Abstract
OBJECTIVES: To assess the prevalence and persistence of depression in patients with acute myocardial infarction (AMI) and the relationship between assessment modality and prevalence.
DATA SOURCES: MEDLINE®, Cochrane, CINAHL®, PsycINFO®, and EMBASE®.
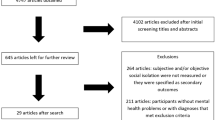
REVIEW METHODS: A comprehensive search was conducted in March 2004 to identify original research studies published since 1980 that used a standardized interview or validated questionnaire to assess depression. The search was augmented by hand searching of selected journals from October 2003 through April 2004 and references of identified articles and reviews. Studies were excluded if only an abstract was provided, if not in English, or if depression was not measured by a validated method.
RESULTS: Major depression was identified in 19.8% (95% confidence interval [CI] 19.1% to 20.6%) of patients using structured interviews (N=10,785, 8 studies). The prevalence of significant depressive symptoms based on a Beck Depression Inventory score ≥10 was 31.1% (CI 29.2% to 33.0%; N=2,273, 6 studies), using a Hospital Anxiety and Depression Scale (HADS) score ≥8%, 15.5% (CI 13.2% to 18.0%; N=863, 4 studies), and with a HADS score ≥11%, 7.3% (CI 5.5% to 9.3%; N=830, 4 studies). Although a significant proportion of patients continued to be depressed in the year after discharge, the limited number of studies and variable follow-up times precluded specification of prevalence rates at given time points.
CONCLUSIONS: Depression is common and persistent in AMI survivors. Prevalence varies depending on assessment method, likely reflecting treatment of somatic symptoms.
Similar content being viewed by others
References
Frasure-Smith N, Lesperance F, Talajic M. Depression following myocardial infarction. Impact on 6-month survival. JAMA. 1993;270:1819–25.
Carney RM, Blumenthal JA, Catellier D, et al. Depression as a risk factor for mortality after acute myocardial infarction. Am J Cardiol. 2003;92:1277–81.
Lesperance F, Frasure-Smith N, Talajic M, Bourassa MG. Five-year risk of cardiac mortality in relation to initial severity and one-year changes in depression symptoms after myocardial infarction. Circulation. 2002;105:1049–53.
Welin C, Lappas G, Wilhelmsen L. Independent importance of psychosocial factors for prognosis after myocardial infarction. J Intern Med. 2000;247:629–39.
Frasure-Smith N, Lesperance F, Talajic M. Depression and 18-month prognosis after myocardial infarction. Circulation. 1995;91:999–1005.
Bush DE, Ziegelstein RC, Tayback M, et al. Even minimal symptoms of depression increase mortality risk after acute myocardial infarction. Am J Cardiol. 2001;88:337–41.
Ladwig KH, Kieser M, Konig J, Breithardt G, Borggrefe M. Affective disorders and survival after acute myocardial infarction. Results from the post-infarction late potential study. Eur Heart J. 1991;12:959–64.
Kaufmann MW, Fitzgibbons JP, Sussman EJ, et al. Relation between myocardial infarction, depression, hostility, and death. Am Heart J. 1999;138:549–54.
Irvine J, Baker B, Smith J, et al. Poor adherence to placebo or amiodarone therapy predicts mortality: results from the CAMIAT study. Canadian Amiodarone Myocardial Infarction Arrhythmia Trial. Psychosom Med. 1999;61:566–75.
van Melle JP, de Jonge P, Spijkerman TA, et al. Prognostic association of depression following myocardial infarction with mortality and cardiovascular events: a meta-analysis. Psychosm Med. 2004;66:814–22.
Barth J, Schumacher M, Herrmann-Lingen C. Depression as a risk factor for mortality in patients with coronary heart disease: a meta-analysis. Psychosom Med. 2004;66:802–13.
Sorensenf C, Friis-Hasche E, Haghfelt T, Bech P. Postmyocardial infarction mortality in relation to depression: a systematic critical review. Psychother Psychosom. 2005;74:69–80.
