Abstract
DECOMPRESSION ILLNESS (DCI) CAN OCCUR in a variety of contexts, including scuba diving and flight in nonpressurized aircraft. It is characterized by joint pain, neurologic injury, and respiratory or constitutional symptoms. To prepare flight crews for accidental decompression events, the Canadian Armed Forces regularly conducts controlled and supervised depressurization exercises in specialized chambers. We present the cases of 3 Canadian Armed Forces personnel who successfully completed such decompression exercises but experienced DCI after they took a 3-hour commercial flight 6 hours after the completion of training. All 3 patients were treated in a hyperbaric oxygen chamber. The pathophysiology, diagnosis and management of DCI and the travel implications for military personnel who have undergone such training exercises are discussed. Although DCI is relatively uncommon, physicians may see it and should be aware of its presentation and treatment.
Case
Three previously well male Canadian Armed Forces personnel participated as part of a group of 17 trainees in high-altitude indoctrination (HAI) training over 3 days in Winnipeg (altitude 761 ft [232 m]). In Canada, HAI involves exposure to low pressures in a hypobaric chamber to familiarize personnel with the physical and mental stress of depressurization at high altitudes. Personnel use supplemental oxygen for 30 minutes in chambers at a pressure equal to that at ground level to reduce the nitrogen load in their body tissues. To permit the trainees to experience hypoxia, the chamber is gradually depressurized to about 25 000 ft (7620 m), and the trainees, who are seated, then remove their supplemental oxygen supply and complete simple, repetitive drawing tasks. They replace their oxygen masks anytime they feel or appear unwell. Occasionally, to simulate sudden loss of cabin pressure, chamber pressure can be dropped abruptly from the equivalent of 4000 ft to 18 000 ft (from 1219 m to 5486 m) of altitude. The trainees are then repressurized and gradually returned to the pressure at ground level. As a point of reference, commercial airlines typically pressurize their cabins to the equivalent of 7000–8000 ft (2134–2438 m).
The 3 patients completed 33 minutes at the pressure equivalent of 26 000 ft (7925 m) and 18 minutes at the equivalent of 18 000 ft (5486 m) on the first day. After no training on the second day, they completed 24 minutes at the equivalent of 26 000 ft on the morning of the third day.
About 6 hours after the end of HAI training, the 3 patients boarded a commercial flight from Winnipeg to Vancouver (at sea level). During the flight, which lasted just over 3 hours, patient A experienced knee pain, which became severe and progressed to his hips, back, shoulders, elbows and neck. Patient B noted chest discomfort followed by numbness in his left arm and difficulty breathing. Patient C experienced retrosternal chest pain followed by back pain, headache, shortness of breath and bilateral tingling in his calves; he also had trouble swallowing and speaking for 20 minutes during the flight. Despite their symptoms, the patients took their connecting flight from Vancouver to Comox, BC (at sea level). On arrival, they contacted the physician on call for Canadian Forces Base Comox and were immediately referred to the local community hospital, where decompression illness (DCI) was suspected. The hyperbaric medicine physician in Victoria was consulted by telephone, and treatment was started with oxygen (15 L/min) and intravenously administered saline in all 3 patients. They were then transferred by helicopter to the military hyperbaric unit in Victoria (at sea level, about 220 km away); the pilot was directed to fly below 1000 ft (305 m).
Before entering the hyperbaric chamber, the patients were interviewed and underwent thorough physical examinations. Their physical findings and course are summarized in Table 1. All 3 had normal blood pressure, heart rate and oxygen saturation (while receiving 15 L/min), and normal chest radiograph and electrocardiogram findings. The arterial blood gases were within normal limits in patients B and C; they were not measured in patient A because he did not have respiratory symptoms. Other laboratory investigations (serum levels of creatine kinase, creatine kinase [MB], troponin, glucose, sodium, potassium, chloride, bicarbonate and creatinine, blood urea nitrogen level and complete blood count) gave normal results.
Table 1.
Before entering the hyperbaric chamber the patients had had symptoms for about 91/2 hours. All 3 were symptom free after almost 8 hours of treatment in the chamber (Fig. 1). Patients B and C had no further problems, but patient A had burning respiration, typical of pulmonary oxygen toxicity, from days 2 to 9 after treatment.
