- © 2007 Canadian Medical Association
What's your call?

CT scan (left) and chest radiograph (right) of a 37-year-old homeless man whose pulmonary tuberculosis had been treated in hospital 5 months before presentation. He returned to hospital after losing 5 kg. Over the preceding 2 months, he had experienced anorexia, low-grade intermittent fevers and a productive cough.
This 37-year-old man who was homeless was admitted to hospital and treated for pulmonary tuberculosis. Five months later, the patient returned to hospital with a 5-kg weight loss and a 2-month history of anorexia, low-grade intermittent fevers and a productive cough.
A preliminary chest radiograph revealed marked volume loss within the patient's left lung secondary to pleuroparenchymal fibrosis with upward retraction of the left hilar structures and apical pleural thickening. Within the left upper lobe there was a large cavity. A loculated left pleural effusion was also visible. Many poorly defined nodules lay within his right lung, mostly in the upper lobe. Follow-up 4-mm unenhanced coronal CT maximum-intensity projection images confirmed the presence of centrilobular nodules, primarily involving the right upper lobe and left lower lobe of the lung (Figure 1), with a “tree-in-bud” appearance that is nonspecific but consistent with endobronchial tuberculosis.
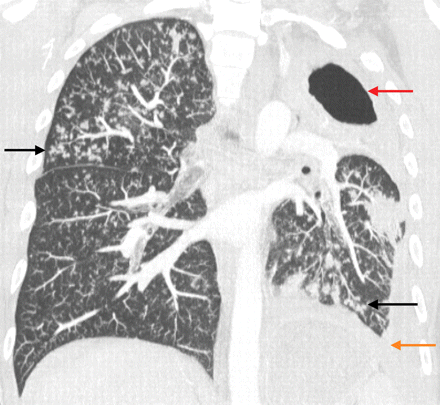
Figure 1: A 4-mm coronal CT maximum intensity projection image. The black arrows point to nodules in the right upper and left lower lobes of the lungs, with a “tree-in-bud” appearance due to small airway spread of tuberculous infection. The large left upper lobe cavity (red arrow) is the hallmark of postprimary tuberculosis. The accompanying loculated left-sided tuberculous empyema (orange arrow) was subsequently drained percutaneously.
The cavity in the left upper lobe suggested that the inflammatory process was extending into adjacent airways. The left-sided tuberculous empyema was drained by insertion of a pigtail catheter. The diffuse pleural thickening in the left upper hemithorax (Appendix 1; available online at www.cmaj.ca/cgi/content/full/177/2/148/DC1) was most likely secondary to prior pleural infection. Sputum cultures and a pleural smear confirmed the presence of Mycobacterium tuberculosis. The patient responded well to treatment with antitubercular medications.
Postprimary pulmonary tuberculosis (also called reactivation tuberculosis) develops in 5%–20% of patients infected with M. tuberculosis. Found mainly in adults, this form of tuberculosis arises from the reactivation of bacilli that lay dormant within a fibrotic area of the lung.1,2 In adults, reinfection with a strain of mycobacterium that differs from that which caused the primary infection is also possible. Predisposing factors include immunosuppression, diabetes, malnutrition and alcoholism.
Postprimary tuberculosis manifests radiographically as focal or patchy parenchymal opacities, mainly in the apical and posterior segments of the upper lobes and the superior segments of the lower lobes. Cavitation from active infection is the hallmark of this form of tuberculosis, seen in up to 50% of cases. High-resolution CT is more sensitive than radiography in defining small cavities and in distinguishing them from cystic bronchiectasis or paracicatricial emphysema. The CT finding of tree-in-bud nodules, also a marker for disease activity, represents endobronchial spread of the disease. These nodules, which are usually poorly defined, with a segmental or lobar distribution, are secondary to caseation necrosis and granulomatous inflammation filling and engulfing the terminal bronchioles. Mediastinal or hilar lym phadenopathy occurs in up to 10% of cases; pleural effusions, up to 25%.
Computed tomography is superior to radiography in the diagnosis of tracheobronchial tuberculosis. CT plays an important role in delineating findings that may imply disease activity (e.g., cavitation or endobronchial involvement), thereby expediting therapy for patients who pose a public health risk. Endobronchial tuberculosis should be distinguished from miliary or hematogenous dissemination, in which the nodules are more sharply defined and randomly distributed throughout the lungs.
Footnotes
-
This article has been peer reviewed.
Competing interests: None declared.