Antman EM, Anbe DT, Armstrong PW, et al. ACC/AHA guidelines for the management of patients with ST-elevation myocardial infarction; A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (committee to revise the 1999 guidelines for the management of patients with acute myocardial infarction). J Am Coll Cardiol. 2004;44:E1–211.
Cavanaugh S, Clark DC, Gibbons RD. Diagnosing depression in the hospitalized medically ill. Psychosomatics. 1983;24:809–15.
Morrison MF, Kastenberg JS. Differentiation of secondary from primary mood disorders: controversies and consensus. Semin Clin Neuropsychiatr. 1997;2:232–43.
Sutor B, Rummans TA, Jowsey SG, et al. Major depression in medically ill patients. Mayo Clin Proc. 1998;73:329–37.
First MB, Spitzer RL, Gibbon M, Williams J. Structured Clinical Interview for DSM-IV Axis I Disorders—Patient Edition (SCID-I/P, Version 2.0). New York: Biometrics Research Department, New York State Psychiatric Institute; 1996.
Spitzer RL, Endicott J, Robins E. Research Diagnostic Criteria: rationale and reliability. Arch Gen Psychiatr. 1978;35:773–82.
Robins LN, Helzer JE, Croughan J, Ratcliff KS. National Institute of Mental Health Diagnostic Interview Schedule. Its history, characteristics, and validity. Arch Gen Psychiatr. 1981;38:381–9.
Beck AT, Steer RA, Garbin MG. Psychometric properties of the Beck Depression Inventory: twenty-five years of evaluation. Clin Psychol Rev. 1988;8:77–100.
Zigmond AS, Snaith RP. The Hospital Anxiety and Depression Scale. Acta Psychiatr Scand. 1983;67:361–70.
Bush DE, Ziegelstein RC, Patel UV, et al. Post-myocardial infarction depression. Evidence Rep Technol Assess (Summ). 2005;1–8.
Berlin JA. Does blinding of readers affect the results of meta-analyses? University of Pennsylvania Meta-Analysis Blinding Study Group. Lancet. 1997;350:185–6.
Atkins D, Eccles M, Flottorp S, et al. Systems for grading the quality of evidence and the strength of recommendations I: critical appraisal of existing approaches. The GRADE working group. BMC Health Serv Res. 2004;4:38.
O’Rourke Á, Hampson SE. Psychosocial outcomes after an MI: an evaluation of two approaches to rehabilitation. Psychol, Health Med. 1999;4:393–402.
Bennett P, Mayfield T. Mood and behaviour change following first myocardial infarction. Coronary Health Care. 1998;2:210–4.
Mayou RA, Gill D, Thompson DR, et al. Depression and anxiety as predictors of outcome after myocardial infarction. Psychosom Med. 2000;62:212–9.
Brink E, Karlson BW, Hallberg LR. Health experiences of first-time myocardial infarction: factors influencing women’s and men’s health-related quality of life after five months. Psychol Health Med. 2002;7:5–16.
Martin CR, Lewin RJ, Thompson DR. A confirmatory factor analysis of the Hospital Anxiety and Depression Scale in coronary care patients following acute myocardial infarction. Psychiatr Res. 2003;120:85–94.
Efron B, Tibshirani R. The bootstrap method for assessing statistical accuracy. Behaviormetrika. 1985;17:1–35.
Platt RW, Hanley JA, Yang H. Bootstrap confidence intervals for the sensitivity of a quantitative diagnostic test. Stat Med. 2000;19:313–22.
Hochberg Y. A sharper Bonferroni procedure for multiple tests of significance. Biometrika. 1988;75:800–3.
Schleifer SJ, Macari-Hinson MM, Coyle DA, et al. The nature and course of depression following myocardial infarction. Arch Intern Med. 1989;149:1785–9.
Carney RM, Freedland KE, Jaffe AS. Insomnia and depression prior to myocardial infarction. Psychosom Med. 1990;52:603–9.
Forrester AW, Lipsey JR, Teitelbaum ML, DePaulo JR, Andrzejewski PL. Depression following myocardial infarction. Int J Psychiatr Med. 1992;22:33–46.
