Article Figures & Tables
Figures
Fig. 1: A molecular and cellular model for the action of antidepressant treatments and the pathophysiology of stress-related disorders. This model of the hippocampus shows the major cell types in the hippocampus and how stress and antidepressant treatments may influence CA3 pyramidal cells. The 3 major subfields of the hippocampus (CA3 and CA1 pyramidal cells and dentate gyrus granule cells) are connected by the mossy fibre and Schaffer collateral pathways. Recent studies demonstrate that chronic stress decreases the expression of brain-derived neurotrophic factor (BDNF) in the hippocampus. This may contribute to the atrophy or death of neurons in the CA3 pyramidal cell layer of the hippocampus. Long-term elevation of glucocorticoid levels is also known to decrease the survival of these neurons. Other types of neuronal insult, such as hypoxia–ischemia, hypoglycemia, neurotoxins and viral infections, may also cause atrophy or damage of neurons and thereby make a person vulnerable to subsequent insults. These types of interaction may underlie the observations of decreased function and volume of hippocampus in patients with affective disorders and may explain the selective vulnerability of certain people to become depressed. Long-term antidepressant treatments increase the expression of BDNF as well as tyrosine kinase receptor B (trkB) and prevent the down-regulation of BDNF elicited by stress. This may increase the growth or survival of neurons, or help repair or protect neurons from further damage. Increased expression of BDNF and trkB seems to be mediated by the sustained elevation of the serotonin and norepinephrine (NE) systems and the cyclic adenosine monophosphate cascade. Normalization of glucocorticoid levels by long-term antidepressant treatments may also contribute to the recovery of CA3 neurons. (Adapted from Duman et al (22) with permission of the publisher.) Photo: Paulette Dennis
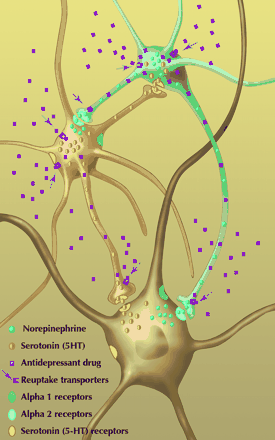
Fig. 2: Schematic of the “cross talk” and purported interactions in the brain between norepinephrine (NE), serotonin (5-HT) and the postsynaptic neurons. (Adapted from Blier (28) with permission of the publisher.) Photo: Paulette Dennis