain scores and improved functional outcomes, no high level of evidence for stem cell therapy in the treatment of patients is currently available.70
Research into novel pathways for pain management and opioid avoidance continues with evaluating the potential role for cannabis-based medications. Future treatment options may also include biologic modulators of the Wnt pathway, which is implicated in the pathophysiology of osteoarthritis. Early clinical trials of such agents are underway, looking at whether they decrease or reverse the rate of cartilage breakdown (NCT03122860).71 Questions for future research are summarized in Box 2.
Unanswered questions
What is the comparative effectiveness of upcoming knee injectables?
What specific formulation of platelet-rich plasma shows efficacy in knee osteoarthritis?
What role do stem cell injections play in the knee?
What is the comparative effectiveness of platelet-rich plasma and stem cells?
What is the optimal combination treatment for knee osteoarthritis?
What is the role of cannabinoids in knee osteoarthritis?
What about a multimodal approach to treatment?
Guidelines rarely recommend a multimodal approach to treatment, and treatment options are often presented according to best evidence or level of invasiveness, as if they should be used in sequence. In reality, patients often use many treatments in parallel. The additive, or synergistic, effects of multimodal therapies for knee osteoarthritis are largely unknown and understudied. Patients may meet with a number of physicians and allied health professionals when seeking care for osteoarthritic symptoms. We suggest that a multidisciplinary approach or comprehensive multimodal approach to managing symptoms of knee osteoarthritis through physical therapy, lifestyle modifications and pharmacologic treatments is most sensible. As guidelines are updated, clear comparative analyses of the relative value of single and multimodal approaches should be undertaken.
Footnotes
Competing interests: Mohit Bhandari reports research grants from Sanofi, Pendopharm, Ferring and DJO, outside the submitted work. Mitchell Winemaker reports personal fees and nonfinancial support from Stryker Canada, outside the submitted work. No other competing interests were declared.
This article has been peer reviewed.
Contributors: All of the authors contributed to the conception and design of the work, drafted the manuscript, revised it critically for important intellectual content, gave final approval of the version to be published and agreed to be accountable for all aspects of the work.