Lesperance F, Frasure-Smith N, Talajic M. Major depression before and after myocardial infarction: its nature and consequences. Psychosom Med. 1996;58:99–110.
Watkins LL, Blumenthal JA, Carney RM. Association of anxiety with reduced baroreflex cardiac control in patients after acute myocardial infarction. Am Heart J. 2002;143:460–6.
Berkman LF, Blumenthal J, Burg M, et al. Effects of treating depression and low perceived social support on clinical events after myocardial infarction: the enhancing recovery in coronary heart disease patients (ENRICHD) randomized trial. JAMA. 2003;289:3106–16.
Lane D, Carroll D, Ring C, Beevers DG, Lip GY. The prevalence and persistence of depression and anxiety following myocardial infarction. Br J Health Psychol. 2002;7:11–21.
Luutonen S, Holm H, Salminen JK, Risla A, Salokangas RK. Inadequate treatment of depression after myocardial infarction. Acta Psychiatr Scand. 2002;106:434–9.
Barefoot JC, Burg MM, Carney RM, et al. Aspects of social support associated with depression at hospitalization and follow-up assessment among cardiac patients. J Cardiopulm Rehabil. 2003;23:404–12.
Lauzon C, Beck CA, Huynh T, et al. Depression and prognosis following hospital admission because of acute myocardial infarction. CMAJ. 2003;168:547–52.
Taylor CB, Houston-Miller N, Ahn DK, Haskell W, DeBusk RF. The effects of exercise training programs on psychosocial improvement in uncomplicated postmyocardial infarction patients. J Psychosom Res. 1986;30:581–7.
Davis T, Jensen L. Identifying depression in medical patients. Image J Nurs Sch. 1988;20:191–5.
Silverstone PH. Changes in depression scores following life-threatening illness. J Psychosom Res. 1990;34:659–63.
Gilutz H, Bar-On D, Billing E, Rehnquist N, Cristal N. The relationship between causal attribution and rehabilitation in patients after their first myocardial infarction. A cross cultural study. Eur Heart J. 1991;12:883–8.
Legault SE, Joffe RT, Armstrong PW. Psychiatric morbidity during the early phase of coronary care for myocardial infarction: association with cardiac diagnosis and outcome. Can J Psychiatr. 1992;37:316–25.
Steeds RP, Bickerton D, Smith MJ, Muthusamy R. Assessment of depression following acute myocardial infarction using the Beck Depression Inventory. Heart. 2004;90:217–8.
Garcia L, Valdes M, Jodar I, Riesco N, de Flores T. Psychological factors and vulnerability to psychiatric morbidity after myocardial infarction. Psychother Psychosom. 1994;61:187–94.
Travella JI, Forrester AW, Schultz SK, Robinson RG. Depression following myocardial infarction: a one year longitudinal study. Int J Psychiatr Med. 1994;24:357–69.
Strik JJ, Honig A, Lousberg R, Denollet J. Sensitivity and specificity of observer and self-report questionnaires in major and minor depression following myocardial infarction. Psychosomatics. 2001;42:423–8.
Lesperance F, Frasure-Smith N, Theroux P, Irwin M. The association between major depression and levels of soluble intercellular adhesion molecule 1, interleukin-6, and C-reactive protein in patients with recent acute coronary syndromes. Am J Psychiatr. 2004;161:271–7.
Trelawny-Ross C, Russell O. Social and psychological responses to myocardial infarction: multiple determinants of outcome at six months. J Psychosom Res. 1987;31:125–30.
Follick MJ, Gorkin L, Smith TW, Capone RJ, Visco J, Stablein D. Quality of life post-myocardial infarction: effects of a transtelephonic coronary intervention system. Health Psychol. 1988;7:169–82.
Clarke DE, Walker JR, Cuddy TE. The role of perceived overprotectiveness in recovery 3 months after myocardial infarction. J Cardiopulm Rehabil. 1996;16:372–7.
