Abstract
Background: There has been little systematic investigation of widespread reports of drugging and sexual assault. We sought to determine the prevalence of and factors associated with suspected drug-facilitated sexual assault.
Methods: Between June 2005 and March 2007, a total of 977 consecutive sexual assault victims underwent screening for suspected drugging at 7 hospital-based sexual assault treatment centres. We defined victims of drug-facilitated sexual assault as those who presented to a centre within about 72 hours of being assaulted and who provided at least 1 valid reason for suspecting that she or he had been drugged and sexually assaulted. We used logistic regression modelling to compare victims of suspected drug-facilitated sexual assault with other sexual assault victims, controlling for covariates.
Results: In total, 882 victims were eligible for inclusion in the study. Of these, 855 (96.9%) were women, and 184 (20.9%) met the criteria for suspected drug-facilitated sexual assault. Compared with other victims, victims of drug-facilitated sexual assault were more likely to have presented to a large urban centre for care (odds ratio [OR] 2.31, 95% confidence interval [CI] 1.47–3.65), to be employed (OR 1.92, 95% CI 1.34–2.76), to have consumed over-the-counter medications (OR 3.97, 95% CI 2.47–6.38) and street drugs (OR 1.71, 95% CI 1.12–2.62) in the 72 hours before being examined and to have used alcohol before the assault (OR 4.00, 95% CI 2.53–6.32).
Interpretation: Suspected drug-facilitated sexual assault is a common problem. Sexual assault services should be tailored to meet the needs of those experiencing this type of victimization.
Since the mid-1990s, there has been a growing number of unconfirmed reports of assailants surreptitiously using prescription and nonprescription drugs to induce disinhibition, sedation and amnesia to facilitate rape.1 This type of victimization is most commonly referred to as drug-facilitated sexual assault. Although flunitrazepam, in particular, has been maligned as a “date rape drug,”2 many other easily accessible substances have reportedly been used to facilitate sexual assault, including alcohol and alprazolam, chloral hydrate, gamma-hydroxybutyrate, ketamine, lorazepam, ziploclone and zolpidem.1,3
Few studies have systematically measured the occurrence of drug-facilitated sexual assault. Because there is no agreed-upon definition of the phenomenon,4 comparisons across studies are difficult. In a large population-based telephone survey focused on rape in the United States, 2.3% of adult women reported that they had been deliberately incapacitated with drugs or alcohol and sexually assaulted.5 According to the 2001 British Crime Survey, among adult female victims of rape, 5.0% reported that they had been “drugged in some way.”6 Rates of suspected drug-facilitated sexual assault derived from chart reviews of sexual assault victims presenting to specialized sexual assault services have ranged from 6.3% to 17.5%.1,7–9 One such study demonstrated that the incidence of hospital-reported drug-facilitated sexual assault had shown a marked and continuing increase since 1999.10
Little is known about the victims of drug-facilitated sexual assault and how they may differ from victims of other forms of sexual assault.1,5 In a retrospective analysis of sexual assaults in the city of Vancouver, British Columbia, McGregor and colleagues1 found that, compared with other victims, those who suspected that they had been drugged waited longer before presenting to a hospital sexual assault service. In addition, this group had a lower occurrence of genital and extragenital injuries. Women aged 15–19 years had the highest risk of experiencing this type of sexual assault.10 Testa and colleagues,11 working in the United States, compared 48 incidents of rape while incapacitated with 65 other rape incidents. They found that rapes involving incapacitation were less likely than other types of rape to result in injury and were also less likely to involve a perpetrator with whom the victim had had previous sexual intercourse. Rapes involving incapacitation were more likely to have occurred following time spent in a bar or at a party and were more likely to involve higher levels of drinking and self-reported intoxication.
This study had 2 goals: to determine the proportion of sexual assault victims who suspected that they had been covertly drugged, and to determine whether and how victims of drug-facilitated sexual assault differed from other victims of sexual assault.
Methods
Setting
In 2004, we recruited 7 of the 34 hospital-based treatment centers for sexual assault and domestic violence in Ontario. These centres were selected because they served both rural and urban areas of the province and people representing Ontario's culturally diverse population. Nurses and physicians provided on-call services 24 hours a day, 7 days a week, to victims, who generally presented within 72 hours of being assaulted. Services included crisis intervention, physical assessment and treatment of injuries, collection of medicolegal evidence, prophylactic medication for pregnancy and sexually transmitted infections, and referral to counselling and community agencies for ongoing support.
We received ethics approval for our study from the research ethics board of Sunnybrook and Women's College Health Sciences Centre and from each of the other participating sites.
