- © 2007 Canadian Medical Association or its licensors
The case: A 33-year-old woman had received a diagnosis of primary hypothyroidism when she was 23 years of age and had been taking an essentially stable dose of levothyroxine (0.112 mg/d) for at least 2 years. The patient began taking folic acid supplements (1 mg/d) 2 months before a natural, planned conception occurred. About 7 weeks before becoming pregnant, her thyroid stimulating hormone level was 5.95 mU/L, and the levothyroxine dose was increased to 0.116 mg/d. Pregnancy was confirmed by means of a urine home pregnancy test 4 weeks after her last menstrual period. At that time, the patient stopped taking folic acid supplements and, simultaneously with the levothyroxine, began taking prenatal multivitamins that contained iron (ferrous fumarate 60 mg), folic acid (1 mg) and other vitamins and minerals. Her thyroid stimulating hormone level was rechecked 8 weeks after her last menstrual period and was found to be elevated (40.75 mU/L), with a normal free thyroxine level (12.6 pmol/L); thus, the dose of levothyroxine was increased. Throughout her pregnancy, the dose of levothyroxine was adjusted multiple times in response to her thyroid stimulating hormone levels.
An ultrasound performed during week 16 of pregnancy showed live diamnionic, dichorionic fetuses. Labour was induced during week 37, and a vaginal delivery of healthy fraternal twin boys (2910 g and 2530 g) was performed. The patient did not receive levothyroxine therapy for 1 week after the delivery. Post partum, she resumed levothyroxine therapy (0.175 mg/d). On the basis of subsequent thyroid stimulating hormone levels, the levothyroxine dose was reduced to 0.125 mg/d, which resulted in normal thyroid stimulating hormone levels.
Maternal hypothyroidism has been reported to affect as many as 2.5% of pregnancies. Low concentrations of maternal thyroid hormones during early gestation delays neurodevelopment of the fetus and may lead to lower intelligence quotient scores compared with those of age-matched controls.1 It has long been recognized that women with known primary hypothyroidism should have their thyroid stimulating hormone level checked at least once per trimester. The majority of pregnant women who have primary hypothyroidism require additional levothyroxine supplementation to achieve pre-conception thyroid stimulating hormone levels.2,3 This dose increase may be required as early as the fifth week of gestation, which demonstrates the importance of early detection and supplementation during pregnancy. The increased levels of estrogen during pregnancy likely lead to increased levels of thyroxine-binding globulin, which may result in more bound, and less free, triiodothyronine and thyroxine. Thus, the patient is clinically hypothyroid.
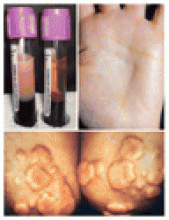
It is quite common for primary hypothyroidism to be diagnosed among women in their child-bearing years, at a time when perinatal vitamin supplementation is often recommended. These supplements typically include, among other ingredients, folate, iron and selenium. However, patients should be cautioned against simulta-neous use of perinatal vitamins and levothyroxine: a clinically significant reduction in levothyroxine efficacy can occur, probably caused by binding of levothyroxine with iron.4 A clinical trial that included 14 patients with primary hypothyroidism reported a greater than 3 times increase in thyroid stimulating hormone levels (from 1.6 mU/L to 5.4 mU/L) after 12 weeks of simulta-neous ferrous sulfate and levothyroxine therapy.4 In vitro, if ferrous sulfate and levothyroxine are mixed, the result is a “poorly soluble purple complex”; this suggests that these drugs form an insoluble complex in the gastrointestinal tract, which thereby reduces the absorption of levothyroxine.
Our case is similar to others that have described the timing and magnitude of the increase in thyroid stimulating hormone levels and the changes in levothyroxine doses required during pregnancy.2,3 In week 8 of pregnancy, our patient had a thyroid stimulating hormone level that was 8 times greater than the level during week 1, and the dose of levothyroxine was increased by 32% (last increase was during week 19). The literature suggests that levothyroxine requirements begin to change during the fifth week of pregnancy and stabilize by week 21. In addition, the magnitude of increase in thyroid stimulating hormone levels is 7–19 times the baseline level, with a corresponding 29%–48% increase in levothyroxine dose requirements. Despite the consistency of our case with other reports, the magnitude of the interaction between perinatal vitamins and levothyroxine therapy is uncertain.
When a patient with primary hypothyroidism is planning a pregnancy, it seems reasonable to proactively implement a plan to avoid exacerbation of the hypothyroidism. Early in the pregnancy, the fetus is completely depen-dent on maternal triiodothyronine and thyroxine. Further, the pharmacodynamic effect of levothyroxine does not manifest until the patient has been taking it for 4–6 weeks. As such, the practical solution offered by Alexander and colleagues seems reasonable:2 upon confirmation of pregnancy, the current dose of levothyroxine should be increased by 29%, or the equivalent of 2 additional doses per week. They suggest that this dose be continued until thyroid function testing is performed. It is prudent that health care providers inform patients of the potential interaction between perinatal vitamins and levothyroxine to avoid any potential reduction in levothyroxine efficacy.
Footnotes
-
This article has been peer reviewed.
Competing interests: None declared.