Lehto S, Koukkunen H, Hintikka J, Viinamaki H, Laakso M, Pyorala K. Depression after coronary heart disease events. Scand Cardiovasc J. 2000;34:580–3.
Shiotani I, Sato H, Kinjo K, et al. Depressive symptoms predict 12-month prognosis in elderly patients with acute myocardial infarction. J Cardiovasc Risk. 2002;9:153–60.
Blazer DG, Kessler RC, McGonagle KA, Swartz MS. The prevalence and distribution of major depression in a national community sample: the National Comorbidity Survey. Am J Psychiatr. 1994;151:979–86.
Burvill PW. Recent progress in the epidemiology of major depression. Epidemiol Rev. 1995;17:21–31.
Burvill PW, Johnson GA, Jamrozik KD, Anderson CS, Stewart-Wynne EG, Chakera TM. Prevalence of depression after stroke: the Perth community stroke study. Br J Psychiatr. 1995;166:320–7.
Robinson RG, Starr LB, Price TR. A two year longitudinal study of mood disorders following stroke. Prevalence and duration at six months followup. Br J Psychiatr. 1984;144:256–62.
Cassidy E, O’Connor R, O’Keane V. Prevalence of post-stroke depression in an Irish sample and its relationship with disability and outcome following inpatient rehabilitation. Disabil Rehabil. 2004;26:71–7.
Astrom M, Adolfsson R, Asplund K. Major depression in stroke patients. A 3-year longitudinal study. Stroke. 1993;24:976–82.
Kurlowicz LH, Streim JE. Measuring depression in hospitalized, medically ill, older adults. Arch Psychiatr Nurs. 1998;12:209–18.
Koenig HG, Cohen HJ, Blazer DG, Krishnan KR, Sibert TE. Profile of depressive symptoms in younger and older medical inpatients with major depression. J Am Geriatr Soc. 1993;41:1169–76.
Koenig HG, George LK, Peterson BL, Pieper CF. Depression in medically ill hospitalized older adults: prevalence, characteristics, and course of symptoms according to six diagnostic schemes. Am J Psychiatr. 1997;154:1376–83.
American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 4th ed. Washington, DC: American Psychiatric Association; 1994.
Snaith RP. The Hospital Anxiety and Depression Scale. Health Qual Life Outcomes. 2003;1:29.
Ruo B, Rumsfeld JS, Hlatky MA, Liu H, Browner WS, Whooley MA. Depressive symptoms and health-related quality of life: the heart and soul study. JAMA. 2003;290:215–21.
Serebruany VL, Glassman AH, Malinin AI, et al. Enhanced platelet/endothelial activation in depressed patients with acute coronary syndromes: evidence from recent clinical trials. Blood Coagul Fibrinolysis. 2003;14:563–7.
Ziegelstein RC, Fauerbach JA, Stevens SS, Romanelli J, Richter DP, Bush DE. Patients with depression are less likely to follow recommendations to reduce cardiac risk during recovery from a myocardial infarction. Arch Intern Med. 2000;160:1818–23.
Glassman AH, O’Connor CM, Califf RM, et al. Sertraline treatment of major depression in patients with acute MI or unstable angina. JAMA. 2002;288:701–9.
Author information
Authors and Affiliations
Corresponding author
Additional information
The authors have no conflicts of interest to report.
This article is based on research conducted by the Johns Hopkins University Evidence-based Practice Center under contract to the Agency for Healthcare Research and Quality (Contract No. 290-02-0018), Rockville, Md. The authors of this article are responsible for its contents, including any clinical or treatment recommendations. No statement in this article should be construed as an official position of the Agency for Healthcare Research and Quality or of the U.S. Department of Health and Human Services.
Rights and permissions
About this article
Cite this article
Thombs, B.D., Bass, E.B., Ford, D.E. et al. Prevalence of depression in survivors of acute myocardial infarction. J GEN INTERN MED 21, 30–38 (2006). https://doi.org/10.1111/j.1525-1497.2005.00269.x
Received:
Revised:
Accepted:
Issue Date:
DOI: https://doi.org/10.1111/j.1525-1497.2005.00269.x