Definitions
We chose the Delphi method,12 a systematic, iterative means of determining the parameters of a phenomenon, to generate key criteria for suspected drug-facilitated sexual assault. Using the Delphi method, an advisory committee, which comprised 2 toxicologists, a forensic biologist, a physician sexual assault examiner and the program coordinators from the 7 participating sites, aided in identifying 16 symptoms that might be associated with suspected drugging (Table 1). We classified cases of suspected drug-facilitated sexual assault as those in which the person reported a suspicion of having been drugged in combination with at least 1 of the 16 associated symptoms, gave a valid reason for believing that a sexual assault had occurred (Table 1) and presented within about 72 hours of being assaulted.
Table 1.
Data collection
We created a screening form to gather information about the participants. Staff members at an eighth sexual assault and domestic violence treatment centre piloted the form for 3 weeks. We revised the form on the basis of their feedback. The final version of the form included the list of valid reasons that would support a person's belief that she or he had been sexually assaulted and the list of symptoms associated with a suspicion of having been drugged. It also contained 19 other items in 5 brief sections: victim information, assault history, alcohol use, drug use and time frame (Appendix 1, available at www.cmaj.ca/cgi/content/full/180/5/513/DC2).
In May 2005, we trained 5 site coordinators by videoconference using a “train-the-trainer” model. During this session, we presented information about drug-facilitated sexual assault and the goals, procedures and inclusion criteria of the study. We introduced the screening form and explained how to complete it. We asked the 5 site coordinators to train staff members at their own sites. In January 2006, we provided in-person training to all available staff members at the remaining 2 sites.
For each consecutive person who presented to a participating site between June 2005 and March 2007, the attending health care provider completed the screening form. We asked site coordinators to fill in missing information, when it was possible to do so, and to return the forms to the study coordinator (N.R.), who reviewed them for completeness and participant eligibility. We entered the data from the forms into a database on a biweekly basis.
Statistical analysis
We examined variables pertaining to the location of the service; the date and the victim's time of arrival at the centre, as well as her or his sociodemographic characteristics (e.g., age, sex), health history (physical and mental health problems) and voluntary use of substances (over-the-counter medications, prescription medications, street drugs) in the previous 72 hours; and the assault (e.g., type of assault, presence of a weapon) (Table 2).
Table 2.
We first described the sample characteristics using descriptive statistics: frequency counts and percentages for categorical variables and means and standard deviations (SD) for continuous data. Next, we compared victims of suspected drug-facilitated sexual assault and victims of other types of sexual assault using χ2 tests with cross-tabulation or the Fisher exact test when cell sizes were small. Finally, to determine what factors, if any, were associated with drug-facilitated sexual assaults, we entered variables that were significant at p < 0.10 in the bivariate analyses into a multivariable model using logistic regression. We entered age as a continuous variable. We classified time from assault to presentation as less than or equal to 24 hours or greater than 24 hours. We reclassified the location of service as large urban centre or other (suburb, smaller city, town, rural area). We examined all variables for multicollinearity. We used the Hosmer–Lemeshow goodness-of-fit statistic to check the fit of the model. We defined p values of 0.05 or below as statistically significant. We report the findings as odds ratios (ORs) with 95% confidence intervals (CIs).
Because of substantial missing data, we did not enter into the multivariable model 3 variables that were significant in the bivariate analyses: kissing or fondling, cunnilingus or fellatio, and presence of a weapon. To assess the effect of missing data on the remaining factors, we ran models with missing values set to “no,” with missing values set to “yes,” and with missing values left out. The results of these analyses were essentially the same, and we present here the model with missing values set to “no.”
Results
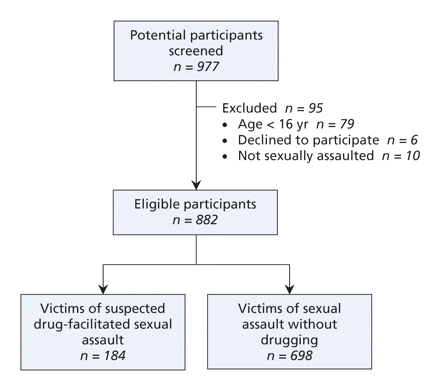
The centres recorded a total of 977 consecutive sexual assault victims during the study period. Some persons were ineligible for inclusion in the study because they declined to participate (n = 6), did not suspect that they had been sexually assaulted (n = 10) or were younger than 16 years of age (n = 79) (Figure 1). Of the 882 (90.3%) eligible participants, most (466/706, 66.0%) were screened within 24 hours of the (suspected) assault. Participants ranged in age from 16 to 91 years (mean 27.2 years, SD 10.2 years) and the majority were female (855/882, 96.9%). Just under half were employed (390/826, 47.2%) and two-fifths were living with family (344/837, 41.1%). About one-third stated that they were students (286/805, 35.5%) and reported having mental health problems (e.g., depression, anxiety) (255/801, 31.8%). A small proportion (91/838, 10.9%) had physical or cognitive disabilities (e.g., intellectual delay, epilepsy, attention deficit disorder).