Fig. 1: Eight-person hyperbaric chamber. One or more patients are monitored by inside attendant(s) and observed through a window and on video. Communication between patients and the outside chamber takes place by intercom. There is a small portal for passing medicines, food and other necessities. Usual treatment lasts 286 minutes.
Comments
Although DCI is relatively uncommon, physicians may see it and should be aware of its presentation and treatment. DCI following high-altitude exposure is rare but has a presentation similar to that of DCI due to other causes.
Pressure-related injuries arise in a variety of circumstances. Increased pressure stress occurs with diving, compressed-air construction work (e.g., caisson disease),1 work in hyperbaric chambers2 and being in disabled submarines.3 Decreased pressure stress can result from nonpressurized flight, from loss of cabin pressure in pressurized aircraft, with work in hypobaric chambers and with extravehicular activities in space.
Changes in atmospheric pressure have a direct effect on closed gas-filled spaces in the body, with gas volume increasing as pressure decreases. Volume changes result in injuries, such as tympanic membrane rupture, sinus squeeze and pulmonary barotrauma. Pulmonary barotrauma is the result of the volume expansion exceeding the limits of the alveoli. The increase in intra-alveolar pressure either forces air bubbles across the alveolar–capillary membrane or causes rupture of the alveolar wall. This can result in pneumothorax, pneumomediastinum, subcutaneous emphysema, alveolar hemorrhage or arterial gas embolism, which may cause cerebral infarction and injury. Pulmonary or pleural scarring and obstructive airway disease increase the risk of pulmonary barotrauma. Pulmonary barotrauma very rarely results from high- altitude stresses.4
More commonly, reductions in pressure result in dissolved nitrogen coming out of solution and expanding as bubbles in veins and tissues, the injury often referred to as decompression sickness (DCS) or “the bends.” Whereas, increased pressures (e.g., when scuba diving) result in the build-up of nitrogen in tissues, followed by bubble formation on return to lower ambient pressure, altitude DCS results from nitrogen already saturated into tissue at ground level coming out of solution at lower atmospheric pressures.
In this case, because these patients had undergone training in a depressurized environment, nitrogen bubbles would have formed in their blood and tissues during depressurization. The bubbles would have then compressed and gradually returned to solution as the patients were repressurized to a ground-level pressure. However, these patients took a commercial flight soon after completing their training, and the pressure equivalent of 8000 ft (2438 m) on the flight would have immediately expanded any residual bubbles 1.3 times, probably causing their symptoms.5 A similar situation may occur in individuals who fly shortly after scuba diving. Should any residual bubbles be present after a dive, they would similarly undergo expansion during flight causing DCI.
DCI is a “great imitator” and has a wide range of presentations, including dermatologic symptoms, joint pain, neurologic injury, and respiratory or constitutional symptoms, occurring alone or in combination.6,7,8,9,10,11 Musculoskeletal pain is the most common symptom in altitude-induced DCI, being reported in 60%–83% of cases.6,7,9,10 Neurologic symptoms, predominantly headache and paresthesia, occur in 14%–34% of cases.6,7,8,9,10 With most symptoms (50%–77%) the onset occurs on return to ground level; 44%–67% occur within the first 2 hours, and the remainder within 20 hours or longer.6,7,9
Traditionally, DCS is divided into type I and type II. Type I is generally considered to be milder and includes mottling or marbling of the skin, lymphedema and musculoskeletal pain. Type II is generally more severe and can involve the inner ear (“the staggers”), the lungs (“the chokes”) and the CNS. Many diving medicine physicians now classify arterial gas embolism and DCS together as DCI and specify the diagnosis with reference to the type of injury. Our patient A had DCI subtype musculoskeletal/ joint pain, and patients B and C had DCI subtype musculoskeletal/joint pain, neurologic and respiratory.
Most cases of altitude-induced DCI result from HAI training, but flight operations cause up to 10% of cases,6 and the disorder has been reported in private pilots.12Altitude-induced DCI has been reported at altitudes as low as 8000 ft (2438 m),13 but the risk rises substantially between 21 200 and 22 500 ft (6462 to 6858 m) and increases with increasing altitude.14,15 Increased duration or repetition of exposure,14,16,17,18 increased activity at altitude15,17,18 and failure to use supplemental oxygen before exposure14,15,18 all increase the risk considerably. Increased age,19 past injury or surgery20 and flying after altitude exposure21,22 are also known risk factors for DCI. Crowell21 reviewed Canadian Armed Forces HAI training in 1983 and recommended that trainees wait 18–24 hours before flying commercially.
