As of Oct. 29, 2003, Nigeria gained the dubious honour of having the highest number of reported cases of polio (217 new cases) in the world, surpassing the previous leader, India.1 The resurgence of poliomyelitis in northern Nigeria poses a threat to neighbouring countries and further postpones the goal of the World Health Organization (WHO) to eradicate the disease globally. This is by no means an impossible goal: humans are the only natural reservoir, an inexpensive and effective vaccine is available, immunity is life-long, and the virus can survive for only a very short time outside the human host.
Figure. Refugees from the Democratic Republic of the Congo with Red Cross health cards and meal vouchers. Lugufu Refugee Camp, Western Tanzania, March 2003. Photo by: Dr. Valerie F. Krym
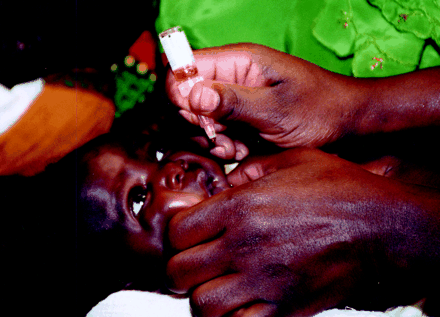
Figure. Administration of oral polio vaccine to a refugee from Burundi. Mtendali Refugee Camp, Western Tanzania, March 2003. Photo by: Dr. Valerie F. Krym
Prevention and immunity
Immunity to poliovirus is type specific. A trivalent live attenuated oral vaccine and a trivalent inactivated injectable vaccine are available. The oral vaccine induces a mucosal immunity that inhibits replication of the virus in the small intestine, thereby reducing shedding of the virus in feces and decreasing transmission. In areas where fecal–oral transmission is the most frequent route of transmission, the oral vaccine is the vaccine of choice. It is, however, associated with rare cases of vaccine-derived paralytic poliomyelitis.2,3 In addition, the live attenuated virus is shed mainly in feces, and its circulation in poorly immunized populations may result in mutated poliovirus strains with virulence similar to that of the wild virus.2
The injectable inactivated vaccine, in addition to providing mucosal immunity in the small intestine, also stimulates production of circulating antibodies that stop the virus from spreading to the central nervous system.
Global eradication
In 1988 the WHO launched a global initiative to eradicate polio by the year 2000. At that time, less than half the world's children had received 3 doses of the oral polio vaccine, and more than 350 000 new cases of polio were estimated to have been reported in 125 countries.3
By 2001 the number of polio-endemic countries was down to 10, and the annual number of new cases was less than 500. In 2002, however, the number of cases increased to 1920, in large part because of decreased immunization efforts in some states in India. Despite India launching its largest-ever national campaign to eradicate polio, its recent polio outbreak has yet to be contained. As of Oct. 28, 2003, there were 477 cases of confirmed polio in 7 endemic countries.4
The global effort to eradicate polio, now in its 15th year, has led to more than 600 million children being vaccinated. To date, the WHO has certified 3 regions as “polio-free”: the Americas, the Western Pacific and the European regions.
In countries without well-established, routinely implemented national immunization programs, symptomatic and asymptomatic polio is best eradicated by the use of National and Sub-National Immunization Days. With this type of strategy, 2 doses of oral polio vaccine are given to all children under the age of 5 years, regardless of their vaccination history, over several days. For example, over the course of 6 days in 2003, 1.3 million volunteers and health care workers in India administered nearly 200 million doses of vaccine to more than 165 million children under the age of 5.
In addition to national and subnational immunization days, it is important to develop and maintain surveillance activities to identify and confirm any new cases of infection with wild poliovirus. If polio is detected, supplemental or “mop-up” campaigns provide intense immunization coverage in focal areas identified by surveillance.
To be effective, immunization programs in non-outbreak settings must cover at least 80% of the population. They must reach at least 90%–95% of children under 5 years of age, and there must be no pockets of children with lower coverage rates. Finally, there must be an adequate surveillance system to identify new cases.
To augment the eradication effort, the US Centers for Disease Control and Prevention established the Stop Transmission of Polio (STOP) program in 1998 in partnership with the WHO, Rotary International and UNICEF. Teams of international consultants are sent to polio-endemic areas to support national immunization programs, assist with disease surveillance and case-finding, and help contain local outbreaks (one of us [V.F.K.] served for 3 months as a Canadian representative on STOP Team 12 in Tanzania). Health care workers interested in participating in polio eradication programs can consult the Web sites of the Canadian Public Health Association (www.cpha.ca/english/intprog/CIII/contents.htm) or the STOP program (www.cdc.gov/nip/global/stopteam.htm).
Despite the multi-billion dollar cost, it is estimated that polio eradication strategies will save US$128 billion and prevent 855 000 deaths, 4 million cases of paralysis and 40 million disability-adjusted life-years during the period 1970–2050.5 Unfortunately, funding for the immunization programs is uncertain. The financial shortfall for 2003–2005, partly a result of the global economic slowdown, has resulted in a lack of resources for supplemental immunization activities in some countries. Recent donations, including one from Canada of US$13.9 million over 3 years for Nigeria, may well result in the eradication of polio worldwide. If so, it will be only the second time in history that a communicable disease has been eradicated.
Valerie F. Krym Stop Transmission of Polio (STOP) Program World Health Organization Dar Es Salaam, Tanzania Centre for International Health Faculty of Medicine University of Toronto Toronto, Ont. Russell D. MacDonald Division of Emergency Medicine Department of Medicine University of Toronto Toronto, Ont.
-
Caused by an enterovirus with 3 serotypes (1, 2* and 3), poliomyelitis is spread mainly by the fecal–oral route. However, where there is good sanitation, the virus may be transmitted in throat secretions, airborne droplets or, in rare instances, milk or other foodstuffs that have been contaminated with feces. Water and sewage are rarely implicated.
-
The poliovirus binds to specific receptors in the oropharynx, tonsils and small intestine. It then may spread to the central nervous system by penetrating the blood–brain barrier or by spreading along nerve fibres. In about 1% of infections (mainly those caused by type 1 poliovirus) motor neurons are destroyed, which results in paralysis of affected muscle groups.
-
The incubation period is 7–14 days. The disease may be inapparent or present as a mild, nonspecific viral illness. Aseptic meningitis or paralytic poliomyelitis is rare. Many people who have subclinical poliomyelitis shed the virus, which results in transmission to others.
-
*Global immunization efforts have stopped the spread of indigenous wild type 2 poliovirus, which was last detected in October 1999.
Poliomyelitis