Figure 1: Screening of sexual assault victims for suspected drug-facilitated sexual assault.
According to the self-reported data, in the 72 hours before being examined, 12.3% (101/819) of the participants had consumed over-the-counter medications (e.g., analgesics, antiemetics), 32.8% (268/816) had consumed prescription medications (e.g., antidepressants, tranquilizers), and 21.4% (174/814) had consumed street drugs (e.g., marijuana, crack, cocaine, ecstasy). Nearly two-thirds (548/845, 64.9%) reported using alcohol immediately before the (suspected) assault. Almost half (404/848, 47.6%) of the (suspected) assaults took place between Friday and Sunday. Kissing or fondling reportedly occurred in 70.5% (353/501) of cases, cunnilingus or fellatio in 32.4% (145/447), and vaginal or anal penetration in 93.7% (563/601). Weapons were present in 7.2% (49/682) of cases. Almost two-fifths of victims (298/773, 38.6%) sustained a genital or extragenital injury.
Overall, 184 (20.9%) of the 882 eligible cases were deemed to represent suspected drug-facilitated sexual assault (Figure 1). Several factors differentiated the victims in these cases from the victims of other types of sexual assault (Table 2). More victims of suspected drug-facilitated sexual assault were employed and were students. A greater proportion had used over-the-counter medications and street drugs in the 72 hours before being examined, consumed alcohol immediately before being assaulted, been subjected to kissing or fondling and cunnilingus or fellatio, and had sustained physical injuries. Fewer victims of suspected drug-facilitated sexual assault reported mental health problems, physical or cognitive disabilities, and the presence of a weapon during the assault. Other factors that differed between the 2 groups were location of service, time to presentation and age.
Several variables retained significance in the multivariable model (Table 3; Appendix 2, available at www.cmaj.ca/cgi/content/full/180/5/513/DC2). Victims of suspected drug-facilitated sexual assault were more likely than victims of other types of sexual assault to have been seen at a large urban centre (OR 2.31, 95% CI 1.47–3.65) and were more likely to be employed (OR 1.92, 95% CI 1.34–2.76). They were also more likely to have consumed over-the-counter medications (OR 3.97, 95% CI 2.47–6.38) and street drugs (OR 1.71, 95% CI 1.12–2.62) in the 72 hours before being examined and to have been drinking alcohol immediately before being assaulted (OR 4.00, 95% CI 2.53–6.32).
Table 3.
Interpretation
Of the 882 eligible victims screened in this study, 184 (20.9%) met the criteria for suspected drug-facilitated sexual assault. Factors associated with this type of assault were location of service, employment status and use of over-the-counter medications, street drugs and alcohol.
The rate of suspected drugging in this study was higher than that reported in chart reviews of cases of sexual assault from similar specialized services in Victoria, Australia (17.5%),7 Vancouver, Canada (12.1%),1 Paris, France (6.3%),8 and Minneapolis, United States (7.0%).9 This difference may be related to the systematic and prospective collection of data in our study, our definition of drug-facilitated sexual assault and the year of our study. McGregor and colleagues1 found that the proportion of cases in which drugging was suspected had more than doubled, to 23% in 1999, over the previous 6 years.
In our study, victims who reported a suspicion of being drugged were more than 2 times more likely than other victims of other types of sexual assault to have presented to a large urban centre. This result may not be surprising, given that “date rape drugs” may be more easily obtained in larger cities. Victims of suspected drugging were also almost 2 times more likely to be employed. Gee and colleagues13 found that the most commonly reported locations for contact with an assailant immediately before being drugged and sexually assaulted were pubs and clubs, establishments where disposable income is required to buy drinks.