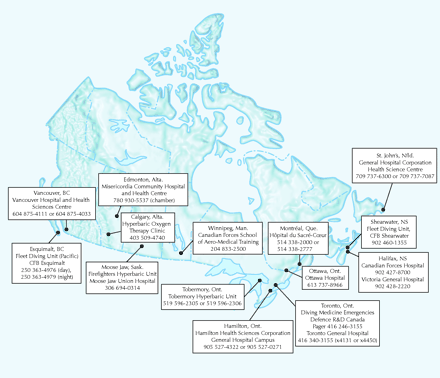
The management of DCI involves hyperbaric oxygen treatment, which is best started as soon as possible because recovery is improved with early treatment.23 Delays in treatment can result from patient uncertainty about the cause of symptoms, patient reluctance to acknowledge injury for fear of career repercussions, and misdiagnosis by medical care providers.23 The distance to the hyperbaric chamber can also be a barrier to expedient treatment (see Fig. 2 for locations of hyperbaric facilities in Canada). Often the most rapid means of transport is by air. It is important to use pressurized aircraft or low- altitude flying to minimize the decrease in pressure, which increases gas bubble size and may worsen symptoms.24,25,26 The altitude of any mountain passes should be considered in ground transportation. Although not commonly used, transportable chambers capable of maintaining 2 atm of pressure may be helpful during transport.27 Oxygen at 100% should always be administered until hyperbaric oxygen treatment can be started.24 As well, dehydration is correlated with pressure-related injury, so fluids should be administered intravenously regardless of reported hydration status. It is prudent to rule out pneumothorax or myocardial infarction in patients with respiratory or cardiovascular symptoms before transport or initiation of hyperbaric oxygen therapy.
Fig. 2: Canadian hyperbaric facilities and diving medicine contact locations.
Research indicates that ground-level oxygen is sufficient for patients free of symptoms or signs on return to ground level and those with complete resolution of symptoms and signs while receiving ground-level oxygen and awaiting hyperbaric oxygen therapy.28,29,30 However, for patients with symptoms that have not resolved on return to ground level or while receiving ground-level oxygen, hyperbaric oxygen therapy remains the preferred treatment.28,29,30,31 Death from altitude-induced DCI was not uncommon before the introduction of hyperbaric oxygen therapy.6 Unfortunately, the latter is not without risk and can result in pulmonary and cerebral oxygen toxicity.31,32 Hyperbaric medicine physicians must be attentive to these conditions.
Although peak rates of 4 cases of DCI in 27 exposures have been reported,33 rates of 1 to 12 cases per 1000 HAI exposures are more common,7,21,34 and the armed forces of most countries accept these risks for the benefits of training. In response to this incident of 3 cases among a class of 17, the Canadian Armed Forces suspended and investigated HAI training. Following the investigation, a policy of no flying for 24 hours after HAI training was instituted. It is hoped that further studies will support training using reduced oxygen concentration to simulate altitude-induced hypoxia without reduction in pressure and the associated risk of DCI.35
-
Always consider the diagnosis of decompression illness (DCI) in situations of changing ambient pressure, such as scuba diving and flight-related illness.
-
DCI is a “great imitator” and can present with varied signs and symptoms (e.g., body pain and dermatologic, neurologic, vestibular or cardiopulmonary symptoms).
-
Early treatment includes 100% oxygen, intravenously administered fluids for rehydration and evacuation (at the lowest possible altitude) to a hyperbaric facility as soon as possible.
-
Know how to contact your nearest available hyperbaric chamber personnel.
Key points
Footnotes
-
This article has been peer reviewed.
Contributors: Both authors participated in assessing and treating the patients. Both made significant contributions to writing the original draft, editing the paper and working on the final submission.
Acknowledgements: We thank Dr. Debbie Pestell and Dr. Cyd Courchesne for their review of the paper and suggestions.
Competing interests: None declared.