The Case: A 46-year-old nurse was admitted to the Neurology Department after 6 weeks of recurrent and transient neurologic episodes. She described several episodes of disorientation, language abnormalities and motor weakness, all resolving within an hour. She thought the episodes likely related to long hours of work and decreased sleep; however, she had begun noticing problems with memory and concentration, which prompted her to seek medical attention.
She reported no cardiac, rheumatologic or constitutional symptoms, and her medical and family histories were unremarkable. A nonsmoker and nondrinker, she denied any drug use.
Upon examination, she was afebrile and her vital signs were normal. She was alert and oriented. Head and neck results were normal, including fundoscopy. Cardiac examination revealed a grade 4/6 pansystolic murmur, loudest at the apex. Pulmonary and abdominal exam results were normal. Splinter hemorrhages were noted in both hands. Initial neurologic exam results were normal except for her cognitive tests, which showed some difficulty with naming, concentration and short-term memory. The results of laboratory investigations, including a range of hematologic and rheumatologic tests and a full septic workup, were normal.
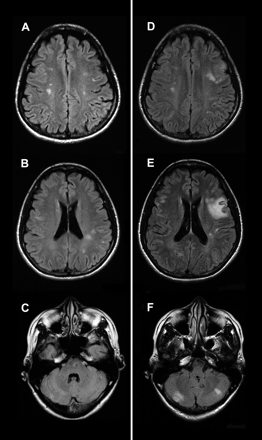
MRIs of the head showed several scattered cortical and subcortical infarcts, including a recent left frontal infarct (Fig. 1). Cerebral angiography did not find evidence of vasculitis.
Fig. 1: MRI scans of the patient.
Chest radiography showed a small density in the right lung. Augmented CT of the chest confirmed a 2.1 × 1.9 cm mass in the right middle lobe and several enlarged subcarinal lymph nodes. A transbronchial biopsy confirmed a stage IIIA adenocarcinoma of the right lung. When quickly seen by the oncology service she was considered, given her high functional status at that time, a candidate for surgery, radiation and possibly chemotherapy.
A transesophageal echocardiogram disclosed a 1.1 × 0.7 cm sessile mass on her mitral valve, thought to be the source of her recurrent embolic strokes. Since the results of her septic workup were negative, nonbacterial thrombotic endocarditis (NBTE) was diagnosed. Staff in both Neurology and Cardiology recommended urgent assessment for cardiovascular surgery for possible mitral-valve replacement.
Soon after admission, however, the patient developed disseminated intravascular coagulopathy (DIC). Despite aggressive intravenous anticoagulation with heparin, plus ASA and clopidogrel, the patient had further, more severe embolic strokes during the week that followed, confirmed with repeat MRI (Fig. 1). These strokes left the patient with pronounced motor and cognitive deficits, including extended periods of confusion and agitation.
Although initially thought to be a candidate for surgery, radiation and chemotherapy for her lung cancer, her rapid clinical deterioration pre-empted any treatment. At the wishes of the patient and her family, compassionate medical management was continued and she was transferred to receive palliative care. She died 1 year later.
NBTE in malignancy was initially described by Ziegler in 1888 and further described by Libman who referred to the process as “terminal type” valve disease or marantic endocarditis.1 The process is thought to be secondary to fibrin– platelet deposition on healthy or degenerating heart valves, often the aortic and mitral valves. This may be related to fibrin or mucin degradation during transit through the lung. Circulating cytokines such as TNF and IL-1 may also play a role in initiating endothelial damage to the heart valves. The presenting symptom is often a stroke.
Malignancy and associated hypercoagulability are often associated with this cytokine release. Autopsy studies have shown that up to 75% of NBTE patients had an underlying malignancy; the actual incidence of NBTE in malignancy has been estimated to be as high as 9%.2 NBTE has been associated with several different malignancies, particularly adenocarcinoma of the lung (Box 1). Retrospective studies have also revealed a strong association with DIC: incidence estimates of NBTE in patients with DIC have been as high as 21%.1
Several problems exist with early diagnosis. NBTE and even DIC are often asymptomatic until major embolic events occur. The malignancy is often advanced by the time of diagnosis, which limits treatment options.
Cardiac abnormalities in NBTE are not always obvious upon examination. An estimated fewer than half of patients have audible murmurs. Furthermore, most lesions are smaller than 5 mm across, which may be too small for routine transthoracic echocardiography. Transesophageal echocardiography is recommended if NBTE is suspected.1
Finally, difficulty lies in distinguishing infective endocarditis (IE) from NBTE, since clues such as fever and positive blood cultures are not always present in IE, and an obvious source of NBTE is often absent. Postmortem observations indicate possible differences between strokes caused by NBTE and IE that could be evident via MRI.2 IE-associated strokes have a variety of MRI patterns, including single cortical strokes, punctate lesions and disseminated patterns, whereas NBTE strokes frequently have multiple disseminated lesions of varying sizes.
Anticoagulation therapy in NBTE is based on the belief that NBTE, like DIC, is part of a continuum of hypercoagulable disorders in malignancy. Heparin is the preferred agent: recurrence of thromboembolic events has been reported in patients with malignancy and DIC when heparin was discontinued.3 Warfarin therapy has not been shown to benefit these patients and is not recommended. Unfortunately, treatment with anticoagulants is often insufficient because it fails to address valve vegetation, the persisting risk factor for recurrent strokes.
Black4 described the use of urgent valve replacement and long-term heparin therapy to treat a young woman's rectal cancer and NBTE. In that case, successful control of thromboembolic complications permitted timely treatment of the underlying malignancy. Urgent valve repair or replacement in addition to long-term anticoagulation should be considered more often, particularly when the prognosis of the underlying malignancy offers the possibility of more than just palliative care. Early mitral valve replacement may have prevented the recurrent strokes that caused our patient's rapid decline and denied her the possibility of treatment for her malignancy. Unfortunately, the delay in presentation and rapid disease progression prevented timely intervention.
Footnotes
-
This article has been peer reviewed.
Acknowledgements: We thank Maher Saqqur, Tom Jeerakathil and Glen Jickling for their assistance, with special thanks to the Divisions of Cardiology and Hematology at the University of Alberta Hospital, and the Division of Oncology at the Cross Cancer Institute.
Competing interests: None declared.