In fact, in our study, victims of suspected drug-facilitated sexual assault were 4 times more likely than victims of other types of sexual assault to report drinking alcohol immediately before being assaulted. In 2 population-based surveys examining the occurrence of sexual assault, drug-assisted rapes and rapes occurring while the victim was incapacitated were also more likely than other forcible rapes to have involved the voluntary use of alcohol,5 as well as the consumption of a greater number of drinks and higher rates of intoxication.11
Victims of suspected drug-facilitated sexual assault in our study were also more likely to have consumed over-the-counter medications and street drugs in the previous 72 hours. These types of substances have pharmacologic properties that can alter states of consciousness and lower inhibitions, especially when used simultaneously with alcohol,11,14,15 and in their own right may be used to spike drinks.16 As such, victims could have unwittingly ingested a “date rape drug.” Testa and colleagues11 also found that rape victims who were incapacitated were more likely than victims of forcible rape to have used drugs before being assaulted. Street drugs are not controlled and thus may contain any number of substances. They are used in pubs and nightclubs and at house parties,17 venues where assailants often seek out victims and perpetrate drug-facilitated sexual assault.13,18
It is possible that not all victims of suspected drug-facilitated sexual assault in our study experienced surreptitious drugging. The voluntary use of alcohol, over-the-counter medications and street drugs, alone or in combination, could have resulted in incapacitation.7,11,13,14,19,20 Although false negatives are possible, Hurley and colleagues7 reported that in only 20% of suspected cases of drug-facilitated sexual assault was a drug found on toxicologic screening that the victim had not voluntarily consumed; this figure was 2% in a study by Scott-Ham and Burton.14 Horvath and Brown18 noted that men may prey on intoxicated women because they are “easy targets.” Horvath and Brown, as well as Gee and colleagues,13 described this type of drug-facilitated sexual assault as “opportunistic.”19
Limitations
This study had limitations. First, the results can be generalized only to cases reported to specialized sexual assault services, which may represent only a fraction of the rapes in the community. In a US survey of 3001 women, Kilpatrick and colleagues5 found that only about one-fifth of those who reported having been sexually assaulted had received post-rape medical care. Thus, our study may represent the tip of the iceberg with regard to this issue. Second, it is possible that we did not collect some key information that might have further differentiated victims of suspected drug-facilitated sexual assault from victims of other types of sexual assault (e.g., victim's relationship to the assailant, activity immediately before the assault) or that might have aided in interpreting the results (e.g., whether assailant plied the victim with alcohol, amount of alcohol consumed). Finally, as might be expected, given that many victims reported amnesia of the event, substantial data were missing for some variables (e.g., type of sex acts perpetrated).
Conclusion
Suspected drugging was common in a sample of people attending sexual assault and domestic violence treatment centres. Providing access to hospital-based toxicologic screening services with the sensitivity to detect “date rape drugs” would help to meet the needs of victims of drug-facilitated sexual assault. At the same time, given that suspected drug-facilitated sexual assault is associated with victims' voluntary substance use, it is imperative that we increase awareness of the effects of using alcohol, particularly in combination with prescription, over-the-counter and street drugs, through public awareness campaigns, including posting information at clubs, pubs, bars, university and college campuses, and community health centres.7,13,20 We also need to educate men that a woman who is intoxicated is incapable of consenting to sexual contact and that using alcohol or drugs (or both) to incapacitate a woman for the purposes of sex represents sexual assault.
@@ See related commentary by Butler and Welch, page 493
Footnotes
-
Une version française de ce résumé est disponible à l'adresse www.cmaj.ca/cgi/content/full/180/5/513/DC1
Funding: This study was funded by a peer-reviewed grant from the Ontario Women's Health Council, Ministry of Health and Long-Term Care, Ontario. Janice Du Mont is the recipient of a New Investigator Award in Gender and Health from the Canadian Institutes of Health Research and is supported by the Atkinson Foundation.
This article has been peer reviewed.
Contributors: Janice Du Mont contributed to the concept and design of the study and to the acquisition, analysis and interpretation of data, and she wrote the first draft of the manuscript. Sheila Macdonald contributed to the concept and design of the study and to the acquisition and interpretation of the data, and she read and revised drafts of the manuscript. Nomi Rotbard coordinated the acquisition of data, aided in the cleaning and interpretation of the data, and she read and revised drafts of the manuscript. Eriola Asllani was responsible for entering, cleaning and running the data, and she read and revised drafts of the manuscript. Deidre Bainbridge contributed to the concept and design of the study and the interpretation of the data, and she read and revised drafts of the manuscript. Marsha Cohen contributed to the concept and design of the study and to the acquisition, analysis and interpretation of data, and she read and revised drafts of the manuscript. All authors gave approval of the manuscript submitted for publication.
Acknowledgements: We thank the sexual assault nurses, physicians and program coordinators at the participating sites, and the project advisory committee.
The study received ethics approval from the research ethics boards of the 7 participating hospitals: Women's College Hospital; Scarborough Hospital, Grace Division; Renfrew Victoria Hospital; Lake of the Woods District Hospital; Guelph General Hospital; Hamilton Health Sciences, McMaster University Medical Centre; and the Ottawa Hospital Civic Campus.
Competing interests: Marsha Cohen, a coauthor of this article, is an associate editor of CMAJ. She was not involved in the selection of peer reviewers for this article or the vetting of the manuscript before its acceptance. None declared for Janice Du Mont, Sheila Macdonald, Nomi Rotbard, Eriola Asllani and Deidre Bainbridge.